COVID-19: Lessons From the New York City Epicenter
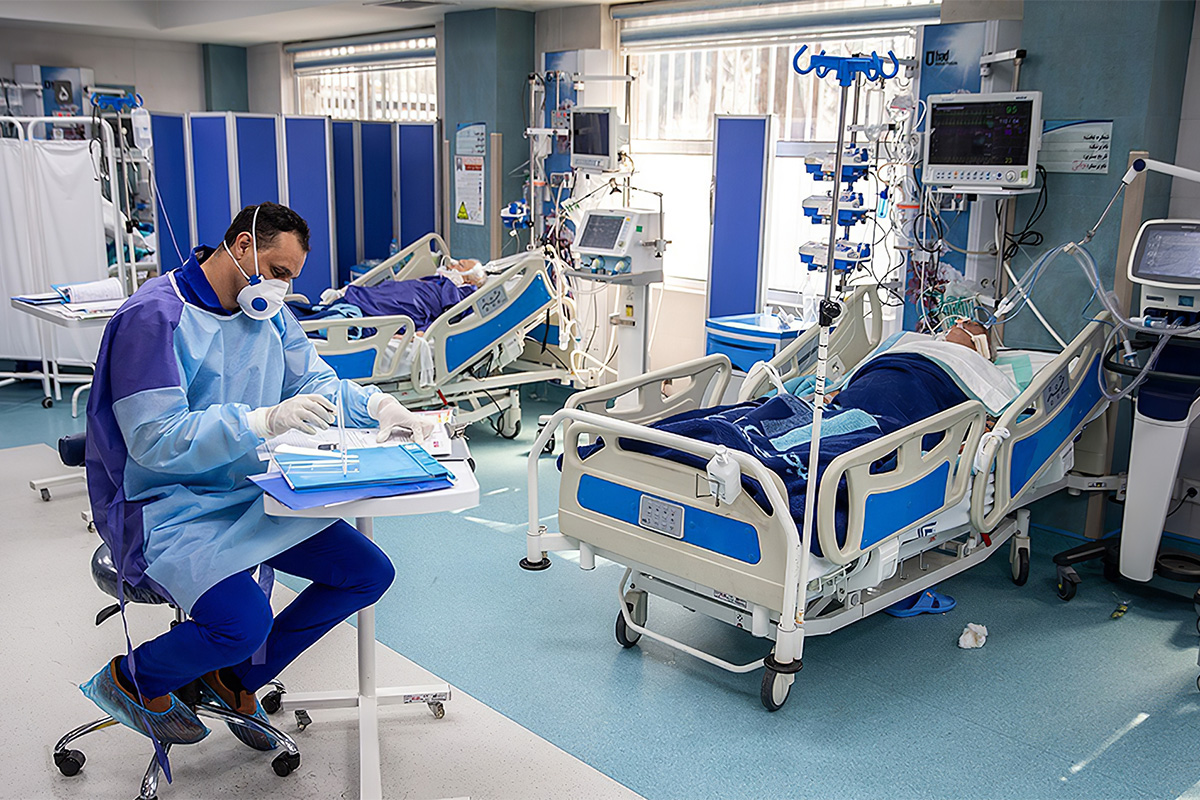
The first case of a pneumonia of unknown cause was reported to the World Health Organization by China on Dec. 31, 2019. Subsequently, news report headlines were dominated by the devastation caused by SARS-CoV2 in China, then Iran and then Italy.
However, these realities felt remote and distant. We knew intrinsically the inherent risks to a densely populated international city such as New York, but we took solace that we had no cases – at least not yet.
Then one day, the air in the hospital was a bit more tense than usual. Whispers started. We had a single case transferred into our system. Suddenly, it was not in our city or country, but our workplace, where we spent more hours than we did at home.
Our colleagues were taking care of this patient.
Our staff was exposed.
Was this an isolated case or just the tip of the iceberg? As details emerged, we very quickly understood it as the latter. Case volume accelerated. The tidal wave was about to hit us. Despite our efforts to prepare for what was to come, we all came to terms with our new reality: the epicenter of the U.S. pandemic.
Be Prepared

To the credit of our institutional leadership, having an early case forced us to prepare early. We started rescheduling at-risk patients for video conferencing even before we had official directives to cancel elective visits. Personal protective equipment (PPE) was in supply, but projections indicated the risk of shortages.
