Biomarkers of Chronic Cardiac Injury and Hemodynamic Stress Identify a Malignant Phenotype of LV Hypertrophy
Editor’s Note: This article is based on Neeland IJ, Drazner MH, Berry JD, et al. Biomarkers of chronic cardiac injury and hemodynamic stress identify a malignant phenotype of left ventricular hypertrophy in the general population. J Am Coll Cardiol 2013;61:187-95.
What is the independent contribution of elevated biomarkers to predicting risk in patients with left ventricular hypertrophy (LVH)? In this study, the authors tested the ability of markers of subclinical myocardial injury (high sensitivity cardiac troponin T [hscTnT]) and hemodynamic stress (N-terminal pro–B-type natriuretic peptide [NT-proBNP]) for identifying asymptomatic individuals with LVH who were at increased risk for heart failure (HF) and death.
A total of 2,413 participants in the Dallas Heart Study who were without clinical HF, LV dysfunction, or chronic kidney disease underwent measurement of LV mass by magnetic resonance imaging (MRI). Levels of hscTnT, and NT-proBNP were also measured. Patients were stratified according to LVH and by detectable cTnT (≥3 pg/ml) and increased NT-proBNP values. For each analysis, participants were categorized into groups based on the presence or absence of LVH and biomarker elevations.
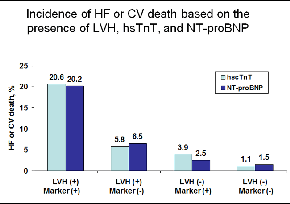
Of the participants, 9% were LVH(+), 25% were hscTnT(+), and 24% were NT-proBNP(+). Those who were LVH(+) and hscTnT(+) and/or NT-proBNP(+)(n = 144) were older and more likely to be male, with a greater risk factor burden and more severe LVH compared with those who were LVH(+) but biomarker(–) (p <0.01 for each). Within the LVH population, structural changes associated with cTnT included increased LV wall thickness and concentricity; in contrast, NT-proBNP was associated with increased LV end-diastolic and end-systolic volumes. During a median follow-up period of 8.1 years, the primary outcome of HF or CV death occurred in 65 (2.7%) participants, including 28 HF events (65% systolic HF and 35% diastolic HF) and 37 CV deaths. The cumulative incidence of HF or CV death was significantly higher among LVH(+) who had elevated hscTnT(+) (p < 0.0001)(FIGURE). Individuals who were LVH(+) and either hscTnT(+) or NT-proBNP(+) remained at >4-fold higher risk for HF or CV death after multivariable adjustment for CV risk factors, renal function, and LV mass compared with those who were LVH(–), biomarker(–). When ECG-defined LVH was used instead of MRI, individuals who were biomarker (+) identified those who had an increased risk for HF or CV death of >11% compared with those with ECG-defined LVH but who were biomarker (-).
The authors concluded that minimal elevations in biomarkers of subclinical cardiac injury and hemodynamic stress accentuate the association of LVH with adverse outcomes, identifying a malignant subphenotype of LVH with high risk for progression to HF and CV death.
Discussion
Although LVH is associated with substantial morbidity and mortality, including the development of HF and death,1,2 the natural history of LVH is heterogeneous. Identifying markers related to the pathways that contribute to the transition from LVH to clinical HF could potentially identify asymptomatic individuals at high risk for adverse outcomes. If this can be done, potentially new therapeutic targets could be identified that would prevent disease progression.
The biomarkers the authors chose to evaluate, hscTnT and NT-proBNP, are released from cardiac myocytes in response to increased LV wall stress and hypertrophy, as well as being markers of cardiac injury.3,4 In addition, both biomarkers have been shown to associate strongly with HF5,6 and mortality7,8 in the general population.
The authors found a marked variation in outcomes in patients LVH, with a very high risk of HF or CV death seen in individuals who had LVH and elevated (as defined in the study) hscTnT and NT-proBNP. Although they represented only a minority of the total population, those with elevated biomarkers accounted for almost 40% of HF or CV death events. An interesting finding was that the results were not explained simply by higher LV mass among those with abnormal cTnT or NT-proBNP; findings remained consistent after further adjustment using the most accurate measure of LV mass- cardiac MRI. Therefore, increases in hscTnT and NT-proBNP, rather than simply being a marker for more severe LVH, identify a cohort in whom there is likely adverse remodeling, leading to clinical HF and CV death.
