Assessment of Coronary Arteries in Children
Introduction
Coronary artery assessment is essential when certain diseases such as anomalous aortic origin of a coronary artery (AAOCA), intramyocardial (IM) coronary arteries/myocardial bridges or Kawasaki disease are suspected, or during routine surveillance after cardiac transplantation or repair of congenital heart disease. Most imaging modalities require patients to lay still. Thus, sedation for invasive procedures or those with lengthy acquisition times is necessary in children. Invasive angiography by cardiac catheterization can be challenging in small coronary arteries, but it has been safely performed in recent years.
Noninvasive Imaging
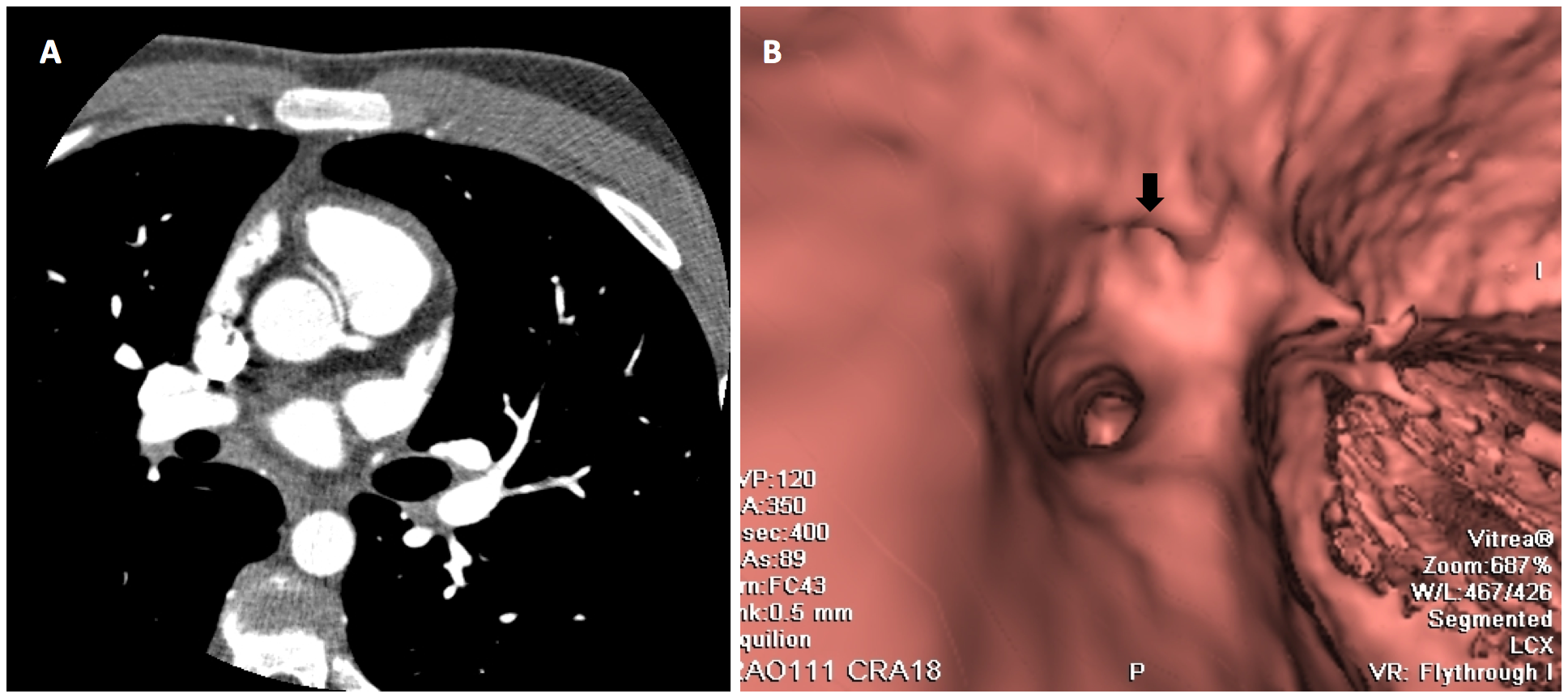
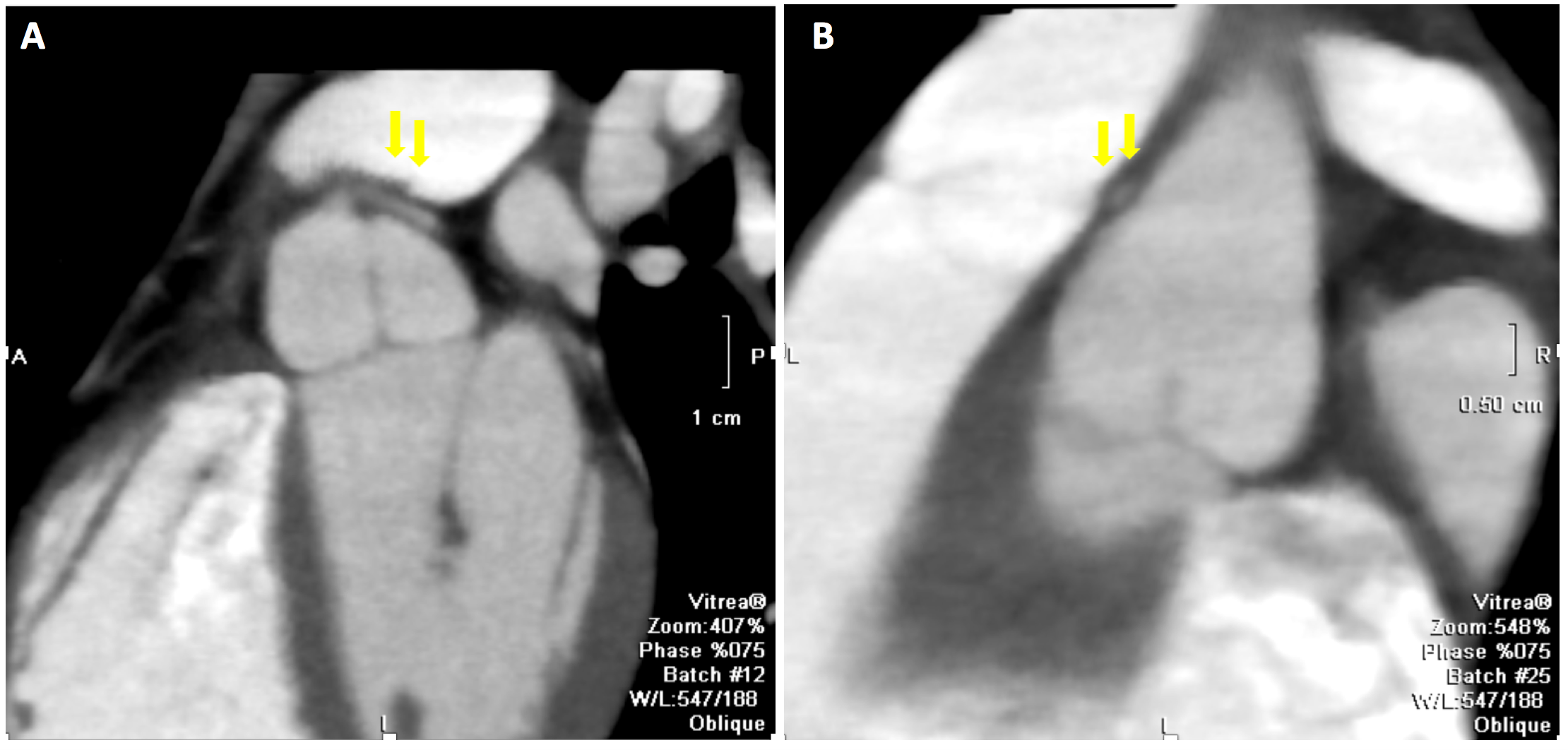
Echocardiography is the initial modality employed in the assessment of proximal coronary arteries in children (Video 1).1 However, echo images may be sub-optimal in older patients with high body mass indices. Improved resolution and precise details of coronary anatomy may be obtained by computed tomography angiography (CTA) with virtual angioscopy (Figure 1) and magnetic resonance imaging (MRI). At Texas Children's Hospital (TCH), CTA has been the procedure of choice to define coronary anatomy and course.2 Complemented with virtual angioscopy, CTA can determine the spatial relationship of the coronary ostia to the aortic sinus (Figure 1).2 The presence and length of the intramural course can be determined by assessing the cross-sectional shape of the coronary lumen and the "pericoronary fat sign." In the former, the mediastinal segment has a round lumen, while the intramural segment is ovoid. In the latter, a thin wall of soft-tissue density appears grey in the intramural segment, while the mediastinal segment is surrounded by low-density fat which appears black (Figure 2). These details are useful for risk stratification and for surgical planning.
