A 74-year-old female patient with newly diagnosed paroxysmal atrial fibrillation (AF) was managed by her general practitioner.
Known history of peripheral artery disease.
No hypertension, diabetes, heart failure, angina or prior myocardial infarction.
Normal echocardiogram.
General practitioner classed the patient as 'low risk' and started patient on aspirin only.
Three months later the patient had a left sided stroke. Oral anticoagulation was started with adjusted dose warfarin (target INR 2-3). She made a good recovery post-stroke.
Six months later she was admitted with chest pain and dynamic ECG changes in the anterolateral leads, with positive troponin. A non-ST elevation myocardial infarction was diagnosed. Coronary angiography was undertaken, and a drug eluting stent deployed in the mid segment of the left anterior descending artery.
The correct answer is: B. Triple therapy (warfarin, aspirin plus clopidogrel) for 3-6 months, then warfarin plus single antiplatelet (e.g. clopidogrel), then after 1 year, warfarin alone
At initial presentation, this 74-year-old female patient with newly diagnosed paroxysmal atrial fibrillation (AF) had a CHADS2 score=0. However, such a patient may not be at low risk, as patients with a CHADS2 score=0 have a stroke risk ranging between 0.8%/year to 3.2%/year.1 Similar observations that a CHADS2 score=0-1 is not 'low risk' have been reported in a trial cohort2 and in a series post-ablation.3
The pros and cons of the CHADS
2 score have been discussed
4. Notably, it does not include many common stroke risk factors associated with AF.
5 One systematic review using pooled c statistic and calibration analysis revealed minimal utility of both the classic and revised view of the CHADS
2 score in predicting ischaemic stroke across all risk strata.
6 The CHA
2DS
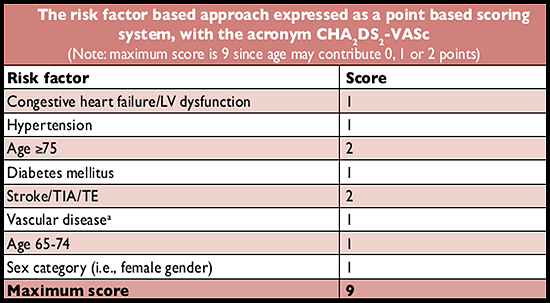
2-VASc score provides additional weight to age ≥75 (since the risk of stroke rises from age 65 upwards), vascular disease and female gender
7 [Table]. The CHA
2DS
2-VASc score is now well validated, in several independent cohorts.
The focus on identification of high risk patients was justified when warfarin was the only available oral anticoagulant, however the availability of novel oral anticoagulants with improved efficacy, safety and convenience compared to warfarin, has shifted the priority (as advocated by the clinical practice change recommended in the 2012 ESC guidelines)
8, 9 to identify 'truly low risk' patients with AF, who do not need any antithrombotic therapy. Aspirin is minimally effective and is not safer than warfarin, with similar rates of major bleeding.
10, 11
'Truly low risk' patients with a CHA
2DS
2-VASc score = 0 have an annual stroke risk < 1.0%
12 and antithrombotic therapy is not warranted. For all other AF patients either well-controlled warfarin or a novel oral anticoagulant should be offered. The CHA
2DS
2-VASc score is now the recommended stroke risk stratification score in the 2012 ESC guidelines.
8 The patient in our case history had a CHA
2DS
2-VASc score=3 prior to suffering a stroke, which was indicative of a 3.2% annual stroke risk and oral anticoagulation should have been recommended.
8
Our patient also developed an acute coronary syndrome treated with a drug-eluting coronary artery stent, which represents a difficult management problem, given the need to balance stroke and ischemia prevention against the potential for major bleeding. Consensus recommendations from Europe and North America recommend a period of triple therapy, followed by oral anticoagulant plus single antiplatelet drug for one year, followed by oral anticoagulation alone.
13-15 The recommended duration of triple therapy can range from 1 month for a bare metal stent used in an elective angioplasty/stent procedure to 6 months or more after an acute coronary syndrome necessitating a drug-eluting stent, assuming bleeding risk is acceptable.
