Feature | Cardiopsychology: Exploring the Heart/Brain Connection in Cardiovascular Disease
Psychological stress and mental health concerns are both risk factors for and possible complications of cardiovascular disease (CVD). These connections have been recognized in publications dating back to the 1960s, however relatively little attention is given to this issue day to day.
The field of cardiology has forever been focused on physical health outcomes, like mortality, with a reactive, disease-centered lens. More recently, cardiovascular disease prevention is recognized as an important approach, encouraging healthy lifestyles. Yet even these efforts are centered on diet and exercise, with no mention of mental health in, for example, Life's Simple 7.
Living with cardiovascular disease is stressful for our patients, and substantial mental health burdens have been demonstrated in almost all types of cardiovascular disease, with impacts on metrics such as quality of life, days of missed work and disability.
The Heart/Brain Connection

There are multiple pathways by which psychological stress and mental health problems like anxiety and depression contribute to cardiovascular disease development and associated mortality.1
In this way, the heart and brain are connected and interdependent. Chronic stress results in increased glucocorticoid release, heightened sympathetic nervous system activation, immune dysregulation and endothelial dysfunction.2 Similar pathways have been identified for anxiety and depression.
In response to stress, people tend to engage in unhealthy behaviors, such as poor dietary practices, smoking or lack of exercise, as a means of emotion-focused coping. These and other unhealthy practices like poor medication adherence exacerbate cardiovascular disease risk beyond that imparted by the stress itself.
Although stress can have motivating effects – for example, some people exercise as a way to "burn off" stress – overall, evidence suggests that stress results in less physical activity.2
Stress can also have adverse effects on sleep as a result of increased cortisol levels, which make it harder to fall and stay asleep. This may create a vicious cycle where stress worsens sleep, and lack of sleep increases stress. Over time, chronic stress can lead to insomnia, further increasing cardiovascular disease risk and worsening mental health.
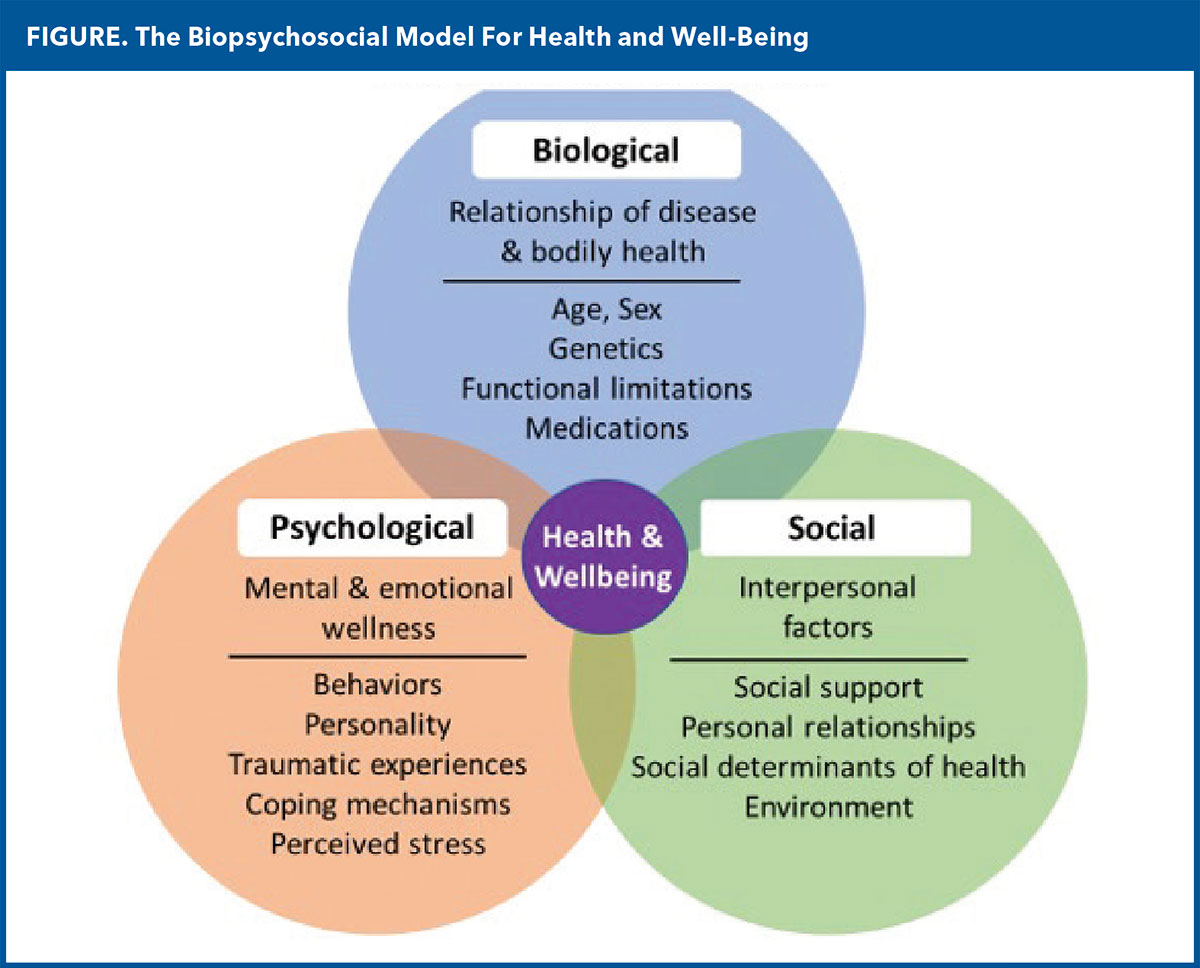
The biopsychosocial model (Figure) is a useful gestalt to help visualize these connections. The model, originally introduced by George Engel in 1977,3 aimed to expand upon the biological focus of the medical model by considering people's lived experiences and the systems in which people reside.
In the biopsychosocial model, a person's biology or risks for illness (e.g., age, sex, genetics, physiological disease processes) interact with psychological factors (e.g., perceived stress) and social factors (e.g., social support, relationship with medical staff, social determinants of health) to impact health and well-being. The heart/brain connection is impacted by factors across the levels of the person's biology, psychology and social environment to ultimately impart cumulative cardiovascular disease risk.