Video 1
Figure 1
Figure 2
Myocardial Functional Imaging
Modalities that assess myocardial function and perfusion at rest and during stress, such as stress nuclear perfusion imaging (sNPI), stress echocardiography and stress cardiac MRI (sCMR) are important tools that may aid in clinical decision making.3 Cardiac nuclear perfusion imaging with Thallium-201 was first used in children over three decades ago, but did not attain widespread use due to lower spatial resolution, higher cost, and artifact accumulation in the lungs and liver.4-6 Intravenous 99mTc sestamibi administration at rest and at peak exercise has been the method of choice for performance of sNPI at TCH. However, this modality is fraught with recurrent problems with false positive and false negative results.3
Stress CMR using various agents such as adenosine, dipyridamole, regadenoson, and dobutamine can be safely performed in children with congenital heart disease.7 Compared to sNPI, sCMR may be more reliable in assessing myocardial perfusion in children with AAOCA.3 Hence, sCMR has replaced sNPI study for assessment of myocardial perfusion at our institution, unless a contraindication precludes performing the study.
Stress echocardiography has been performed for over 3 decades in conjunction with exercise on a treadmill or cycle ergometer. In patients with contraindication to physical exercise, continuous dobutamine infusion has been used to simulate exercise. In 1980, Alpert at al.8 reported the feasibility of performing stress echocardiography in pediatric patients using a cycle ergometer. Exercise simulation using Dobutamine is the most commonly used stress agent for stress echocardiogram in the current era. Noto et al.9 showed that Dobutamine stress echocardiogram can safely detect coronary artery stenosis in patients with Kawasaki disease. However, a large volume of studies need to be performed to acquire and maintain expertise in detecting wall motion abnormalities in this setting.
Exercise stress test using treadmill or cycle ergometer is another useful test to identify ischemic electrocardiographic changes or symptoms in patients suspected to have coronary lesions. The modified Bruce protocol is used in children and aims to achieve maximal heart rate response and maximum oxygen uptake in 8-12 minutes. It consists of three minute stages of increasing speed and treadmill elevation. Cycle ergometers permit an increasing workload in supine and upright cycling positions.10 Symptoms such as chest pain, syncope, dyspnea, palpitations and dizziness, or EKG changes such as ST depressions or elevations >1mm in limb leads, >2 mm in chest leads, T wave inversions in lateral leads, prominent Q waves or development polymorphic premature ventricular contractions, supraventricular or ventricular tachycardia are considered abnormal.
Although symptoms and noninvasive imaging as described above are commonly used to risk stratify these patients, these studies can be equivocal. In such cases, data from invasive cardiac catheterization with measurement of fraction flow reserve (FFR) and intravascular ultrasound (IVUS) can be helpful in a select group of patients with AAOCA.11,12
Invasive Testing
In general, invasive testing should be considered in:
- Patients with intramyocardial coronary arteries that present with symptoms suggestive of ischemia or with equivocal non-invasive functional testing.
- Patients with AAOCA in which the anatomy is unclear by non-invasive imaging.
- Evaluation of patients after surgical repair of AAOCA and/or myocardial bridges or other congenital heart disease if the results of non-invasive testing are equivocal.
- Kawasaki disease with large or complex coronary artery aneurysms, 6-12 months after acute illness or sooner if clinically indicated.
- Pre-surgical planning of symptomatic patients with Kawasaki disease or if catheter-based intervention is planned.
- Post heart transplant surveillance coronary angiograms.
