Do You Notice It?
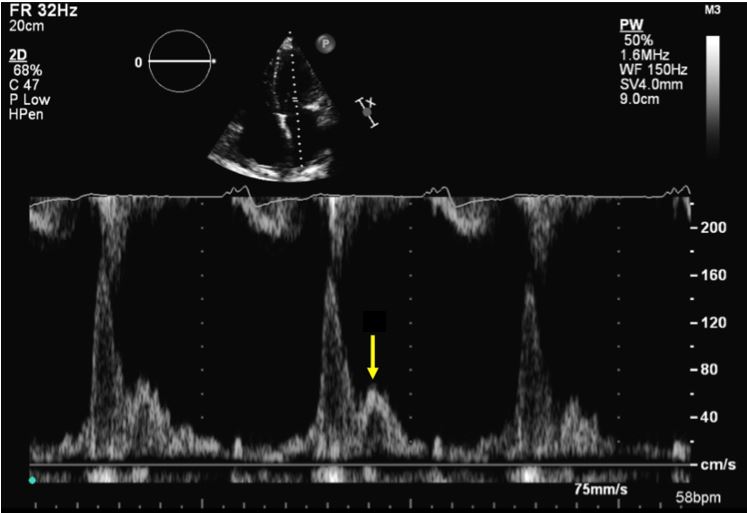
An 87-year-old man with a history of coronary artery disease, diabetes mellitus, atrial fibrillation, moderate aortic stenosis, and diastolic heart failure presented to the cardiology department for an outpatient echocardiogram. He was noted on exam to have significant bilateral lower extremity edema and orthopnea, requiring two pillows during the exam for which a physician was called in to assess the patient. The patient stated that he had 2 weeks of progressively worsening shortness of breath since being discharged after a recent lower gastrointestinal bleed on a lower dose of his furosemide. He was previously able to do his usual activities but now has New York Heart Association Class IV symptoms, with associated paroxysmal nocturnal dyspnea and worsening edema. He denied any chest pain. He was afebrile with a pulse of 60 beats per minute and a blood pressure of 155/100 mmHg. Physical exam was remarkable for jugular venous distention of 10 cm, diffuse bibasilar wheezing on lung exam, a marked S4 on cardiac exam, distension with a positive fluid on abdominal exam, and pitting bilateral lower extremity edema. Pulse-wave Doppler images showed the mitral valve inflow pattern in Figure 1.
Figure 1
In Figure 1, what is the name of the wave marked with the arrow?
Show Answer