Recurrent SVT in a Patient With Systemic Amyloidosis
|
|
What would be the next most appropriate course of action?
Show Answer

|
|
Show Answer
The correct answer is: D. Electrophysiologic study and possible ablation
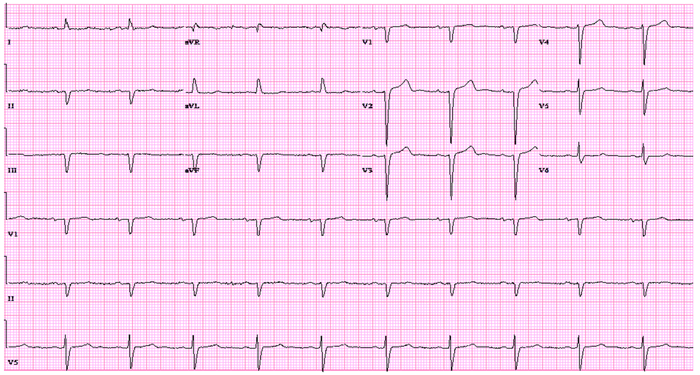
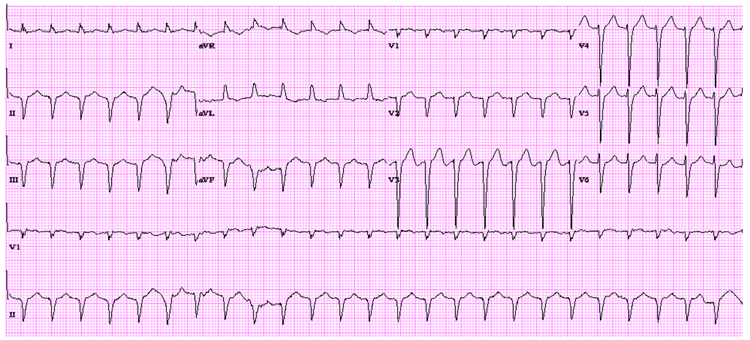
We describe a patient with an infiltrative cardiomyopathy, presumed to be cardiac amyloid given his prior history of TTR amyloidosis, who presented with multiple episodes of AV Nodal Re-entrant Tachycardia (AVNRT). The tracing above shows a regular narrow complex tachycardia with pseudo R' in lead V1 consistent with a short RP tachycardia. AVNRT is typically associated with structurally normal hearts and usually has a good prognosis.1
Cardiac amyloid is an infiltrative cardiomyopathy which occurs from protein deposition that can cause heart failure, arrhythmias, and early death. In at least half of cases presenting with familial amyloid (TTR subtype) mortality typically is cardiac in nature.3 Contingent upon where the amyloid is deposited, familial amyloid can lead to a restrictive cardiomyopathy. Many studies have shown a high prevalence of atrial and ventricular rhythm disturbances which worsen with disease progression. Conduction abnormalities typically include low voltage on EKG, sinus node dysfunction (sick sinus syndrome), bradycardia, atrial fibrillation, advanced AV block, intraventricular block, and ventricular arrhythmias.2,4 Therapy is geared towards reducing the mortality associated with these arrhythmias by implanting pacemakers.5 However, there is no data on AVNRT in patients with cardiac amyloidosis and likely the AVNRT in the case above was co-incidental.
Cardiac MRI is becoming more customary in understanding and assessing cardiac anatomy. It provides clinically relevant prognostic data for certain dilated and infiltrative cardiomyopathies which makes it an excellent non-invasive test. Our patient's MRI had features consistent with an infiltrative cardiomyopathy; however, in limited prior studies, the LGE in cardiac amyloid is described as more diffuse than what was seen in our patient. Given our patient's history, it was likely his infiltrative cardiomyopathy was cardiac amyloidosis. If a more definitive diagnosis were needed, myocardial biopsy could be pursued and is extremely sensitive for cardiac amyloidosis.6
Despite correcting his electrolytes and volume status, the patient continued to have recurrent episodes of SVT which on EKG demonstrated a short R-P tachycardia suggesting AVNRT, an ectopic atrial tachycardia, or AV re-entrant tachycardia (AVRT). These arrhythmias are amenable to ablation with a high likelihood of a cure with a low risk of complications.7 The patient underwent an EP study that demonstrated typical AVNRT and subsequently had a successful ablation (option D).
AVNRT is one of the most common types of supraventricular tachycardia.1,7 It is usually caused by at least two functional pathways in the AV node, at least one of which is a fast pathway and one of which is a slow pathway. Typical (common) AVNRT, also known as "slow-fast", conducts anterograde through the slow pathway and retrograde through the fast pathway creating a reentry circuit. Typical AVNRT accounts for the vast majority (80-90%) of cases.7 Patient can often experience presyncope or syncope given the extreme heart rates which may be exaggerated in cardiac amyloid patients who often have restrictive physiology and thus poor left ventricular filling in the setting of tachycardia.11 Furthermore, if AVNRT is frequent or persistent as it was in our patient, tachycardia mediated cardiomyopathy can occur. Given this concern, the decision to have invasive electrophysiology study with subsequent ablation was made. Radiofrequency ablation (RFA) and cryoablation have excellent and comparable initial success rate (97-98%). Cryoablation does tend to have a higher rate of recurrence.10 The advantage of cryoablation is that the risk for causing complete heart block is close to zero whereas the incidence of complete heart block necessitating permanent pacemaker in patients undergoing RFAis 1.5-2.0%.
Option A, calcium channel blockers, are a possible therapy to suppress AVNRT. The patient, however, had chronic diarrhea and presented to the emergency room with volume depletion and hypotension. Diltiazem was decided against as it may worsen his hypotension should he become volume depleted again.
Amiodarone (option B), a class III anti-arrhythmic prolongs the effective refractory period in the anterograde fast pathway and can be successful in preventing the recurrence of AVNRT.8 Amiodorone, however, can have significant toxicities including liver effect and would not be ideal in a liver transplant patient.9
Option E, further holter monitoring, would be unlikely to add new information to what was seen on telemetry as he had multiple documented episodes of SVT already.
References
© 2026 American College of Cardiology Foundation. All rights reserved.