A 74-Year-Old Caucasian Woman With a History of Intermittent Borderline Hypertension
A 74-year-old White woman with a history of intermittent borderline hypertension that resolved with prior weight loss and osteoarthritis comes to see you after the results of her lipid panel. She leads an active lifestyle and wants to remain healthy and keep her risk for cardiovascular events low. Her lipid panel reveals a total cholesterol of 213, an LDL of 140, HDL of 45, and TGs of 140. Her blood pressure is 130/80. Her BMI is 28.5. She walks each day with her dog for 20 minutes, and enjoys a diet that limits red meats, though she does eat a fair amount of saturated fats.
The guideline recommended risk discussion that occurs before a statin prescription in primary prevention should focus on:
Show Answer
The correct answer is: 5) All of the above
Discussion
The new lipid guidelines are still confusing regarding how to best implement this for your patients. You can't easily calculate risk (unless you're a natural log expert) and you're not ready to understand how the practice of lipid management for nearly the past 20 years could change so radically. On top of this, you want to be part of your patient's team and ensure that she is on board and the center of any decision-making. How to proceed?
First, the patient needs to help guide the decision of what to do in this situation. While there may be loads of good quality data, much personal experience, and loads of expert opinions telling you what you must do for your patient, the only one in the room that really matters is your patient and her goals and preferences.
As such, the first step in this situation is to ensure the patient knows what the problem is and how it impacts her life. Cholesterol, for those not medically knowledgeable is an abstract concept. Explaining the basics of atherogenesis and coronary disease along with prognosis is a good way to start. One way to explain the concept that atherosclerosis is to liken it to plumbing, i.e. a process where sludge develops on the supply pipes to the heart as a result of cholesterol deposition along with other risk factors which can result in hardening of the arteries. With these hardened and narrowed arteries, the potential for the demand of the heart muscle to outpace the ability of these diseased arteries to supply nutrients can be exceeded resulting in angina or even a heart attack. Of course, the key with these explanations is to approach it from the perspective of the patient's existing knowledge, level of education, and ability to understand the concepts being presented. Sometimes, using a model, a web site, or an animated graphic (such as on the CardioSmart Explorer app available in the iTunes store) is an easy way to explain abstract disease processes. Once the patient has an understanding of the issue and her risks, the next step is to have a careful discussion about potential treatment options.
|
|||
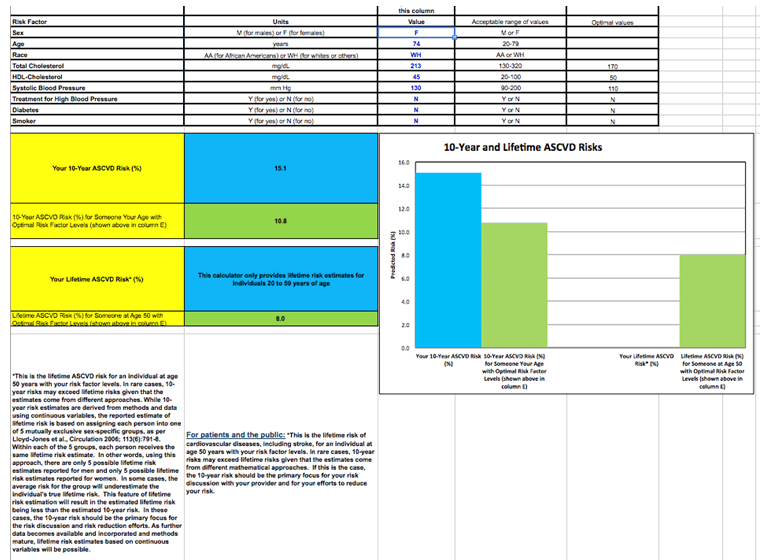
In this case, the patient is a 74-year-old woman without any clinical atherosclerosis or CV disease, but her lifetime risk of CV disease is not really calculable owing to her age (though the calculator suggests 8% for someone with optimal risk factor levels), and her 10-year risk is 15.1%. If she had optimal total cholesterol, systolic blood pressure, and HDL, she would be at 10.1%.
As such, based on the current guidelines, statin therapy could be considered, as could "attaining optimal" factors. However, recent blood pressure guidelines might suggest that treating to optimal blood pressure in this case may not be the best practice.
In any decision for this patient, a careful discussion of lifestyle modification might be in order. For instance, is the patient willing to work on weight loss to get her BMI less than 25? This may help to lower her blood pressure without the need for medicine and lower her lifetime risk. Eating a more plant-based, lower fat diet with less red meat and/or saturated fat might be an option if she was willing to change 74 years of prior habits. Exercising for 30 minutes daily at a brisk pace might be an option, assuming her osteoarthritis would allow this. Exercise alone could lower blood pressure, improve cholesterol, and lower weight.
Regardless, even with "optimal" numbers, this 74 year old woman would still not have a less than 7.5% 10 year risk for events, mostly owing to her age. As such, a careful discussion of statin therapy with its potential side effects, links to diabetes, and a discussion of the "art" of medicine explaining that there are still some areas where there is not enough data to make a firm conclusion. Even with the best clinical trials, no patient is "average" and each is unique and the data might not be generalizable to the person currently in your office. The patient also needs to be able and willing to take a pill each day without any barriers.
Together, with her care providers, and armed with the information derived above, along with knowing her preferences, proclivity towards lifestyle change, and ability to take daily medication a shared decision can be made in a very patient-centered way.
If she opts to take a medication with or without lifestyle modification, follow up visits should focus on compliance, side effects, and education (i.e. understanding the reasons behind the therapy).
Finally, if intensive lifestyle modification is undertaken, an informed decision together with the patient should be made. In this case, even with optimal risk factor profile, her risk for a cardiovascular event is still elevated, but only slightly more than the "threshold" to treat with a statin. As such, after weighing the pros and cons, a provider and the patient might opt against therapy.
The Patient Choice
In this case, the patient opted against further therapy and is working diligently to boost her walking to a goal of two miles covered in 30 minutes five to six days each week. She has opted to eat more plant based and Mediterranean — which has many of the foods she loves to eat. She pledged to give up her pizza night and instead will have a salad when the family goes for pizza.
Conclusion
In short, as you can tell, no medical decision in this setting is necessarily right or wrong. It has to be the right decision for this individual patient at this time with all of her unique considerations.