Coronary Angiography
The first successful selective coronary angiogram was performed in 1958.13 Today, coronary angiography under general anesthesia for younger patients and conscious sedation for older children is not uncommonly performed. Patients are heparinized to achieve activated clotting times of more than 200 seconds. An initial aortic root angiogram is obtained to define the origin of the coronary arteries, aid in the selection of appropriate catheters and identify severe ostial stenosis which may cause hemodynamic instability when engaged. The choice of catheters is dictated by the sinus from which the anomalous coronary artery arises; for example, in anomalous right coronary artery from the left cusp, a Judkins left or Amplatz left coronary catheter or guiding catheters will likely be successful in engaging the coronary artery.
Fractional Flow Reserve
FFR is the ratio of pressure in the coronary artery distal to the stenosis to the aortic pressure. In adults with atherosclerotic coronary artery disease, FFR was reported to be superior to angiography alone in guiding percutaneous coronary interventions.14
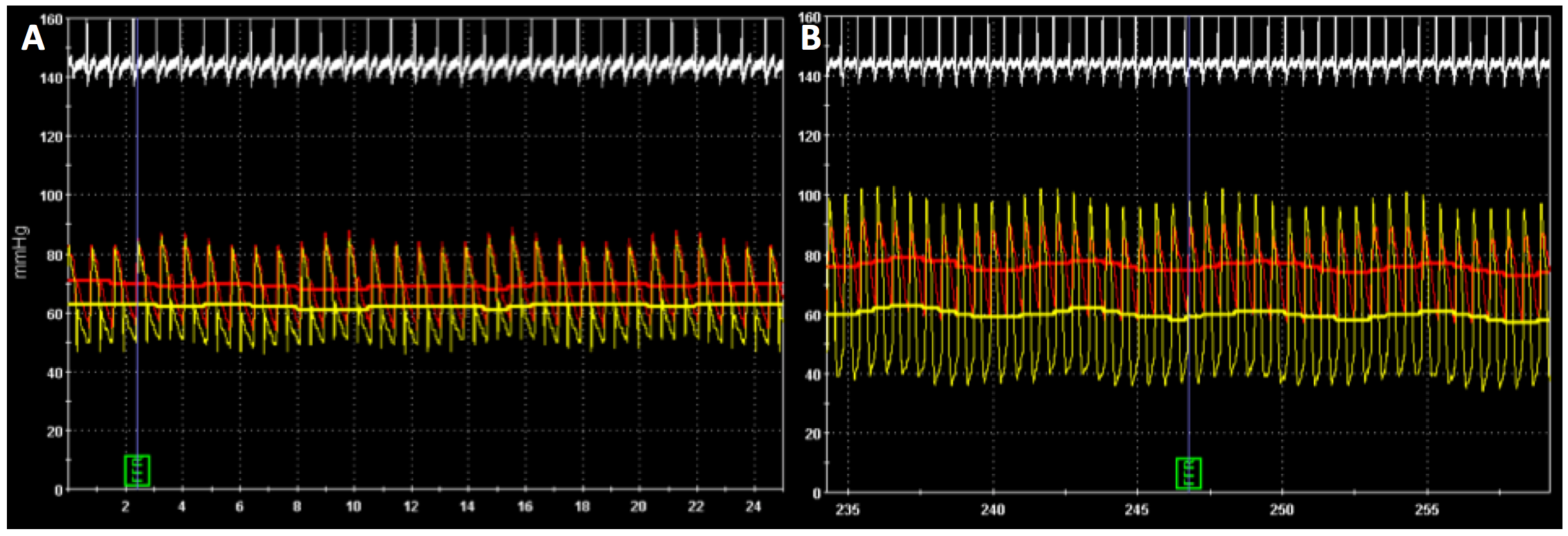
When obtaining FFR in children, intracoronary nitroglycerine is administered to prevent coronary spasm prior to advancing FFR wires or IVUS catheters. It is measured at baseline and again after provocative testing with adenosine infusion for 3 min followed by dobutamine infusion to achieve a heart rate of at least 75% of maximal heart rate (Figure 3).11,15 Induction of maximal hyperemia with adenosine is preferred for fixed stenosis. However, due to the dynamic nature of compression in IM coronary arteries, dobutamine is preferred to mimic the exercise state. Mean FFR is used to assess fixed stenosis. Diastolic FFR is felt to be more sensitive and specific for assessment of dynamic compression that occurs with IM coronary arteries as it avoids intracoronary overshooting of the systolic pressure with increased inotropy.16 An FFR ≤0.8 is considered positive.