We canceled elective cases in both the operating room and the cardiac catheterization laboratory in short order, not only to preserve PPE but also to mitigate risk of exposure to staff or other patients.
We developed strict protocols to stratify cases by urgency and the circumstances under which cases would proceed. Despite a new electronic medical record, we provided ample education to both physicians and advanced care practitioners on how to successfully perform remote telehealth visits.
Be Flexible
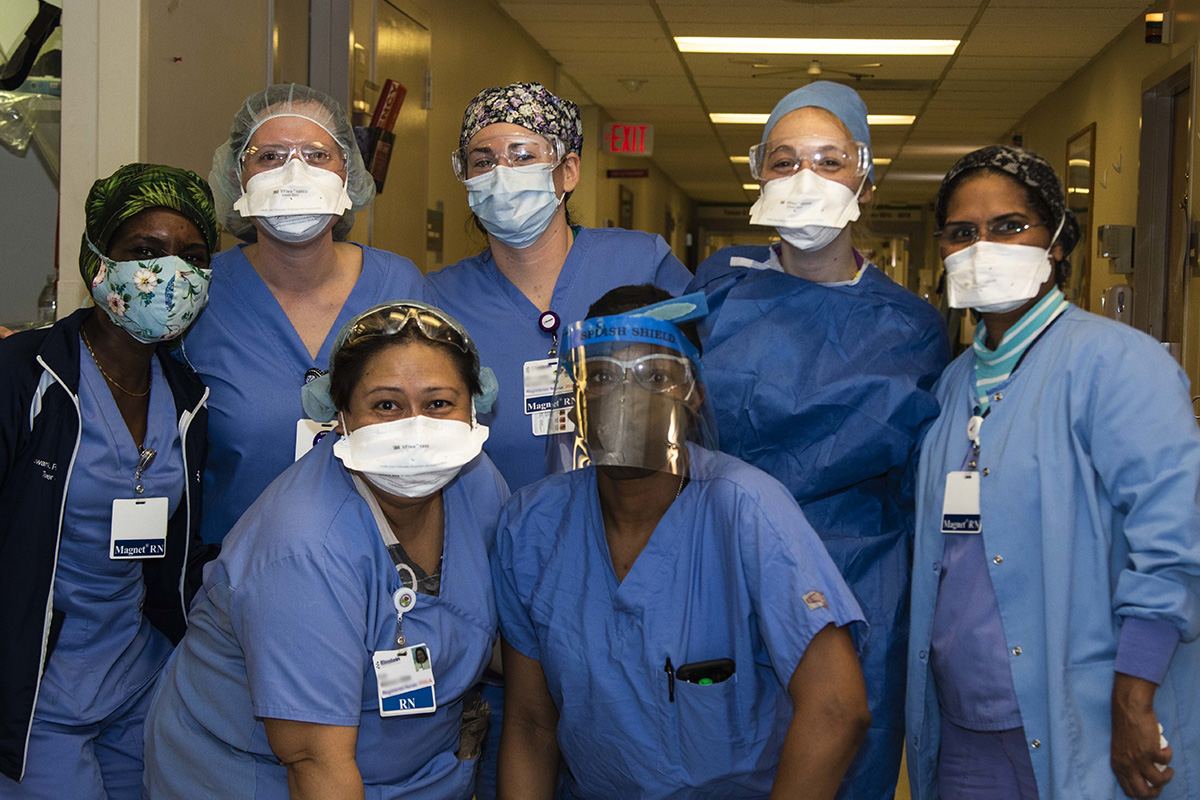
Despite these efforts, the sheer volume of patients was beyond what we could have reasonably expected. Flexibility was key and daily changes were being made both in clinical decisions but also in operations and logistic preparation.
I work in a large academic medical center affiliated with a large multi-hospital network with its inherent advantages of scale and large workforce. Some early career physicians have lead roles in their workplaces despite being a short distance out from training.
Transparency and regular communication is key.
Regular communication and forums to address concerns really help rally the staff and quell latent fears. Furthermore, operational issues will change depending on the clinical needs. Adapting to these challenges may require frequent changes or even reversals of previous statements.
On an individual level, you may be asked to contribute in ways that you previously did not think possible. I never in my life imagined that I would be an attending in the Surgical Intensive Care Unit with an anesthesia fellow, pediatric pulmonary fellow, psychiatry resident and orthopedic surgery intern.