Currently, cMRI is considered to gold standard for measuring left ventricular mass, although expensive. Although cheaper, screening using echocardiography is also cost-prohibitive. An alternative suggested by the authors is to combine the ECG (despite its systematic underestimation of the true prevalence of LVH), with biomarkers, as the interaction between LVH and hscTnT and NT-proBNP was maintained.
Strengths of the current study include use of both cardiac MRI imaging and standard ECG criteria to define LVH, the assessment of cardiac injury by using hscTnT, and long term follow-up in a prospective cohort. The inclusion of a large proportion of African-American patients, a population not routinely included in most studies, is also an important contribution.
Several limitations merit comment. As the authors noted, the number of HF and CV death events was relatively small and therefore the results should be considered preliminary, although they do offer important hypotheses that should be tested. Because of the higher frequency of detectable hscTnT in older patients, different thresholds for each marker may be necessary. In addition, the values considered abnormal for this study may be within the normal range for most individuals, which may limit their use as a screening tool. The authors noted that there is some evidence to suggest the effects of elevated biomarkers may be modified. However, given the relatively small numbers of patients who were LVH (+) who had elevated hsTnT and NT-proBNP, and the prolonged duration of follow up required to detect differences, may make this difficult to do.
In conclusion, by using simple biomarker screening, the authors have identified a subgroup of patients with LVH who are at every high risk for cardiac events. This offers the potential for early detection of a patient population in whom aggressive prevention and treatment may be warranted, with the goal of improving outcomes.
References
- M.H. Drazner, J.E. Rame, E.K. Marino et al. Increased left ventricular mass is a risk factor for the development of a depressed left ventricular ejection fraction within five years: the Cardiovascular Health Study. J Am Coll Cardiol 2004;43:2207–221.
- D. Levy, R.J. Garrison, D.D. Savage, W.B. Kannel, W.P. Castelli. Prognostic implications of echocardiographically determined left ventricular mass in the Framingham Heart Study. N Engl J Med 1990;322:1561–1566.
- T.W. Wallace, S.M. Abdullah, M.H. Drazner et al. Prevalence and determinants of troponin T elevation in the general population. Circulation 2006;113:1958–1965.
- J.A. de Lemos, D.K. McGuire, M.H. Drazner. B-type natriuretic peptide in cardiovascular disease. Lancet 2003;362:316–322.
- J.G. Smith, C. Newton-Cheh, P. Almgren et al. Assessment of conventional cardiovascular risk factors and multiple biomarkers for the prediction of incident heart failure and atrial fibrillation. J Am Coll Cardiol 2010;56:1712–1719.
- J.T. Saunders, V. Nambi, J.A. de Lemos et al. Cardiac troponin T measured by a highly sensitive assay predicts coronary heart disease, heart failure, and mortality in the Atherosclerosis Risk in Communities Study. Circulation 2011;123:1367–1376.
- C. Kistorp, I. Raymond, F. Pedersen, F. Gustafsson, J. Faber, P. Hildebrandt. N-terminal pro-brain natriuretic peptide, C-reactive protein, and urinary albumin levels as predictors of mortality and cardiovascular events in older adults. JAMA, 2005;293:1609–1616.
- J.A. de Lemos, M.H. Drazner, T. Omland et al. Association of troponin T detected with a highly sensitive assay and cardiac structure and mortality risk in the general population. JAMA 2010;304:2503–2512.
Clinical Topics: Heart Failure and Cardiomyopathies, Noninvasive Imaging, Acute Heart Failure, Chronic Heart Failure, Heart Failure and Cardiac Biomarkers, Magnetic Resonance Imaging
Keywords: Biomarkers, Follow-Up Studies, Heart Failure, Heart Failure, Diastolic, Hemodynamics, Hypertrophy, Left Ventricular, Magnetic Resonance Imaging, Natriuretic Peptide, Brain, Phenotype, Risk Factors, Troponin T
< Back to Listings