A 71-year-old male with a history of hypertension, mild-moderate LVH, non-obstructive CAD, and paroxysmal atrial fibrillation (AF) refractory to pharmacologic suppression with Dofetalide underwent radiofrequency (RF) catheter ablation 9 months ago. Ablation consisted of wide-antral circumferential pulmonary vein isolation (PVI). He did well post-procedure without recurrent AF.
|
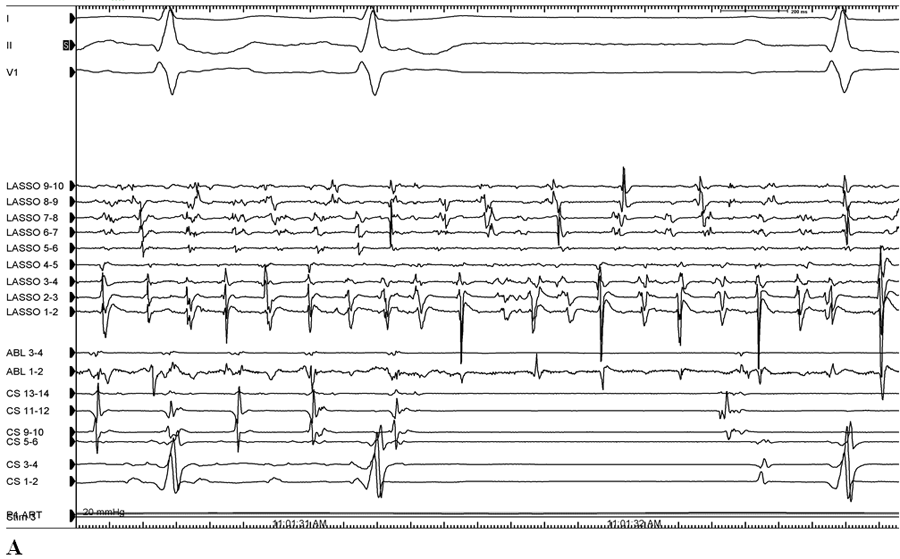
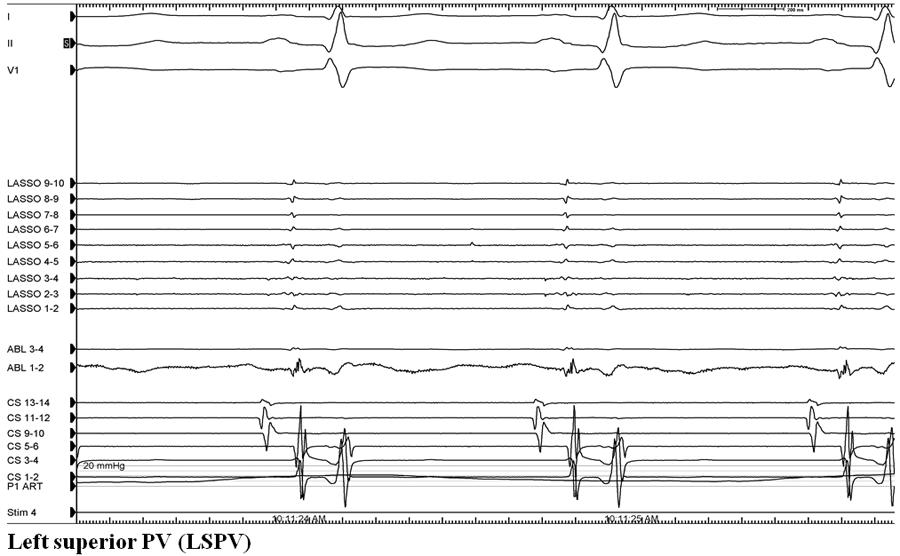
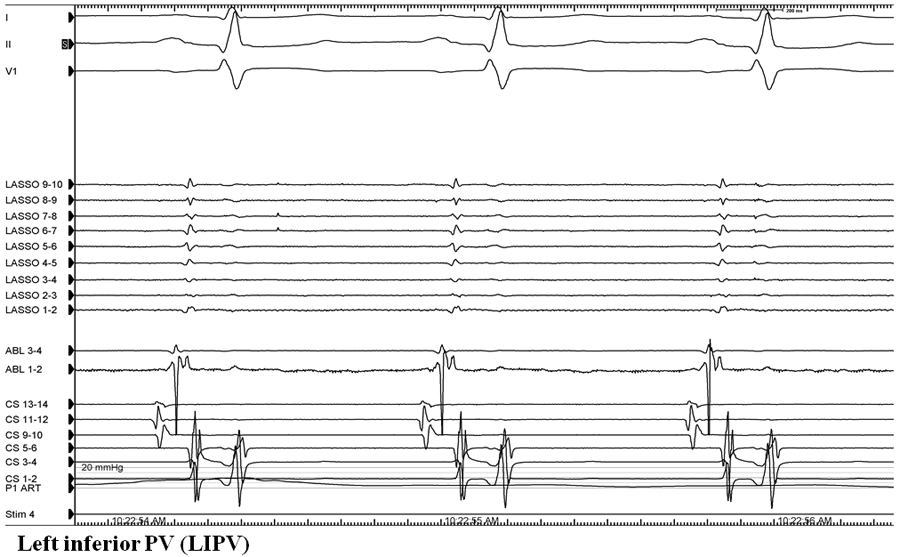
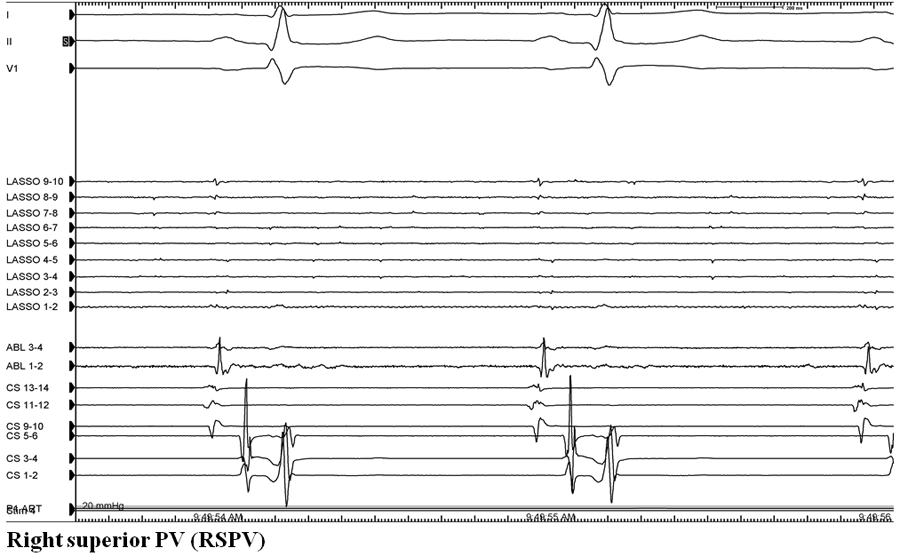
Figure 1: Recordings from the lasso catheter positioned in the ostium of each of the four pulmonary veins. Lasso position was confirmed with intracardiac echo guidance. The ablation catheter is positioned just outside the prior ablation line for each of the four veins. During sinus rhythm, lasso recordings demonstrate no pulmonary vein potentials consistent with entrance block.
|
|

|
|
In follow-up 6 months post-ablation, he had developed recurrent self-limited palpitations and an irregular heart beat. An event monitor confirmed recurrent paroxysms of AF. He was placed back on Dofetalide, but he continued to experience symptomatic arrhythmias lasting several minutes up to 6 hours. An auto-triggered event monitor documented recurrent AF with ventricular rates ranging from 80 to 100 beats per minute.
He was taken back to the EP laboratory for assessment of pulmonary vein isolation and repeat catheter ablation. A circular mapping catheter was placed in each of the four pulmonary veins. All pulmonary veins appeared isolated with evidence of entrance block (Figure 1):
The correct answer is: B. Isoproterenol infusion up to 20 mcg/min.
