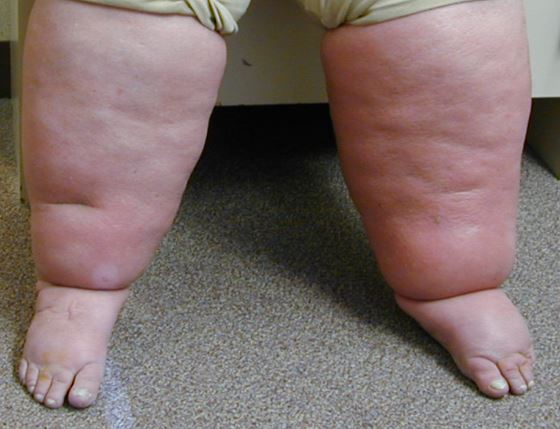
A 73-year-old female was referred for long-standing lower extremity edema. She describes a feeling of heaviness and tightness in her legs with frequent episodes of cellulitis. Her comorbidities include medically complicated obesity, atrial fibrillation, hypertension, and degenerative arthritis in both knees. Her physical examination revealed bilateral lower extremity swelling that included the feet and toes. She has a positive "stemmer" sign with restricted range of motion in her legs with hardening and thickening of the skin (Figure 1). Complete blood count, chemistries, thyroid stimulating hormone, and liver function studies were normal. Venous ultrasound demonstrates patency of the great saphenous vein and small saphenous vein without reflux or incompetence. Sleep study was negative for apneic events. She was diagnosed with lymphedema and prescribed compression garments.
Figure 1
The correct answer is: C. Complete decongestive therapy.
Lymphedema results when the lymphatic system cannot adequately drain lymph fluid.1 The accumulation of lymphatic fluid occurs when there is an interruption of normal lymphatic drainage by various causes (i.e., malignancy, infection, surgical procedures, trauma, etc.) and may lead to swelling, most often in the upper or lower extremity. If the accumulation of lymph fluid is untreated or undertreated, inflammatory lymphatic fluid can lead to a solid phase characterized by fibrotic deposition of fat and fiber in the areas affected by lymphedema. This solid phase is characterized by non-pitting edema and the time frame to transition from fluid to solid phase varies considerably between individuals.1
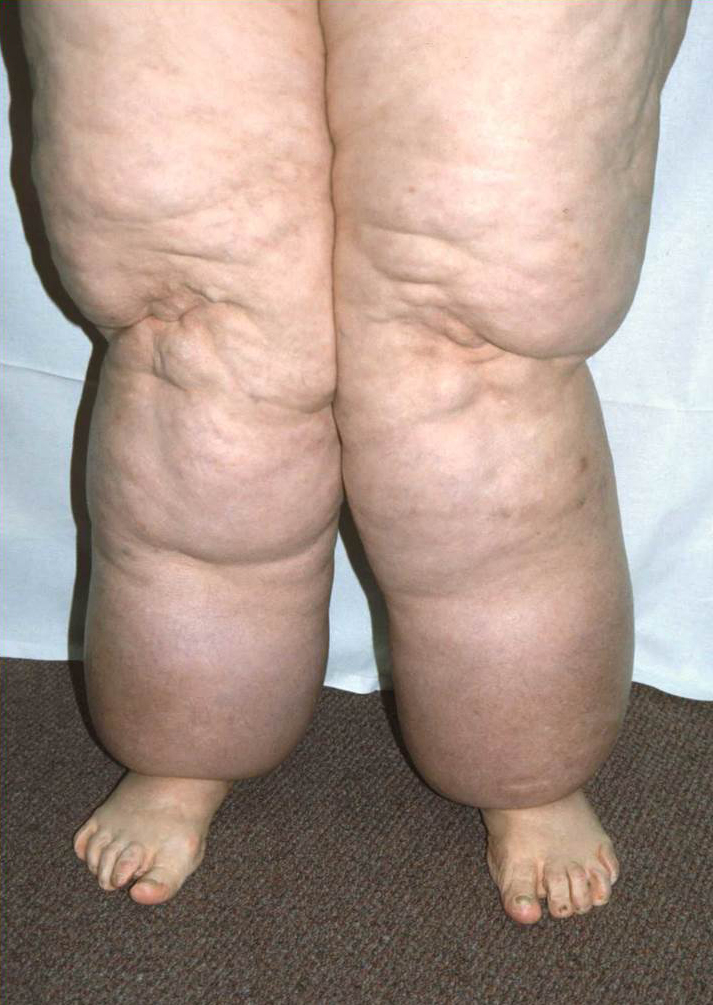
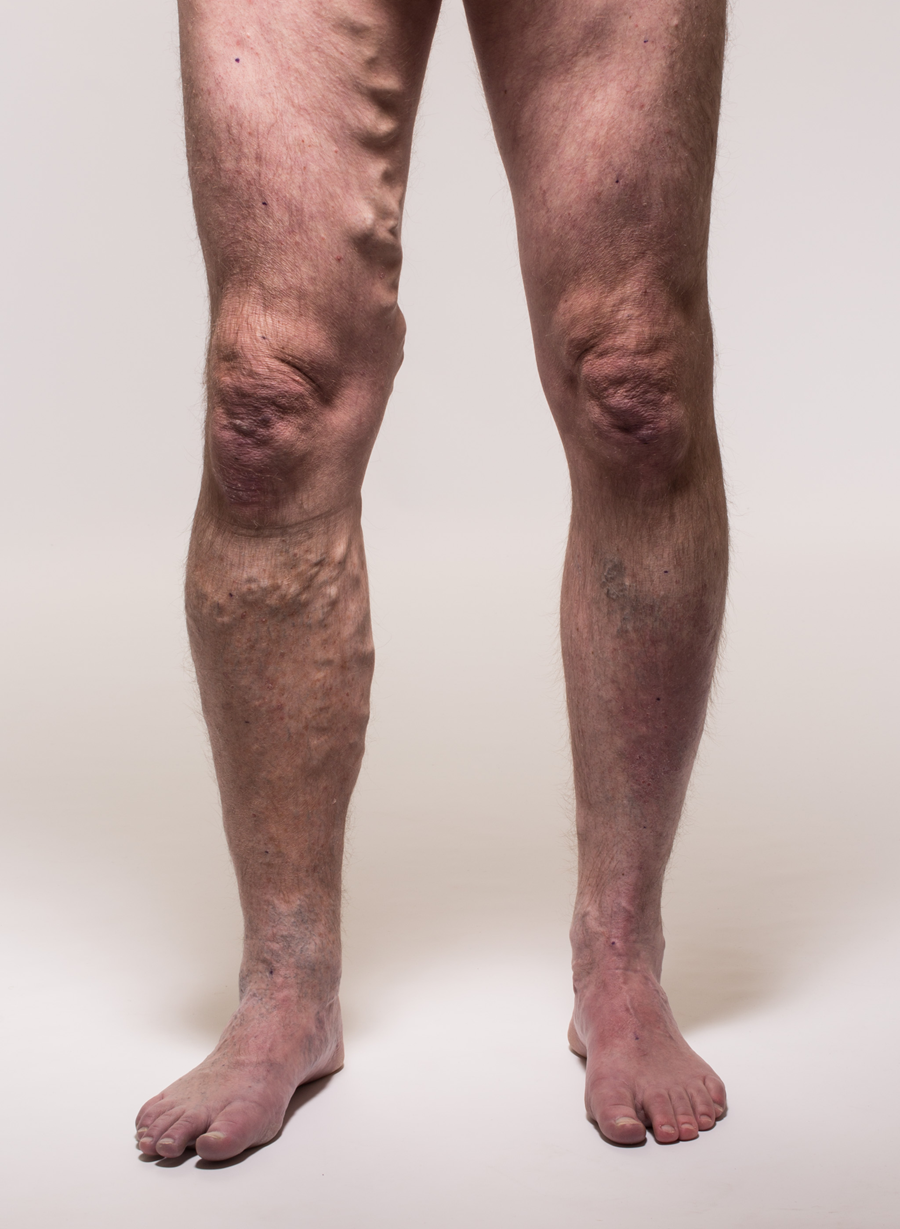