7 Beyond one year, patients with stable vascular disease can be managed with oral anticoagulation alone, as continuing combination anticoagulant and antiplatelet therapy would result in a significant increase in major bleeding and intracranial bleeding, with no appreciable impact on stroke, death, cardiac events etc.
16
References
- Olesen JB, Torp-Pedersen C, Hansen ML, Lip GY. The value of the cha2ds2-vasc score for refining stroke risk stratification in patients with atrial fibrillation with a chads2 score 0-1: A nationwide cohort study. Thromb Haemost 2012;107:1172-1179
- Coppens M, Eikelboom JW, Hart RG, Yusuf S, Lip GY, Dorian P, Shestakovska O, Connolly SJ. The cha2ds2-vasc score identifies those patients with atrial fibrillation and a chads2 score of 1 who are unlikely to benefit from oral anticoagulant therapy. Eur Heart J 2012
- Chao TF, Lin YJ, Tsao HM, Tsai CF, Lin WS, Chang SL, Lo LW, Hu YF, Tuan TC, Suenari K, Li CH, Hartono B, Chang HY, Ambrose K, Wu TJ, Chen SA. Chads(2) and cha(2)ds(2)-vasc scores in the prediction of clinical outcomes in patients with atrial fibrillation after catheter ablation. J Am Coll Cardiol 2011;58:2380-2385
- Karthikeyan G, Eikelboom JW. The chads2 score for stroke risk stratification in atrial fibrillation--friend or foe? Thromb Haemost. 2010;104:45-48
- Pisters R, Lane DA, Marin F, Camm AJ, Lip GY. Stroke and thromboembolism in atrial fibrillation. Circ J. 2012;76:2289-2304
- Keogh C, Wallace E, Dillon C, Dimitrov BD, Fahey T. Validation of the chads2 clinical prediction rule to predict ischaemic stroke. A systematic review and meta-analysis. Thromb Haemost. 2011;106:528-538
- Pisters R, Lane DA, Nieuwlaat R, de Vos CB, Crijns HJ, Lip GY. A novel user-friendly score (has-bled) to assess 1-year risk of major bleeding in patients with atrial fibrillation: The euro heart survey. Chest. 2010;138:1093-1100
- Camm AJ, Lip GY, De Caterina R, et al. 2012 focused update of the esc guidelines for the management of atrial fibrillation: An update of the 2010 esc guidelines for the management of atrial fibrillation * developed with the special contribution of the european heart rhythm association. Europace. 2012
- Potpara TS, Lip GY, Apostolakis S. New anticoagulant treatments to protect against stroke in atrial fibrillation. Heart. 2012;98:1341-1347
- Lip GY. The role of aspirin for stroke prevention in atrial fibrillation. Nat Rev Cardiol. 2011;8:602-606
- Friberg L, Rosenqvist M, Lip GY. Evaluation of risk stratification schemes for ischaemic stroke and bleeding in 182 678 patients with atrial fibrillation: The swedish atrial fibrillation cohort study. Eur Heart J. 2012;33:1500-1510.
- Olesen JB, Lip GY, Hansen ML, et al. Validation of risk stratification schemes for predicting stroke and thromboembolism in patients with atrial fibrillation: Nationwide cohort study. BMJ. 2011;342:d124
- Lip GY, Huber K, Andreotti F, et al. Management of antithrombotic therapy in atrial fibrillation patients presenting with acute coronary syndrome and/or undergoing percutaneous coronary intervention/ stenting. Thromb Haemost. 2010;103:13-28
- Faxon DP, Eikelboom JW, Berger PB, et al. Consensus document: Antithrombotic therapy in patients with atrial fibrillation undergoing coronary stenting. A north-american perspective. Thromb Haemost. 2011;106:572-584
- Huber K, Airaksinen KJ, Cuisset T, Marin F, Rubboli A, Lip GY. Antithrombotic therapy in patients with atrial fibrillation undergoing coronary stenting: Similarities and dissimilarities between north america and europe. Thromb Haemost. 2011;106:569-571
- Lip GY. Don't add aspirin for associated stable vascular disease in a patient with atrial fibrillation receiving anticoagulation. BMJ. 2008;336:614-615