Evolution of Critical Care Cardiology: Meeting the Critical Care Crisis Head-On
On September 11th, 2012, the American Heart Association (AHA) published a scientific statement1 on the evolution of Critical Care Cardiology and the need for new medical staffing and training models for the contemporary cardiac intensive care unit (CICU). It does not take any more than standing in most CICUs in the United States and looking around you to immediately recognize that things have changed over the past decade.2 No longer do you see mostly uncomplicated patients post-myocardial infarction. Rather, you see older patients, with more non-cardiovascular comorbid conditions, higher severity of illness, and more devices for monitoring or therapy. This changing landscape necessitates thoughtful consideration of the current organization of care in CICUs to guide how the cardiovascular community ought to respond to the 'critical care crisis' before other stakeholders impose their own requirements.
Lessons Learned from General Medical and Surgical Critical Care
The cardiovascular community in the United States has been somewhat slow to react to this shifting landscape compared with our colleagues in general critical care medicine and in CICUs in Europe.3 Clinical studies, predominantly observational and performed almost entirely in general ICUs, have provided strong evidence that the best outcomes in patients with critical illness are achieved when care is provided by dedicated intensivists leading experienced multidisciplinary teams.4,5 Such evidence has promoted a shift toward 'closed units,' in which care is transferred to a supervising intensivist upon admission of patients to the ICU, or 'high intensity' staffing, defined by either a closed unit environment or mandatory consultation of an intensivist. Such data have also captured the attention of external business entities, consumer focus groups, and public agencies6 and are consistent with the findings of most studies of cardiovascular procedural volume; more experience is associated with better outcomes and it's not just the provider, it's the team.
Roadmap for Critical Care Cardiology
Recognizing the changing face of critical care, the AHA assembled a multidisciplinary Writing Group to formulate a 'roadmap' for the future of critical care cardiology in the United States. The AHA statement emphasizes 3 central tenets:
- The delivery of cardiac critical care has advanced considerably in terms of its complexity (patients, therapies, and ICU environment all included).
- The advanced expertise of the cardiovascular specialist is pivotal to providing the best possible care for patients with acute cardiovascular diseases. If the main reason that the patient is 'sick' is cardiac, then a cardiologist should be driving their care.
- Access to clinicians who have specialized skills in critical care is important for all settings in which cardiovascular critical care is provided.
The Writing Group proposed 2 primary models for delivering care that is consistent with these tenets:
- Cardiac intensivist model: In this model, which the Writing Group favored for the advanced CICU, care is led by cardiologists with specialized expertise in critical care (acquired either through focused experience or advanced training).
- Shared responsibility model: In this model, which is the most adaptable to a variety of clinical settings, cardiologists and general intensivists co-manage patients in the CICU.
Proposal for Categorization of CICUs
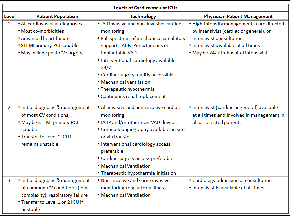
The Writing Group recognized that many CICUs in the United States provide care for a broad spectrum of patients, including patients with uncomplicated myocardial infarction, with heart failure without shock, or with focused cardiovascular problems such as unstable arrhythmias. However, other CICUs may care almost solely for patients with more complex multisystem involvement, including patients with shock, multisystem organ failure, anoxic brain injury due to cardiac arrest, massive pulmonary embolism, intractable unstable arrhythmias, and other advanced disease such as severe pulmonary hypertension. It is for such patients that the best available evidence indicates that more favorable outcomes are observed when cared for in an experienced critical care unit by multidisciplinary teams led by physicians with specialized skills in critical care.4,5 However, it is neither necessary nor possible for all hospitals in the United States to be equipped to provide comprehensive care to such patients.Therefore, the AHA statement describes a schema for categorizing the level of care offered by the CICU within an individual healthcare system. Using a nomenclature similar to the familiar trauma center classification system established by the American College of Surgeons, the AHA statement describes 3 different categories of ICU: Level 1 (most advanced), Level 2, and Level 3 (Table 1). For the Level 1 CICU, the Writing Group favors care by a cardiac intensivist, cohesively providing both specialized cardiovascular and critical care expertise. In the Level 3 CICU, most patients will be cared for by cardiologists with intensivists available for consultation when a patient's condition requires critical care (e.g. new respiratory failure requiring mechanical ventilation). Level 2 CICU's fall in between these 2 categories and may use a high-intensity staffing model, or alternatively intensivist staffing for selected patients.