Therefore, when treating cardiovascular disease, considering the entire person is needed to identify the best course of intervention. In many cases, such an approach requires effort from an interdisciplinary team that includes expertise in social work, psychology and/or psychiatry.
Broad Concern Across CVD Groups

These connections between well-being and cardiac health are evident across many types and manifestations of cardiovascular disease. Perhaps the clearest example is that of stress-induced or takotsubo cardiomyopathy, characterized by transient and sometimes severe systolic dysfunction following an acute stressor.1
This neurocardiogenic syndrome is increasingly recognized and often has a dramatic clinical presentation, mimicking acute myocardial infarction (MI). As in MI, typical symptoms include sudden onset of chest pain, breathlessness or collapse. The electrocardiogram and biomarkers are also similar, making it difficult to distinguish between the two conditions on presentation.
Echocardiography will reveal varying degrees of left ventricular dysfunction, in a typical pattern of apical ballooning with basal hypercontractility. The diagnosis is formally made when cardiac catheterization demonstrates unobstructed coronary arteries. Treatment of stress-induced cardiomyopathy is supportive and includes resolving the underlying stressor, as the syndrome is reversible.
In most cases, cardiovascular disease is chronic, with long-lasting effects on physical and emotional health. Major depression affects 20-40% of patients with cardiovascular disease overall,4 and depression is recognized as both a risk factor for and a result of the development of ischemic disease. After an MI, up to 65% of patients report depressive symptoms, and patients with depression are more likely to die than those without.5
Patients with depression and coronary artery disease also have increased morbidity, with worse health-related quality of life, frequent use of health services, higher health-related costs, and decreased likelihood of returning to work after a cardiac event. Similar problems are seen in patients with peripheral artery disease, who also have high rates of depression and negative impacts on wound healing, survival and quality of life.6
Poor mental health has also been noted to be both correlated with as well as a consequence of sudden cardiac death and cardiac arrest. Depression is associated with higher likelihood of out-of-hospital cardiac arrest (OHCA), regardless of age, sex and preexisting heart disease. Although survival from cardiac arrest has improved with contemporary treatments, depression and anxiety are prevalent among survivors and higher than in the general population.