Lymphedema should not be confused with lipedema that is characterized by bilateral, symmetrical fatty tissue excess that extends down towards the ankles where the adipose tissue forms a ring just above the ankle and does not affect the foot or toes (Figure 2).2 Lymphedema of the lower extremity may also be confused with venous insufficiency in which venous blood refluxes in a retrograde fashion due to valvular incompetence (Figure 3) causing swelling of the leg which may lead to skin changes (i.e., hyperpigmentation, induration, erythema, lipodermatosclerosis, etc.) and eventual skin ulceration.2
Figure 2
Figure 3
The mainstay of treatment for lymphedema is conservative nonsurgical therapy.3 Treatment usually starts with compression therapy involving daily wraps and compression. If wrapping alone is not effective for reduction in lymphedema, an approach called complete decongestive therapy may be useful as the next step. This nonsurgical option involves compression therapy and other techniques, such as massage, exercise, and skin care, to encourage the flow of lymph fluid to help reduce swelling.3 In addition, devices that provide low compression therapy, such as a pump that intermittently inflates to provide pressure (e.g., massage) to the affected limb, may be effective.
If improvement with decongestive therapy is not effective, then surgery would likely be the next step in treatment. Three surgical techniques used for lymphedema that are most useful while the individual is still in the fluid stage are vascularized lymph node transfer, lymphaticovenous anastomosis, and lymphaticolymphatic bypass.4,5 The first, vascularized lymph node transfer, releases scar tissue that is blocking the lymph fluid. It also transfers a soft tissue flap from a donor into the affected area. This flap contains lymph system components. The second surgical technique, lymphaticovenous anastomosis, connects existing