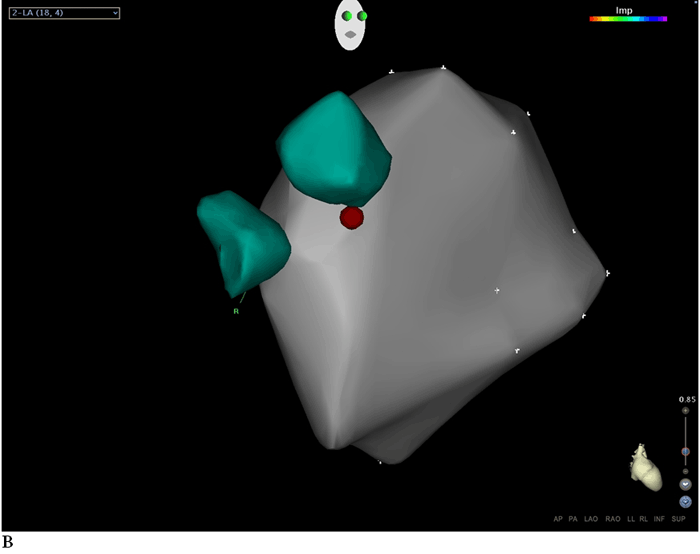
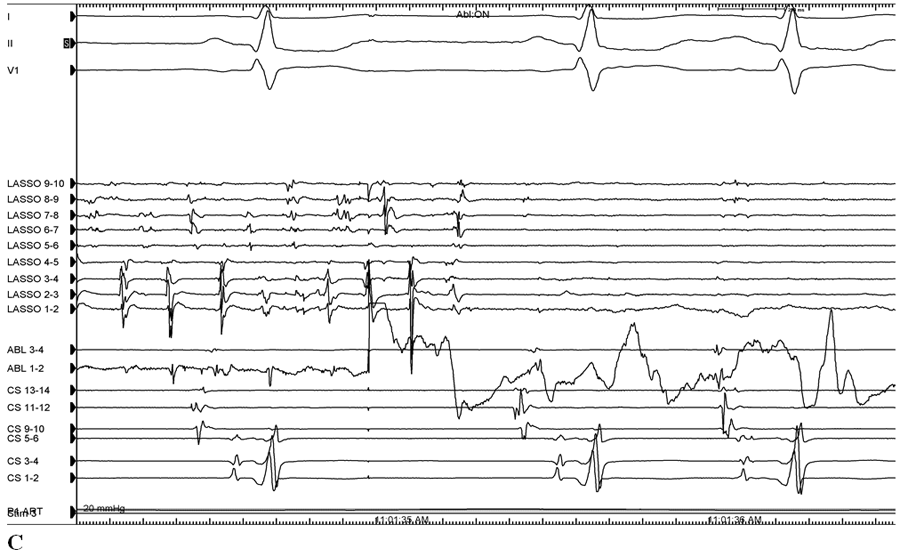
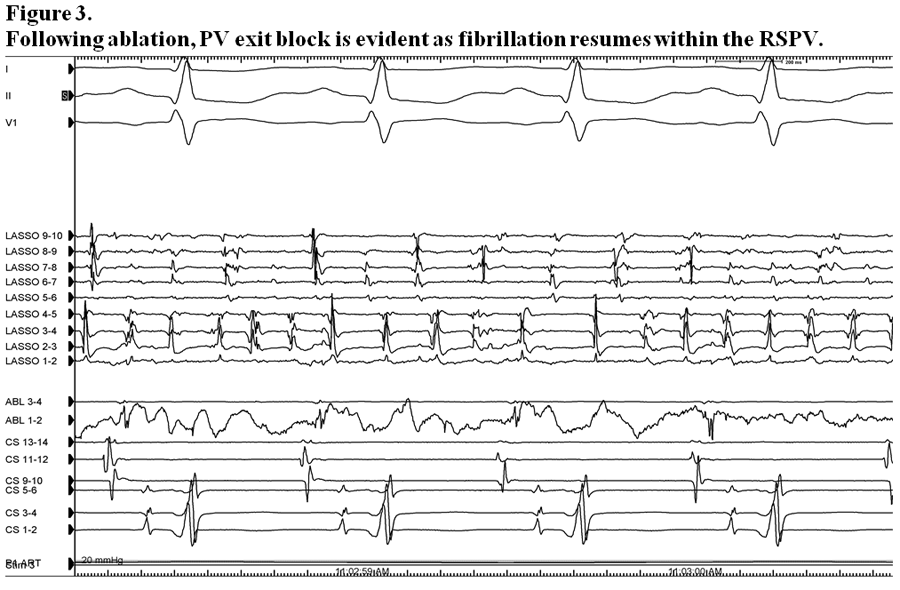
At baseline, all four pulmonary veins (PVs) demonstrated entrance block during sinus rhythm (Figure 1), but exit block had not yet been established. We were unable to observe any spontaneous pulmonary vein firings which would allow us to ascertain the presence of exit block. With isoproterenol infusion to 20 mcg/min, fibrillation originating from the RSPV triggered atrial fibrillation due to the absence of exit block from the vein (Figure 2A). Catheter contact alone resulted in exit block with subsequent termination of AF (Figure 2A). Ablation at a site inferior to the ostium of the RSPV near the anterior carina terminated fibrillation within the RSPV (figure 2B and C). Following ablation, AF resumed within the RSPV, but exit block prevented conduction to the atrium (Figure 3).
Pulmonary vein isolation has been shown to be effective therapy for paroxysmal fibrillation.