Figure 3
FFR assessment has been found to be useful in assessing coronary artery stenosis pre and post intervention in children with Kawasaki disease.17 It has also been used to evaluate small renal arteries in children to determine if intervention is warranted. Instantaneous wave free-ratio FFR (iFR), which obviates the need for provocative agents like adenosine, has been used in adults, but needs further evaluation in children.
Intravascular Ultrasound
IVUS can be useful to define intraluminal or IM compromise in children in the absence of clear clinical symptoms. In a cohort of 67 adults with right AAOCA,18 IVUS identified proximal intramural stenosis which correlated with ischemic symptoms. It can also assess myocardial bridges and detect altered flow dynamics that suggest atherosclerotic changes proximal to the intramyocardial coronary arteries.19 Virtual histology IVUS has been used to identify atherosclerotic changes in patients with Kawasaki disease.20 IVUS has also been utilized to evaluate patients with Kawasaki disease after coronary interventions.21 Severity of stenosis based on IVUS is reported as a percentage of minimal cross sectional area at the point of worse stenosis compared to distal reference cross sectional area (Video 2). Intraluminal narrowing >70% by IVUS is considered significant.22
Video 2
In a select group of children with AAOCA and/or myocardial bridge, IVUS aids in risk stratification and identification of potential targets for surgical therapy.11,15
Conclusion
Assessment of coronary arteries requires a multidisciplinary team of cardiologists, radiologists and cardiovascular surgeons. Non-invasive imaging with echocardiography, CTA and MRI are the primary tools for evaluating coronary arteries. Functional perfusion imaging with stress CMR, invasive coronary angiograms, FFR and IVUS are other useful modalities that aid in risk stratification and surgical planning. Partnering with adult interventional cardiology colleagues is very important to bring catheter based technology to the care of these pediatric patients.
References
- Van Hare GF, Ackerman MJ, Evangelista JK, et al. Eligibility and disqualification recommendations for competitive athletes with cardiovascular abnormalities: task force 4: congenital heart disease: a scientific statement from the American Heart Association and American College of Cardiology. J Am Coll Cardiol 2015;66:2372-84.
- Agrawal H, Mery CM, Krishnamurthy R, Molossi S. Anatomic types of anomalous aortic origin of a coronary artery: a pictorial summary. Congenit Heart Dis 2017;12:603-6.
- Agrawal H, Mery CM, Krishnamurthy R, et al. Stress myocardial perfusion imaging in anomalous aortic origin of a coronary artery: results following a standardized approach. J Am Coll Cardiol 2016;11:1616.
- Sty JR, Starshak RJ. Thallium-201 myocardial imaging in children. J Am Coll 1985;5:128S-39S.
- Gutgesell HP, Pinsky WW, DePuey EG. Thallium-201 myocardial perfusion imaging in infants and children. Value in distinguishing anomalous left coronary artery from congestive cardiomyopathy. Circulation 1980;61:596-9.
- Finley JP, Howman-Giles R, Gilday DL, Olley PM, Rowe RD. Thallium-201 myocardial imaging in anomalous left coronary artery arising from the pulmonary artery. Applications before and after medical and surgical treatment. Am J Cardiol 1978;42:675-80.
- Noel CV, Krishnamurhty R, Moffett B, Krishnamurthy R. Myocardial stress perfusion magnetic resonance: initial experience in a pediatric and young adult population using regadenoson. Pediatr Radiol 2017;47:280-9.
- Alpert BS, Bloom KR, Olley PM. Assessment of left ventricular contractility during supine exercise in children with left-sided cardiac disease. Br Heart J 1980;44:703-10.
- Noto N, Ayusawa M, Karasawa K, et al. Dobutamine stress echodcardiography for detection of coronary artery stenosis in children with Kawasaki disease. J Am Coll Cardiol 1996;27:1251-6.
