Warfarin Pharmacogenetics: The COAG Trial
The use of genetic testing to guide therapy for patients initiating warfarin has had both support and opposition from clinicians, regulatory agencies and societies, and payers. Much of the debate has centered on the lack of large-scale randomized trials. While observational studies1,2 and some small randomized trials have suggested benefit to genotyping patients,3,4 other small trials have not.5,6
The Clarification of Optimal Anticoagulation through Genetics (COAG) trial was a large, multicenter, double-blind, randomized controlled trial designed specifically to determine if the use of genetics for initial warfarin dosing provides additional benefit on anticoagulation control, above and beyond what can be gleaned for clinical information alone.7 The hypothesis was that the addition of genetics to clinical information for dose selection (the pharmacogenetic algorithm arm, PGx) over the initial five days of therapy would lead to better anticoagulation control compared with dosing based solely on clinical information (the clinical algorithm arm). There were several key design elements in COAG that were chosen to try to ensure that a valid answer could be reached for the study's hypothesis. First, the study's comparison group used a clinical dosing algorithm rather than empiric dosing. This ensured that any differences between the two groups would be attributable to the effects of genetics. If empiric dosing (e.g., 5 mg starting dose for most patients) was used, then any differences between the PGx algorithm (which used both genetic and clinical information) and empiric dosing could be attributable to the formalized use of clinical information, genetics, or both. Second, the study was powered to examine the effects of genetics in both all-comers and among those most likely to benefit from genotyping (defined as those with a predicted dose difference between the clinical and PGx algorithms of at least 1 mg/day). Third, warfarin dosing was blinded during the primary (one month) follow-up period. If dosing was known to clinicians and patients, it would be likely that they could identify, at least some of the time, which arm they were in and whether the patient had genetic variants (e.g., those with low or high doses that would be unlikely to be given in the clinical arm). This could alter the approach to monitoring, reporting of outcomes, adherence to medication and diet, etc. Of course, all participants, clinicians, and investigators were also blinded to genotype. Fourth, the study enrolled a large number of African Americans (27% of the study cohort) because it was known that PGx algorithms may not predict as well in African Americans compared with other groups, and the effects in this important group of patients had not been studied in prior trials. Subgroup analysis by race was prespecified in the protocol.
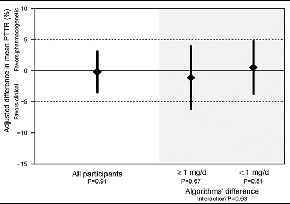
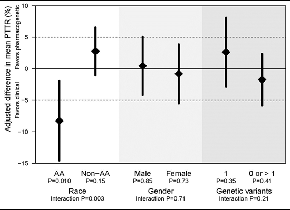
The primary outcome was the percentage of time in therapeutic INR range (PTTR) in the first four weeks of therapy. Overall, there was no difference between the PGx arm and the clinical arm, both overall and in the co-primary analysis among those with predicted dose differences between the two arms of at least 1 mg/day (see Figure 1). The mean PTTR at four weeks was 45.2% in the PGx arm and 45.4% in the clinical arm. However, there was a statistically significant difference in the dosing strategies by race: Among African Americans, the mean PTTR was significantly lower in the PGx arm (35.2%) than in the clinical algorithm arm (43.5%), while there was no statistically significant differences among non-African Americans. (see Figure 2). In addition, African Americans in the PGx arm took longer to reach a first therapeutic INR and were more likely to have elevated INRs than those in the clinical algorithm arm.
The study concluded that there was no benefit to adding genetics to a clinical dosing algorithm and that, among African Americans, the clinical strategy did better than the PGx strategy. This study highlights the importance of performing randomized trials of pharmacogenetic strategies, particularly for complex medications such as warfarin.
Of note, in the same issue of the New England Journal of Medicine, two other pharmacogenetic studies were reported among patients taking warfarin or coumarin derivatives (both part of the EU-PACT trial). In the former, performed in the UK, the comparison was between a PGx strategy that included clinical and genetic information and a fixed-dose strategy that did not incorporate clinical factors (except for age).8 The study also was not double-blinded, was about half the size of the COAG trial, and enrolled very few African Americans. The trial did demonstrate better AC control in the PGx arm versus the fixed dose arm at the primary endpoint at 3 months. The other EU-PACT trial, performed in the Netherlands and Greece, compared a PGx algorithm with a clinical algorithm for patients initiating phenprocoumon or acenocoumarol.9 There was no benefit to the PGx strategy for the primary endpoint (3 month PTTR). There was however benefit in the post-hoc analyses of PTTR at one month.
References
- Epstein RS, Moyer TP, Aubert RE et al. Warfarin genotyping reduces hospitalization rates results from the MM-WES (Medco-Mayo Warfarin Effectiveness study). J Am Coll Cardiol 2010;55:2804-12.
- Anderson JL, Horne BD, Stevens SM et al. A randomized and clinical effectiveness trial comparing two pharmacogenetic algorithms and standard care for individualizing warfarin dosing (CoumaGen-II). Circulation 2012;125:1997-2005.
- Wang M, Lang X, Cui S et al. Clinical application of pharmacogenetic-based warfarin-dosing algorithm in patients of Han nationality after rheumatic valve replacement: a randomized and controlled trial. Int J Med Sci 2012;9:472-9.
- Caraco Y, Blotnick S, Muszkat M. CYP2C9 Genotype-guided Warfarin Prescribing Enhances the Efficacy and Safety of Anticoagulation: A Prospective Randomized Controlled Study. Clin Pharmacol Ther 2008;83:460-70.
- Anderson JL, Horne BD, Stevens SM et al. Randomized Trial of Genotype-Guided Versus Standard Warfarin Dosing in Patients Initiating Oral Anticoagulation. Circulation 2007;116:2563-70.
- Burmester JK, Berg RL, Yale SH et al. A randomized controlled trial of genotype-based Coumadin initiation. Genet Med 2011;13:509-18.
- Kimmel SE, French B, Kasner SE et al. A pharmacogenetic versus a clinical algorithm for warfarin dosing. N Engl J Med 2013;369:2283-93.
- Pirmohamed M, Burnside G, Eriksson N et al. A randomized trial of genotype-guided dosing of warfarin. N Engl J Med 2013;369:2294-303.
- Verhoef TI, Ragia G, de Boer A et al. A randomized trial of genotype-guided dosing of acenocoumarol and phenprocoumon. N Engl J Med 2013;369:2304-12.
Clinical Topics: Anticoagulation Management, Arrhythmias and Clinical EP, EP Basic Science
Keywords: African Americans, Coumarins, Greece, Netherlands, Pharmacogenetics, Warfarin
< Back to Listings