(1,2) However, clinical recurrence of AF following ablation is often due to reconnection of previously isolated PVs,
(3,4) and a repeat ablation procedure targeting the reconnected PVs has been shown to improve clinical outcomes.
(4) Since this patient experienced recurrent paroxysms of AF, the likely trigger would be a reconnected PV, and, in this setting, empiric linear ablation and/or CFAE ablation would not be expected to improve the clinical outcome.
Dormant conduction between PVs and the left atrium following ablation predicts recurrence of AF following ablation5. Pharmacologic testing maneuvers with adenosine, isoproterenol, and adenosine + isoproterenol have been used to provoke acute PV-atrial reconnection immediately after ablation.
(5,6,7) Adenosine has shown better efficacy than isoproterenol in unmasking dormant conduction attributed to its superior ability to induce cellular hyperpolarization. Dormant conduction in the acute setting following ablation is attributed to a partially depolarized resting membrane potential with consequent loss of excitability in damaged but not yet dead atrial myocytes.
(8) Following ablation, dormant conduction is typically assessed by demonstration of entrance block (LA to PV) after provocative pharmacologic testing.
In our case, unidirectional conduction block (LA to PV) was present in the RSPV but not immediately discernible with lasso placement in the ostium of the vein during sinus rhythm. Pacing from the lasso catheter positioned within the ostium of the PV could also unmask PV to LA conduction, though capture within the PV is not always reliable. We did not observe spontaneous isolated PV firings in any of the PVs. To demonstrate exit block, pharmacologic testing was necessary to trigger PV firing. In patients with recurrent AF following PVI, isoproterenol infusion up to 20 mcg/min has demonstrated that the majority of AF triggers (54%) originate in previously targeted PVs.
(9) Since many months had elapsed since the initial PVI procedure, dormant conduction would neither have been operative nor have been expected to produce unidirectional conduction block. Therefore, testing with adenosine would not be useful in this case.
Confirmation of bidirectional block of the PV-LA junction has been shown to reduce PV reconnection in the acute setting immediately after ablation.
(10) Confirmation of bidirectional block would be expected to improve long term clinical outcomes following PV isolation.
References
- Jaïs P, Cauchemez B, Macle L, et al. Catheter ablation versus antiarrhythmic drugs for atrial fibrillation. Circulation 2008; 118:2498–2505.
- Wilber DJ, Pappone C, Neuzil P, et al. and the ThermoCool AF Trial Investigators (Comparison of antiarrhythmic drug therapy and radiofrequency catheter ablation in patients with paroxysmal atrial fibrillation: a randomized controlled trial). JAMA 2010; 303:333–340.
- Cappato R, Negroni S, Pecora D, et al. Prospective assessment of late conduction recurrence across radiofrequency lesions producing electrical disconnection at the pulmonary vein ostium in patients with atrial fibrillation. Circulation 2003; 108:1599–1604.
- Nanthakumar K, Plumb VJ, Epstein AE, Veenhuyzen GD, Link D, Kay GN. Resumption of electrical conduction in previously isolated pulmonary veins: rationale for a different strategy? Circulation 2004; 109:1226–1229.
- Arentz T, Macle L, Kalusche D, et al. “Dormant” pulmonary vein conduction revealed by adenosine after ostial radiofrequency catheter ablation. J Cardiovasc Electrophysiol 2004; 15:1041–1047.
- Sauer WH, McKernan ML, Lin D, Gerstenfeld EP, Callans DJ, Marchlinski F. Clinical predictors and outcomes associated with acute return of pulmonary vein conduction during pulmonary vein isolation for treatment of atrial fibrillation. Heart Rhythm 2006; 3:1024–1028.
- Matsuo S, Yamane T, Date T, et al. Reduction of AF recurrence after pulmonary vein isolation by eliminating ATP-induced transient venous re-conduction. J Cardiovasc Electrophysiol 2007; 18:704–708.
- Datino T, Macle L, Qi XY, et al. Mechanisms by which adenosine restores conduction in dormant canine pulmonary veins. Circulation 2010; 121:963–972.
- Gerstenfeld EP, Callans DJ, Dixit S, Zado E, Marchlinski FE. Incidence and location of focal atrial fibrillation triggers in patients undergoing repeat pulmonary vein isolation: implications for ablation strategies. J Cardiovasc Electrophysiol 2003; 14:685-90.
- Chen S, Meng W, Sheng He D, et al. Blocking the Pulmonary Vein to Left Atrium Conduction in Addition to the Entrance Block Enhances Clinical Efficacy in Atrial Fibrillation Ablation. PACE 2012 [Epub ahead of print].