Implications for Cardiovascular Training
The Writing Group concluded that in the face of the progressively increasing complexity of the CICU environment there is a rationale for developing new training pathways for selected cardiovascular trainees who wish to acquire advanced skills in critical care. It is expected that under current training paradigms, cardiovascular trainees will acquire the basic knowledge and skills required to be competent as a cardiovascular consultant for patients who are critically ill (COCATS level 1 or 2).7 However, given the competing demands of cardiovascular training, it is challenging for cardiovascular trainees to gain sufficient experience in the CICU environment to master the full set of advanced critical care skills that are optimal for a Level 1 CICU. Thus, the AHA statement describes strong grounds for providing opportunities for advanced training in this specialized area (COCATS level 3) for individuals who desire to practice as a dedicated cardiac intensivist. At the same time, the Writing Group advocated for attention to continuing medical education and reassessment of proficiency focused for providers of cardiac critical care.
Summary
The contemporary advanced CICU has evolved from a "coronary" observation unit to a complex ICU environment that provides comprehensive critical care for patients with acute or chronic cardiovascular disease. This transformation of the CICU arrives at both an opportunity and a necessity to develop innovative approaches to staffing, structure, and training. The AHA scientific statement on Critical Care Cardiology provides a blueprint for the continued maturation of the CICU with evidence-based staffing models that include the availability of experienced cardiac intensivists or consulting general intensivists for patients requiring advanced cardiac critical care. Such specialized skills may have been acquired through experience or formal advanced training. The AHA statement describes a classification system based on the capabilities and resources of the individual CICU or health system, with the 2 highest levels (Level 1 and level 2) requiring the availability of intensivists (cardiac or general) and specialized multidisciplinary teams. The statement also describes proposed novel pathways for training of cardiologists with advanced skills in critical care cardiology.
The AHA statement is a starting point for additional important discussion within our cardiovascular professional societies, as well as with other major stakeholders in the training and certification of cardiovascular specialists. In addition, the statement identifies an unmet need for additional investigation of specific organizational and practice interventions within CICUs.
References
- Morrow DA, Fang JC, Fintel DJ, et al. Evolution of Critical Care Cardiology: Transformation of the Cardiovascular Intensive Care Unit and the Emerging Need for New Medical Staffing and Training Models: A Scientific Statement From the American Heart Association. Circulation 2012.
- Katz JN, Shah BR, Volz EM, et al. Evolution of the coronary care unit: clinical characteristics and temporal trends in healthcare delivery and outcomes. Crit Care Med 2010;38:375-81.
- Hasin Y, Danchin N, Filippatos GS, et al. Recommendations for the structure, organization, and operation of intensive cardiac care units. Eur Heart J 2005;26:1676-82.
- Pronovost PJ, Angus DC, Dorman T, Robinson KA, Dremsizov TT, Young TL. Physician staffing patterns and clinical outcomes in critically ill patients: a systematic review. JAMA 2002;288:2151-62.
- Pronovost P, Thompson DA, Holzmueller CG, Dorman T, Morlock LL. Impact of the Leapfrog Group's intensive care unit physician staffing standard. J Crit Care 2007;22:89-96.
- Angus DC, Shorr AF, White A, Dremsizov TT, Schmitz RJ, Kelley MA. Critical care delivery in the United States: distribution of services and compliance with Leapfrog recommendations. Crit Care Med 2006;34:1016-24.
- Beller GA, Bonow RO, Fuster V. ACCF 2008 Recommendations for Training in Adult Cardiovascular Medicine Core Cardiology Training (COCATS 3) (revision of the 2002 COCATS Training Statement). J Am Coll Cardiol 2008;51:335-8.
Keywords: American Heart Association, Critical Care, Intensive Care Units, Myocardial Infarction
< Back to Listings