- Paridon SM, Alpert BS, Boas SR, et al. Clinical stress testing in the pediatric age group: a statement from the American Heart Association Council on Cardiovascular Disease in the Young, Committee on Atherosclerosis, Hypertension, and Obesity in Youth. Circulation 2006;113:1905-20.
- Agrawal H, Molossi S, Alam M, et al. Anomalous coronary arteries and myocardial bridges: risk stratification in children using novel cardiac catheterization techniques. Pediatr Cardiol 2017;38:624-30.
- Quershi AM, Agrawal H. Catheter-based anatomic and functional assessment of coronary arteries in anomalous aortic origin of a coronary artery, myocardial bridges and Kawasaki disease. Congenit Heart Dis 2017;12:615-8.
- Bruschke AV, Sheldon WC, Shirey EK, Proudfit WL. A half century of selective coronary arteriography. J Am Coll Cardiol 2009;54:2139-44.
- Tonino PA, De Bruyne B, Pijls NH, et al. Fractional flow reserve versus angiography for guiding percutaneous coronary intervention. N Engl J Med 2009;360:213-24.
- Agrawal H, Sexson-Tejtel SK, Qureshi AM, et al. Aborted sudden cardiac death after unroofing of anomalous left coronary artery. Ann Thorac Surg 2017;104:e265-7.
- Escaned J, Cortes J, Flores A, et al. Importance of diastolic fractional flow reserve and dobutamine challenge in physiologic assessment of myocardial bridging. J Am Coll Cardiol 2003;42:226-33.
- Ogawa S, Ohkubo T, Fukazawa R, et al. Estimation of myocardial hemodynamics before and after intervention in children with Kawasaki disease. J Am Coll Cardiol 2004;43:653-61.
- Angelini P, Uribe C, Monge J, Tobis JM, Elayda MA, Willerson JT. Origin of the right coronary artery from the opposite sinus of Valsalva in adults: characterization by intravascular ultrasonography at baseline and after stent angioplasty. Catheter Cardiovasc Interv 2015;86:199-208.
- Ge J, Jeremias A, Rupp A, et al. New signs characteristics of myocardial bridging demonstrated by intracoronary ultrasound and Doppler. Eur Heart J 1999;20:1707-16.
- Mitani Y, Ohashi H, Sawada H, et al. In vivo plaque composition and morphology in coronary artery lesions in adolescents and young adults long after Kawasaki disease: a virtual histology-intravascular ultrasound study. Circulation 2009;119:2829-36.
- Ishii M, Ueno T, Ikeda H, et al. Sequential follow-up results of catheter intervention for coronary artery lesions after Kawasaki disease: quantitative coronary artery angiography and intravascular ultrasound imaging study. Circulation 2002;105:3004-10.
- Groves EM, Seto AH, Kern MJ. Invasive testing for coronary artery disease: FFR, IVUS, OCT, NIRS. Cardiol Clin 2014;32:405-17.
Keywords: Pediatrics, Anesthesia, General, Angiography, Coronary Angiography, Adenosine, Arterial Pressure, Artifacts, Blood Pressure, Cardiac Catheterization, Angioscopy, Chest Pain, Cohort Studies, Conscious Sedation, Constriction, Pathologic, Coronary Aneurysm, Coronary Artery Disease, Coronary Angiography, Coronary Vasospasm, Coronary Stenosis, Cross-Sectional Studies, Coronary Vessels, Dipyridamole, Depression, Dizziness, Dobutamine, Dyspnea, Echocardiography, Echocardiography, Stress, Electrocardiography, Exercise, Exercise Test, Heart Rate, Heart Transplantation, Heparin, Hyperemia, Magnetic Resonance Imaging, Mucocutaneous Lymph Node Syndrome, Oxygen, Patient Care Team, Percutaneous Coronary Intervention, Perfusion Imaging, Purines, Pyrazoles, Renal Artery, Sinus of Valsalva, Syncope, Surgeons, Tachycardia, Ventricular, Thallium, Ventricular Premature Complexes, Technetium Tc 99m Sestamibi, Sports
< Back to Listings