PFO in a SCUBA Diver: When Is It Safe to Continue Diving?
A 22-year-old healthy, asymptomatic female is referred to the adult congenital cardiology clinic after she is found to have a positive bubble study on echocardiogram. The patient is an avid recreational diver and plans to attend the Divers Institute of Technology (DIT) to be trained in commercial diving. The echocardiogram was ordered prior to enrollment due to a history of migraines. She takes an oral contraceptive but no additional medications. She has no personal or family history of transient ischemic attacks (TIA), stroke, syncope or blood clots. She has not had any episodes of decompression illness and strictly adheres to the Navy diving tables. On exam, her vital signs are stable, and no murmur is appreciated. The rest of her exam is benign. Electrocardiogram is unremarkable. A transesophageal echocardiogram (Figure 1) was performed with images below.
Figure 1
Figure 1
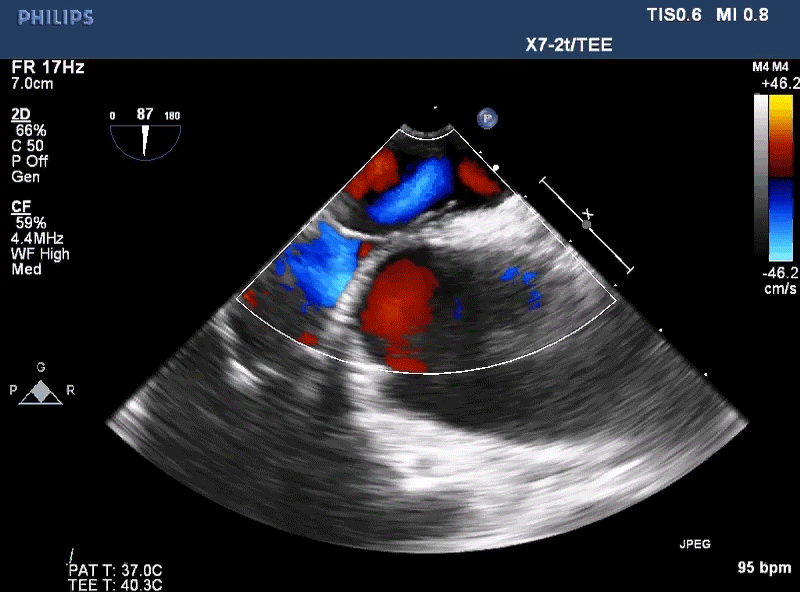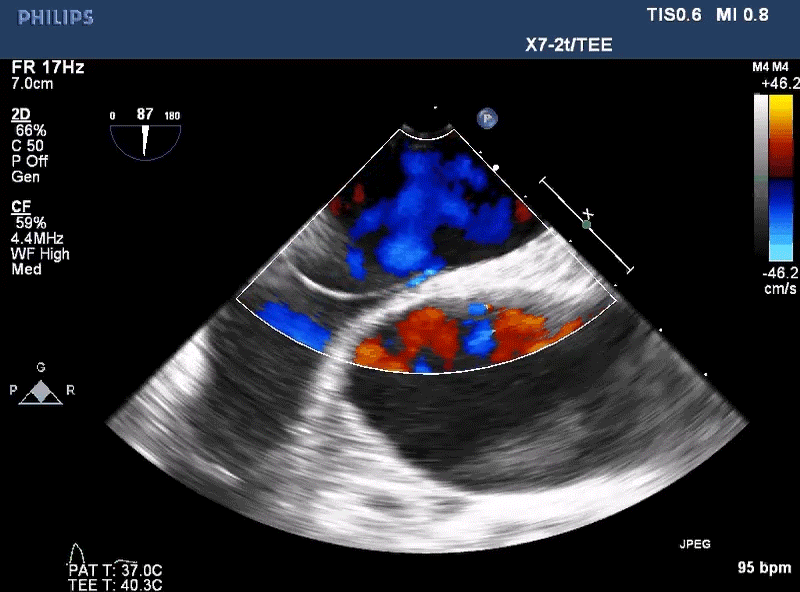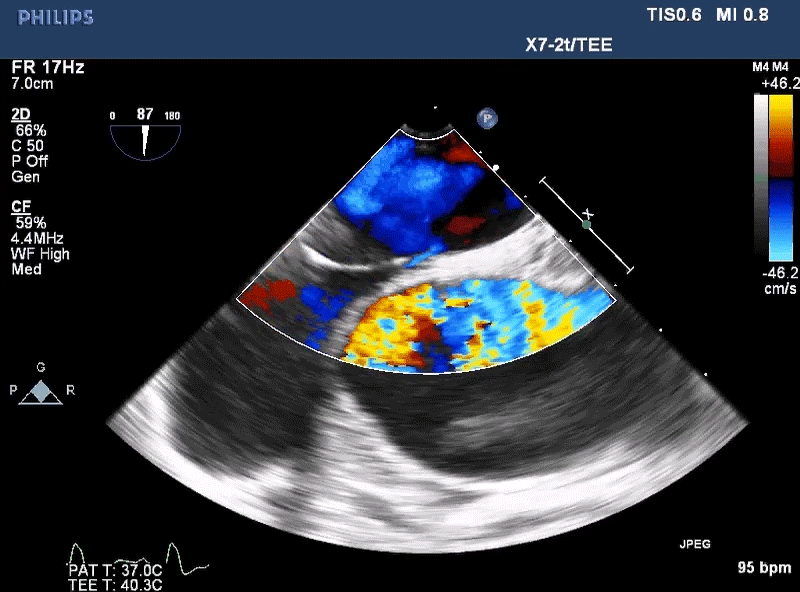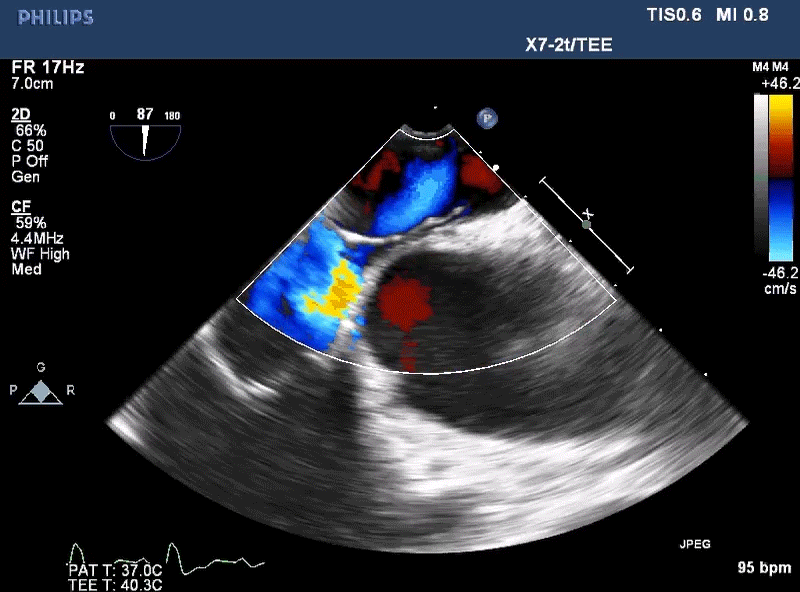
Given the information provided and the image seen, what do you recommend for this patient?
Show Answer
The correct answer is: E. Utilize a shared decision-making approach to discuss our current understanding of the risks and benefits of PFO closure and with continued diving with no intervention.
