Unusual Flow in the Interventricular Septum After Septal Myectomy
A 40-year-old gentleman with past medical history notable for recently diagnosed hypertrophic obstructive cardiomyopathy (HOCM) is referred for surgical evaluation. He has a 2-year history of shortness of breath and presyncope. He has a positive family history of sudden cardiac death and premature coronary artery disease. Prior to presenting, he underwent implantable cardioverter defibrillator (ICD) placement.
The patient is hemodynamically stable. Physical examination reveals a laterally displaced double apical impulse, normal S1, paradoxically split S2, and a crescendo-decrescendo systolic ejection murmur that is best heard between the apex and left sternal border with no radiation to the carotids.
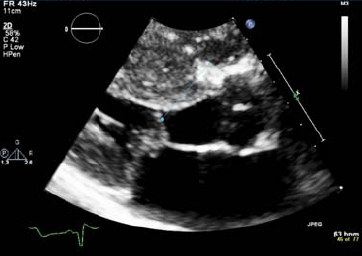
Preoperative echocardiogram shows severe left ventricular septal hypertrophy, significant dynamic left ventricular outflow tract (LVOT) gradient, systolic anterior motion of the leaflet, mild mitral regurgitation, and hyperdynamic LV function.
Figure 1: Massive Septal Hypertrophy and Systolic Anterior Motion of the Mitral Valve
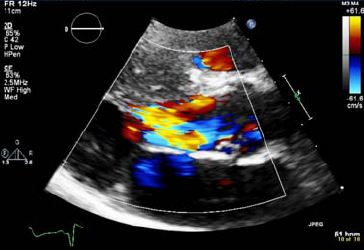
Figure 2: Systolic Flow Around the ALMV as it Contacts the Septum
His preoperative catheterization procedure does not reveal any significant coronary artery disease (CAD). An aberrant right coronary artery (RCA) was noted to be arising above the left coronary artery (LCA). A resting gradient of 100 mm Hg across the left ventricular outflow tract to the aorta. A cardiac CT scan confirmed a high origin of the RCA arising 1.3 cm cranial to the sinotubular junction with a the proximal most 0.8 segment coursing between the aorta and the pulmonary artery before entering the right atrioventricular groove.
In the preoperative phase, the patient goes into multiple episodes of ventricular tachycardia treated with ICD shocks. He subsequently undergoes successful septal myectomy, unroofing of the left anterior descending artery (LAD) and coronary artery bypass graft to the LAD utilizing the left internal mammary artery (LIMA).
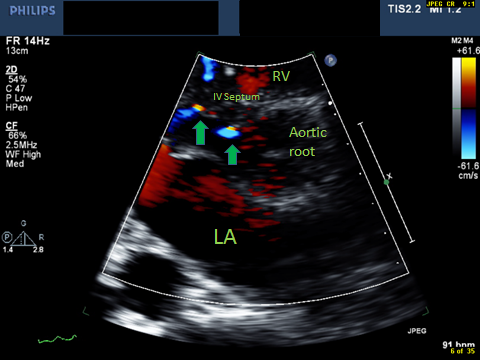
Postoperative echocardiogram reveals a decrease in the thickness of the interventricular septum with no evidence of systolic anterior motion of the mitral valve or an LVOT gradient. Color Doppler examination reveals the presence of diastolic flow originating from the left ventricular side of the septum and directed towards the LVOT (Figure 3, Video 1). This jet was not present on the preoperative echocardiogram.
Figure 3
Video 1
Diastolic flow noted on the postoperative echocardiogram can be best explained by the presence of which of the following?
Show Answer