A recent meta-analysis of OHCA survivorship to one year found there was a significant burden of depression and anxiety, and these patients had higher long-term mortality rates than those without anxiety or depression.7
This suggests there are significant mental health gaps that need to be addressed both before and after such events, underscoring the need to improve mental health in addition to physical health outcomes for patients who have suffered and/or are at risk for sudden cardiac death.
A similar story exists in valve disease. This literature is dominated by reports of innovation and breakthroughs, transcatheter interventions, and better survival with experience. While exciting, we have begun to recognize the importance of careful patient selection and shared decision-making given the impacts of uncertainty and frailty on outcomes. But what is rarely mentioned is the psychological and emotional toll that valve disease and its interventions can have on patients.
As in many cases, a patient's perception of the severity of their illness drives psycho-emotional and quality of life outcomes. Anxiety and depression have been described among those whose quality of life is significantly diminished by their valve disease, with anxiety most prevalent peri-operatively.8
After intervention, these are expected to improve. However, they may also persist or be replaced with, for example, post-traumatic stress, which can impact functional recovery despite procedural success.
These connections are also prevalent in patients who do not have acquired, but rather congenital heart disease. Rates of anxiety and depression in congenital heart disease are similar or higher than that of the general population, ranging from 31-33% for mood disorders like depression and 26-28% for anxiety.9

This can be explained by the high prevalence of risk factors for mental health challenges that are present across the lifespan for people with congenital heart disease, particularly those with more complex cardiac lesions. Biological factors that impact early brain development, including changes in fetal circulation, an altered placental environment and early surgical intervention are then met with additional psychosocial challenges after birth.
Significant parental anxiety, neurodevelopmental delays impacting school performance and social functioning, exposure to traumatic medical interventions and hospitalizations, and uncertainty about one's illness course all have the potential to contribute to poor mental health in this population. Moreover, as people with congenital heart disease age, they are at additional risk for developing acquired heart disease, further adding to these multifaceted stressors.
For all of these cardiovascular disease groups, maximizing mental and psychosocial health is as important as physical health. When cardiovascular disease progresses toward death, the end of life, understandably, can be a distressing time for both patients and their families.
Worrying, feeling irritable and anxiety are common, especially as related to undertreated breathlessness and pain. Depression can add to the distress of those whose conditions deteriorate slowly enough and who feel increasingly isolated or lose their independence.
While whole-person care,10 including spiritual and psychosocial needs, is the expectation of patients and families, many clinicians feel ill-equipped to tend to these concerns. The recognition and management of psychological distress is an important clinical skill, and there is an urgent need for research that results in effective interventions to support the emotional health of patients with end-stage cardiovascular disease.
Employing palliative care methods in the treatment of advanced heart failure is one way to achieve this critical support, whether it be primary palliative care provided by the cardiology clinician or specialty palliative care provided in consultation.
Taking Action to Support Well-Being

Despite all of this evidence, mental health concerns like depression and anxiety are rarely diagnosed or treated in the cardiology setting. Assessment is uncommon in clinical encounters, even though these concerns exist hand-in-hand with and lead to similarly poor outcomes as leading cardiovascular disease risk factors like smoking, high cholesterol and hypertension.
Psychotherapy and pharmacologic treatments appear to be safe and effective options in patients with cardiovascular disease, so clinicians must make an effort to identify stress and mental health concerns, as they would any consequential comorbid condition.
Incorporating a simple screening tool, such as the PHQ-4, into office intake forms is one way that cardiovascular disease clinicians can efficiently risk stratify patients. This tool asks two questions about symptoms common to depression and two for anxiety, taking less than five minutes to administer.