lymphatic vessels to tiny veins located nearby, allowing the extra lymph fluid to drain directly into the veins. The third approach, lymphaticolymphatic bypass, connects normal functioning lymphatic vessels from a donor directly to the lymphatic vessels of the affected limb.4,5
When lymphedema progresses to the point that solids start to accumulate in the limb, more complex surgical approaches must be used to remove that material. Suction-assisted protein lipectomy (e.g., liposuction) with vascularized lymph node transfer may be effective in managing chronic solid-phase lymphedema.6 This involves aspirating large amounts of solid fat and excess proteinaceous material from the affected area combined with one of the other surgical techniques mentioned earlier to resolve lymphedema.
With proper diagnosis and the appropriate selection of treatment, lymphedema can be treated safely and effectively in many individuals when combined with integrated lymphedema therapy.
References
- Wagner S. Lymphedema and lipedema - an overview of conservative treatment. Vasa 2011;40:271-9.
- Tiwari A, Cheng KS, Button M, Myint F, Hamilton G. Differential diagnosis, investigation, and current treatment of lower limb lymphedema. Arch Surg 2003;138:152-61.
- Lasinski BB, McKillip Thrift K, Squire D, et al. A systematic review of the evidence for complete decongestive therapy in the treatment of lymphedema from 2004 to 2011. PMR 2012;4:580-601.
- Ozturk CN, Ozturk C, Glasgow M, et al. Free vascularized lymph node transfer for treatment of lymphedema: A systematic evidence based review. J Plast Reconstr Aesthet Surg 2016;69:1234-47.
- Granzow JW, Soderberg JM, Kaji AH, Dauphine C. Review of current surgical treatments for lymphedema. Ann Surg Oncol 2014;21:1195-201.
- Brorson H. Liposuction in lymphedema treatment. J Reconstr Microsurg 2016;32:56-65.