However, we managed our patients as a team, and I learned quite a bit from the multidisciplinary group. Others have manned fever clinics, done shifts in the emergency room or became procedural "fellows." The leadership will need and count on the younger faculty to spearhead many of these makeshift clinical programs and assignments.
Be Available
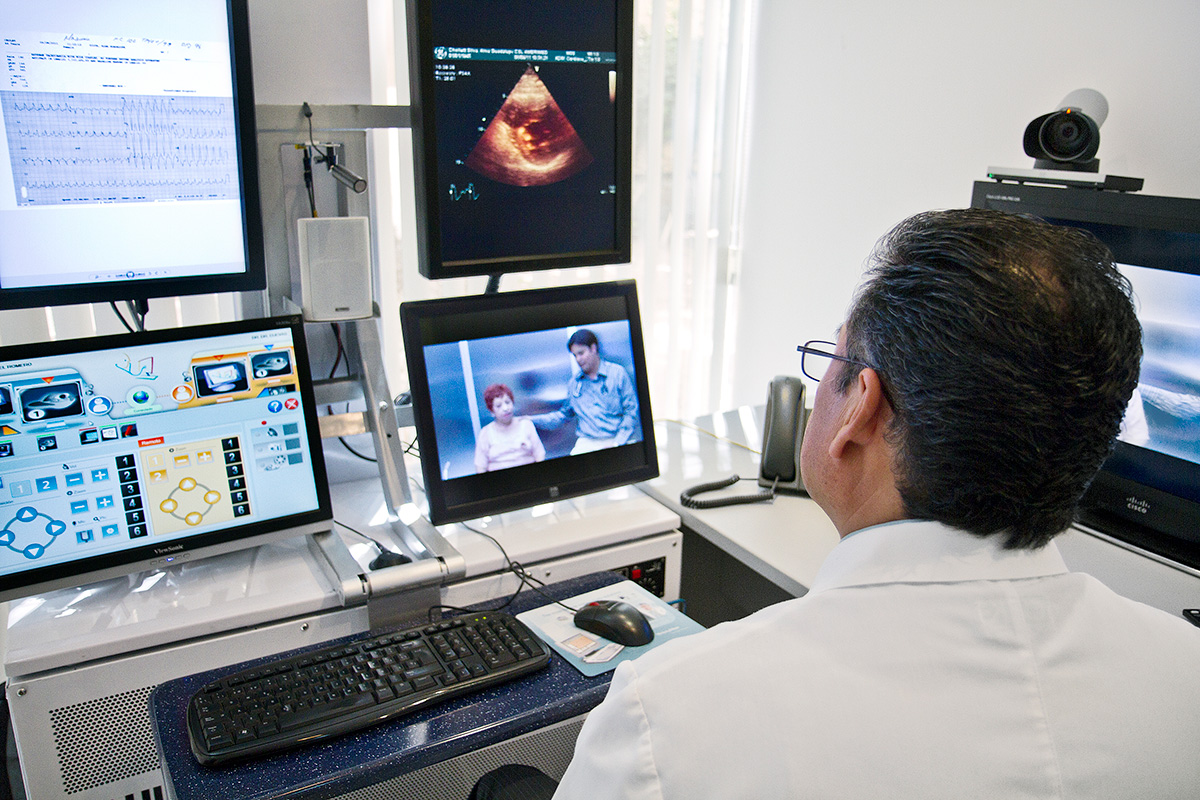
Whether you decide to contribute in patient facing activities, remote clinical activities, logistical/organizational support, research or fundraising, these contributions are key to emerge from this pandemic. The concept of availability extends not just to your workplace but also to your patients.
When not on service, I see patients using video visits both through the EMR and through third-party applications. The patients appreciate the access to their physicians and feel they have a voice to address their concerns.
Be Inquisitive

Our fellows have truly been outstanding in generating research and writing projects. I have been fortunate to work with them. Their energy has been inspiring. In general, research collaborations have blossomed as we recognize the importance of finding treatments for this deadly virus. There are weekly research seminars and daily lectures to update and educate us on both clinical and basic science initiatives.
If you are so inclined, these are excellent opportunities to contribute to science in an impactful way.
While I could have belabored the different initiatives and changes adopted at our institution, this is just a snapshot of the tremendous effort and collaboration needed to face such a pandemic.
However, the most striking feature I have witnessed over the last few weeks has been the sheer humanity and dedication exhibited by people both inside and outside the institution. It is a testament to our collective capabilities when we come together in a time of need.