An elevated score does not diagnose a psychiatric condition, but it is an indicator that further evaluation, such as by a primary care provider or mental health professional, is needed. This implies the need for reliable access to such providers, in which health systems should invest.
Awareness of the importance of stress and mental health comorbidities in cardiovascular disease is needed at the professional level to encourage cardiovascular disease clinicians to consider patients' emotional and psychological well-being in their treatment plans.
There is also a need for rigorous research into the prevention, identification, and management of stress and mental health conditions in the context of cardiovascular disease to combat subjectivity, stigma and clinical inertia.
Other patient populations have experienced better long-term outcomes with consideration and treatment of such concerns, which could certainly translate into better cardiovascular prognoses as well.
The ACC has invested in the importance of the heart/brain connection through the recent establishment of the Cardiovascular Psychology Work Group. This interprofessional group with representation from psychologists, cardiologists and APPs will drive innovation in this space, leading to the development of actionable and sustainable mental health resources that will maximize the physical, mental and emotional well-being of patients with cardiovascular disease.





This article was authored by Jill M. Steiner, MD, MS, FACC, Division of Cardiology and Cambia Palliative Care Center of Excellence, University of Washington, Seattle; Jamie L. Jackson, PhD, Center for Biobehavioral Health, Abigail Wexner Research Institute at Nationwide Children's Hospital, Columbus, OH; Onyedika Ilonze, MD, MPH, FACC, Division of Cardiovascular Medicine, Krannert Cardiovascular Research Center, Indiana University, Indianapolis; Laura Ross, PA-C, AACC, Park Nicollet Heart and Vascular Center, Methodist Hospital, St. Louis Park, MN; and Rosy Thachil, MD, FACC, Division of Cardiology, Elmhurst Hospital/Mount Sinai College of Medicine, New York, NY. All are members of ACC's Cardiovascular Psychology Work Group.
References
- Steptoe A, Kivimäki M. Stress and cardiovascular disease. Nat Rev Cardiol 2012;9:360-70.
- Osborne MT, Shin LM, Mehta NN, et al. Disentangling the links between psychosocial stress and cardiovascular disease. Circ Cardiovasc Imaging 2020;13:e010931.
- Engel GL. The need for a new medical model: A challenge for biomedicine. Science 1977;196:129-36.
- Celano CM, Huffman JC. Depression and cardiac disease: A review. Cardiol Rev 2011;19:130-42.
- Wei J, Rooks C, Ramadan R, et al. Meta-analysis of mental stress-induced myocardial ischemia and subsequent cardiac events in patients with coronary artery disease. Am J Cardiol 2014;114:187-92.
- Welch KG, Faria I, Browder SE, et al. Depression in patients with peripheral artery disease: An underdiagnosis with increased mortality. Ann Vasc Surg 2023;95:80-6.
- Lee J, Cho Y, Oh J, et al. Analysis of anxiety or depression and long-term mortality among survivors of out-of-hospital cardiac arrest. JAMA Netw Open 2023;6:E237809.
- Olsson K, Näslund U, Nilsson J, Hörnsten Å. Experiences of and coping with severe aortic stenosis among patients waiting for transcatheter aortic valve implantation. J Cardiovasc Nurs 2016;31:255-61.
- Kovacs AH, Brouillette J, Ibeziako P, et al. Psychological outcomes and interventions for individuals with congenital heart disease: A scientific statement from the American Heart Association. Circ Cardiovasc Qual Outcomes 2022;15:e000110.
- Selman L, Beynon T, Higginson IJ, Harding R. Psychological, social and spiritual distress at the end of life in heart failure patients. Curr Opin Support Palliat Care 2007;1:260-6.
Clinical Topics: Prevention, Stress
Keywords: Cardiology Magazine, ACC Publications, Depression, Social Determinants of Health, Mental Health, Stress, Psychological, Risk Factors, Psychiatry