This case describes an incidentally found patient foramen ovale (PFO) in a young woman who is preparing for a professional diving career. The patient was referred given concern for the development of arterial gas embolism (AGE), a form of decompression illness (DCI) in the setting of her having a PFO. Venous gas bubbles in small quantities are common after recreational dives and are filtered by the lungs so divers generally remain asymptomatic. DCI is a term used to describe illness caused by formation or expansion of existing inert gas bubbles (usually nitrogen) in blood or tissue after a reduction in environmental pressure (decompression).1 DCI encompasses two conditions: decompression sickness (DCS), which causes local damage, and AGE, which results from bubbles entering the arterial circulation after pulmonary barotrauma or in the setting of a right-to-left shunt.
Rapid ascents, pulmonary pathology, and breath holding increase the risk of developing DCI. The likelihood of bubbles crossing an intracardiac right-to-left shunt is increased during times of physical stress, such as bearing down while hauling heavy equipment out of the water following a dive. The type of DCI typically associated with right-to-left shunts is cerebral and spinal in nature.2 Several studies have shown that compared to control subjects, divers who report symptoms of DCI are more likely to demonstrate a right-to-left shunt.3 The relative risk of DCI in divers with a PFO is reported to be five times higher than divers without a PFO and seems to be proportional to the size of the PFO.4 However, DCI events are quite rare with a reported incidence between 1/1200 and 1/20000 dives and only 1/3 of DCI events occur in those with a PFO.5 Thus, while the relative risk of DCI in divers with a PFO may be higher than those without a PFO, the absolute risk remains quite low.
