The patient is a 75-year-old white gentleman with a history of symptomatic paroxysmal atrial fibrillation (AF) and left atrial flutter (AT), who underwent 2 prior radiofrequency ablations in 2008. They included pulmonary venous antral isolation, left atrial roof line, lateral mitral annular isthmus line, and a right atrial cavo-tricuspid isthmus line.
|
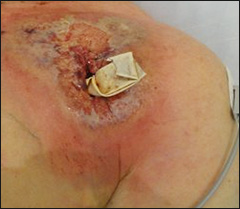
Figure 1: Pain and redness over pacemaker pocket.
|
|
|
He developed recurrent, drug-refractory left atrial tachycardia and presented for a third EP study and RF ablation. In light of a third attempt at controlling his atrial tachyarrhythmia, it was decided to implant a pacemaker with atrial antitachycardia pacing (ATP) capabilities if atrial tachycardia could not be eliminated.
Past Medical History
Paroxysmal symptomatic atrial tachyarrhythmias as described above, one vessel coronary artery disease, dyslipidemia, gout, and thyroid disorder.
EP Procedures
On the day of the procedure, the patient was in atrial tachycardia at a cycle length of 360 ms. This terminated during catheter placement and could not be reproduced. Gaps in the pulmonary veins, LA roof line, and mitral isthmus line were identified and treated with RF energy application empirically. A dual chamber pacer (Medtronic EnRhythm DR) was implanted based on prior discussion. The pacemaker was programmed in the MVP (managed ventricular pacing) mode, with active atrial ATP operation.
Subsequent Course
A week after, the patient presented to the arrhythmia clinic with a two-day history of low-grade fever, pain and redness over the pacemaker pocket. Interrogation of the device showed normal function without recurrent AT.
Physical Exam
VS – HR 86, BP 123/64, RR 16, SaO2 98% on 2 L, and temperature 101.4° F
Neck – 4 cm JVP
Lungs – Clear bilaterally
Left pectoral area – Significant erythema with a yellow exudate, skin exfoliation, and patches of bluish discoloration
CV – Regular S1S2; no appreciated murmur, gallop or rub
Abdomen – Unremarkable
Extremities – Warm, no pitting edema; symmetrical pulses
Neurologic Exam – Normal
Laboratory Values
Hgb: 12.6 (12.9 – 16.9 g/dl)
Platelets: 145 x103 (150 – 350 x103/ul)
WBC: 15.1 x103 (4.5 – 11 x103/ul)
Serum Creatinine: 1.2 (0.6 – 1.5 mg/dl)
Culture and gram stain were acquired from the exudate. The patient was hospitalized and was started on antimicrobial therapy (Vancomycin and Ceftriaxone). The next day, the pacemaker system was explanted and the pocket debrided. A drain was placed. Blood cultures were obtained during fever spikes.
Despite this therapeutic approach, the wound continued to heal extremely poorly and became increasingly erythematous and excoriated (see figure). WBC count rose to 25,000, and temperatures as high as 103° F were recorded. All cultures remained negative and organisms were not seen on gram stain staining.
The correct answer is: C. Punch biopsy of the wound, followed by IV or PO steroids.
With regard to the inflammatory complication that followed the pacemaker implant, the original working diagnosis was acute infection (likely staphylococcal), possibly from suboptimal sterility conditions, although the procedure was carefully reviewed and found to be within our normal standards. Acute pacemaker infection is unusual, estimated to occur in about 0.5% within the first 6-12 months of a new implant, based on US and European series.(1-3) In the case of acute infection, the treatment is device explantation, wound debridement and broad spectrum antibiotics until culture results are available. Staphylococcus species are the most common pathogens (69%).(4) In view of a high prevalence of methicillin-resistant strains among staph aureus and epidermidis, Vancomycin should be invariably used to treat acute device infections.
In our patient, despite adopting such an appropriate strategy for infection, the clinical picture worsened; in addition, exudate culture obtained before starting antibiotics had no bacterial or fungal growth. Blood cultures were sterile, too. This raised the suspicion of a non-infectious condition; therefore answers A and B would be incorrect. In fact, further wound debridement may have madethe wound more inflamed. Latex allergy would not be expected to be limited to the wound site itself, so answer D is incorrect.
The final diagnosis was pyoderma gangrenosum.
Pyoderma gangrenosum (PG) is an ulcerative disease of the skin of unknown origin. The earliest clinical lesion is often a pustule with an inflammatory base. It usually evolves to form shallow or deep ulcers, and can expose underlying tendons or muscle. The ulcers have a purulent base with a ragged, gunmetal colored border that spreads peripherally. PG occurs most commonly on the legs but can develop in any area of the body. Approximately one-half of PG cases are associated with an underlying systemic disease, most commonly inflammatory bowel disease, arthritis, or a lymphoproliferative disorder. PG complicating device implants is unusual but has been reported in some cases.(5-7)
Topical and/or systemic glucocorticoids are generally used first. For lesions that are refractory to glucocorticoids alone, additional treatment options include dapsone, immunomodulators, sulfasalazine and minocycline. Surgical interventions such as skin grafts and/or muscle flaps may be considered for large ulcers.(8)
Our patient, soon after starting systemic steroids, became afebrile and leucocytosis improved, and the wound showed rapid healing. He was transitioned to oral steroids. Throughout his hospital stay, no atrial tachyarrhythmias were recorded by telemetry monitoring. He was discharged home with the plan to pursue further work-up to identify a possible underlying systemic illness accounting for the pyoderma gangrenosum.
References
- Klug D, et al. Risk factors related to infections of implanted pacemakers and cardioverter-defibrillators. Results of a large prospective study. Circulation. 2007;116:1349-1355.
- Johansen JB, et al. Infection after pacemaker implantation: infection rates and risk factors associated with infection in a population-based cohort study of 46299 consecutive patients. Eur Heart J. 2011;32:991-8.
- de Oliveira, JC, et al. Efficacy of antibiotic prophylaxis before the implantation of pacemakers and cardioverter-defibrillators: Results of a large, prospective, randomized, double-blinded, placebo-controlled trial. Circ Arrhythmia Electrophysiol. 2009;2:29–34.
- Muhammad RS, et al. Risk Factor Analysis of Permanent Pacemaker Infection. Clin Infect Dis. 2007;45:166-173.
- Kaur MR, et al. Recurrent postoperative pyoderma gangrenosum complicating pacemaker insertion. Eur Acad Dermatol Venereol. 2006;20:66–467.
- Lo TS, et al. Pyoderma gangrenosum presented as a refractory wound infection following permanent pacemaker implantation. Heart. 2002;87:414.
- Selvapatt N, et al. Pyoderma gangrenosum complicating an implantable cardioverter defibrillator wound in a patient with ulcerative colitis. Europace. 2009;11:1482.
- Miller, J., et al. Pyoderma gangrenosum: a review and update on new therapies. J Am Acad Dermatol. 2010;62:646.