Given the overall low absolute risk of DCI and the lack of a clear causal relationship between a PFO and subsequent DCI, current guidelines warn against screening for PFO in both recreational and commercial divers.6 Recreational divers with known right-to-left shunts should be advised to refrain from diving greater than 15m in depth. Should they desire to go deeper, they should be advised to use more conservative dive profiles, avoiding rapid ascents, or consider using enriched air "NITROX" (higher oxygen and lower nitrogen content) to minimize the accumulation of venous bubbles.7 In those who have had more than one episode of DCI and want to continue diving deeper than 15m, it may be reasonable to evaluate for a PFO. In professional divers who have suffered AGE, there should be a lower threshold for PFO screening as modifying dive tables or stopping diving may not be realistic options.8
Closing a PFO using the newly approved percutaneous devices is not without risks. Recent evidence suggests that adverse outcomes are seen in ~7% of patients with the two most common being arrhythmia (3.7%) and vascular complications (3%).9 In this study, patients less than 60 years of age and those with fewer comorbidities had lower rates of adverse events during percutaneous PFO closure. Divers are often young and healthy. While large studies evaluating the rates of adverse events in a population of divers are lacking, the rates of adverse events may be lower than reported in the higher risk population of patients with a history of stroke or TIA. There are limited data on patients with a history of DCI who were subsequently treated with PFO closure. In one study, of the seven divers who had their PFO closed, all returned to diving without another incident of DCI over the 3-12 months they were followed.10 Their diving profiles before and after the procedure were not reported. Another study compared 47 divers with known open PFOs to those with PFOs recently closed via a catheter-based approach in a simulated dive experience using a hyperbaric chamber. After decompression, an equal number of patients in each group demonstrated venous gas bubbles. Notably, arterial bubbles were not detected in those whose PFO had been closed while 30% of those with a PFO and no intervention had detectable arterial bubbles.11 A similar study following recreational divers with a history of major DCI over a 5.5-year period showed that closure of PFO appeared to prevent recurrence of both severe symptomatic DCI and asymptomatic cerebral DCI as detected by brain magnetic resonance imaging (MRI) compared to those without PFO closure.12 Longer term follow-up in this population is lacking but it is important to emphasize that PFO closure does not eliminate a diver's risk for DCI as there are mechanisms other than right-to-left shunting that can lead to AGE. There is currently no evidence regarding prophylactic closure of PFO for the prevention of DCI.13
Our patient was diving recreationally for several years and never had symptoms of decompression illness. In this case, a screening echocardiogram would not have been recommended. Nevertheless, she was discovered to have an asymptomatic PFO and will be attending commercial diver school where dive profiles may not be adjustable. She also has migraine headaches which, if associated with aura, put a patient at higher risk for neurological DCI.14 In a circumstance where evidence is lacking, and a specific recommendation is not clear, shared decision making between the patient and physician should be considered. Key points to emphasize: 1) There is strong consensus that having PFO is not a contraindication to diving, 2) A PFO may minimally increase one's risk for DCI but evidence of a causal relationship between a PFO and DCI is lacking, 3) Diving with more conservative parameters is likely a better strategy to reduce the risk of DCI than closure of a PFO, 4) Percutaneous PFO closure is not a risk-free procedure and does not eliminate the risk of DCI. Finally, should closure be pursued, a period of treatment with antiplatelet and confirmation of closure must be completed prior to returning to dive activities. Given our patient's desire to dive commercially with limited ability to modify diving tables and to potentially minimize her risk of future DCI, she elected to have her PFO closed and has done well without complications from the procedure or incident DCI.
References
- Liou K, Wolfers D, Turner R, et al. Patent foramen ovale influences the presentation of decompression illness in SCUBA Divers. Heart Lung Circ 2015;24:26-31.
- Cantais E, Louge P, Suppini A, Foster PP, Palmier B. Right-to-left shunt and risk of decompression illness with cochleovestibular and cerebral symptoms in divers: case control study in 101 consecutive dive accidents. Crit Care Med 2003;31:84-8.
- Moon RE, Bove AA. Transcatheter occlusion of patent foramen ovale: a prevention for decompression illness? Undersea Hyperb Med. 2004;31:271-4.
- Torti SR, Billinger M, Schwerzmann M, et al. Risk of decompression illness among 230 divers in relation to the presence and size of patent foramen ovale. Eur Heart J 2004;25:1014-20.
- Bove AA, Moon RE. Patent foramen ovale - is it important to divers? (Divers Alert Network website). 2004. https://www.diversalertnetwork.org/ Accessed 11/01/2019.
- Vann RD, Butler FK, Mitchell SJ, Moon RE. Decompression illness. Lancet 2011;377:153–164.
- Wilmshurst P, Walsh K, Morrison L. Transcatheter occlusion of foramen ovale with a button device after neurological decompression illness in professional divers. Lancet 1996;348:752–3.
- UHMS best practice guidelines: prevention and treatment of decompression sickness and arterial gas embolism. http://membership.uhms.org/resource/resmgr/dcsandage_prevandmgt_uhms-fi.pdf. Accessed 11/01/2019.
- Merkler AE, Gialdini G, Yaghi S, et al. Safety outcomes after percutaneous transcatheter closure of patent foramen ovale. Stroke 2017;48:3073-7.
- Walsh KP, Wilmshurst PT, Morrison WL. Transcatheter closure of patent foramen ovale using the Amplatzer septal occluder to prevent recurrence of neurological decompression illness in divers. Heart 1999;81:257-61.
- Honek J, Sramek M, Sefc L. et al. Effect of catheter-based patent foramen ovale closure on the occurrence of arterial bubbles in scuba divers. JACC Cardiovasc Interv 2014;7:403-8.
- Billinger M, Zbinden R, Mordasini R, et al. Patent foramen ovale closure in recreational divers: effect on decompression illness and ischaemic brain lesions during long-term follow-up. Heart 2011;97:1932-7.
- Sykes O, Clark JE. Patent foramen ovale and scuba diving: a practical guide for physicians on when to refer for screening. Extrem Physiol Med 2013;2:10.
- Wilmshurst P, Nightingale S. Relationship between migraine and cardiac and pulmonary right-to-left shunts. Clin Sci 2001;100:215–20.
