Valve-in-Ring Transcatheter MVR Via Antegrade Percutaneous Approach: Consideration of Sex in the Selection of Surgery vs. TVT
An 87-year-old woman presents with shortness of breath at rest that increases when in the supine position.
The patient's cardiac history is significant for aortic stenosis status post bioprosthetic aortic valve replacement 15 years prior, mitral regurgitation status post repair using a mitral annular ring 15 years prior, congestive heart failure, paroxysmal atrial fibrillation, hypertension, and hyperlipidemia.
On physical exam, the patient is in apparent respiratory distress sitting upright with temperature 36.7°C, heart rate 100 to 110 beats per minute, blood pressure 100/69 mm Hg, respiratory rate 18 breaths per minute, and peripheral oxygen saturation 96% on noninvasive positive pressure ventilation. Her exam is notable for jugular venous distention to the mandible, laterally displaced point of maximal impulse, irregularly irregular heart rhythm, diastolic murmur heard best at the apex, and crackles in the lower half of the lung fields bilaterally. Laboratory data is significant only for a normocytic anemia. Surface electrocardiogram demonstrates atrial fibrillation, non-specific intraventricular conduction delay, and non-specific ST-segment and T wave abnormalities.
The patient is treated with intravenous furosemide with improvement in symptoms and physical exam findings.
Transthoracic echocardiogram demonstrates severe left atrial dilatation, concentric left ventricular hypertrophy, left ventricular ejection fraction of 55% with normal end-diastolic diameter and volume index, and paradoxical septal motion. There is evidence of severe mitral stenosis in the setting of a mitral annuloplasty with an area of 0.7 cm2, mean diastolic gradient between 8 and 11 mm Hg at a heart rate of 70 beats per minute, and trace regurgitation. The aortic valve bioprosthesis has normal function and trace regurgitation. These findings are confirmed on transesophageal echocardiogram.
Right heart catheterization demonstrates mean right atrial pressure of 6 mm Hg, right ventricular pressure of 49/5 mm Hg, pulmonary artery pressure 50/20 mm Hg, and mean pulmonary capillary wedge pressure of 18 mm Hg with a cardiac index of 2.8 L/min/m2 and pulmonary vascular resistance of 3.2 Woods units. Invasive coronary angiography demonstrates mild coronary artery disease.
The patient is diagnosed with symptomatic severe mitral stenosis. Given an elevated Society of Thoracic Surgeons calculated mortality risk of 16.3% and morbidity or mortality risk of 39.4%, the heart team determines that the patient is high risk for surgical therapy. The patient is, therefore, referred for transcatheter mitral valve replacement (MVR).
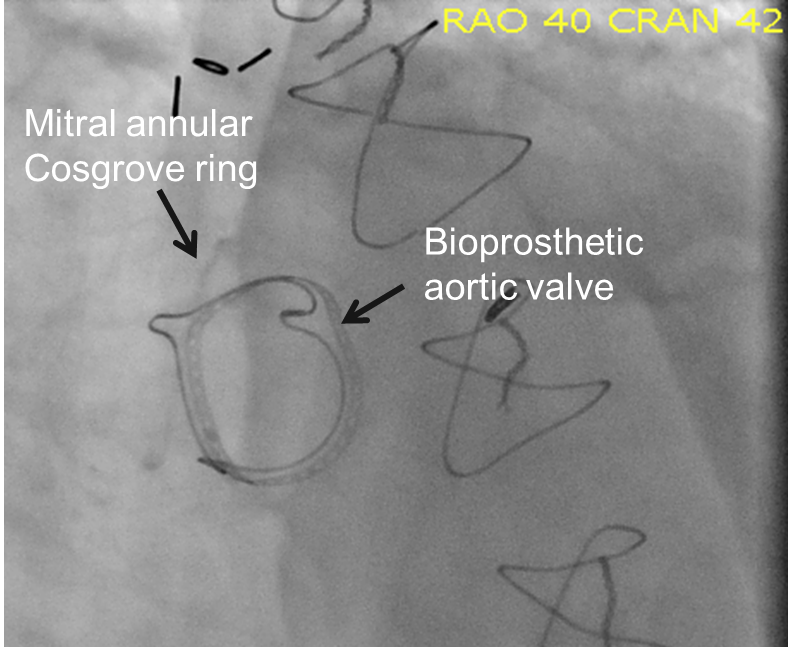
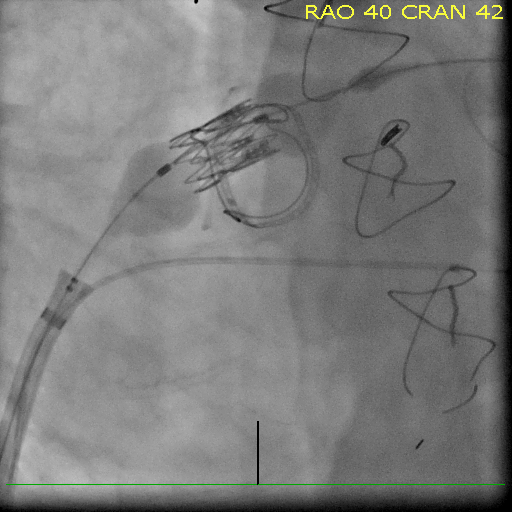
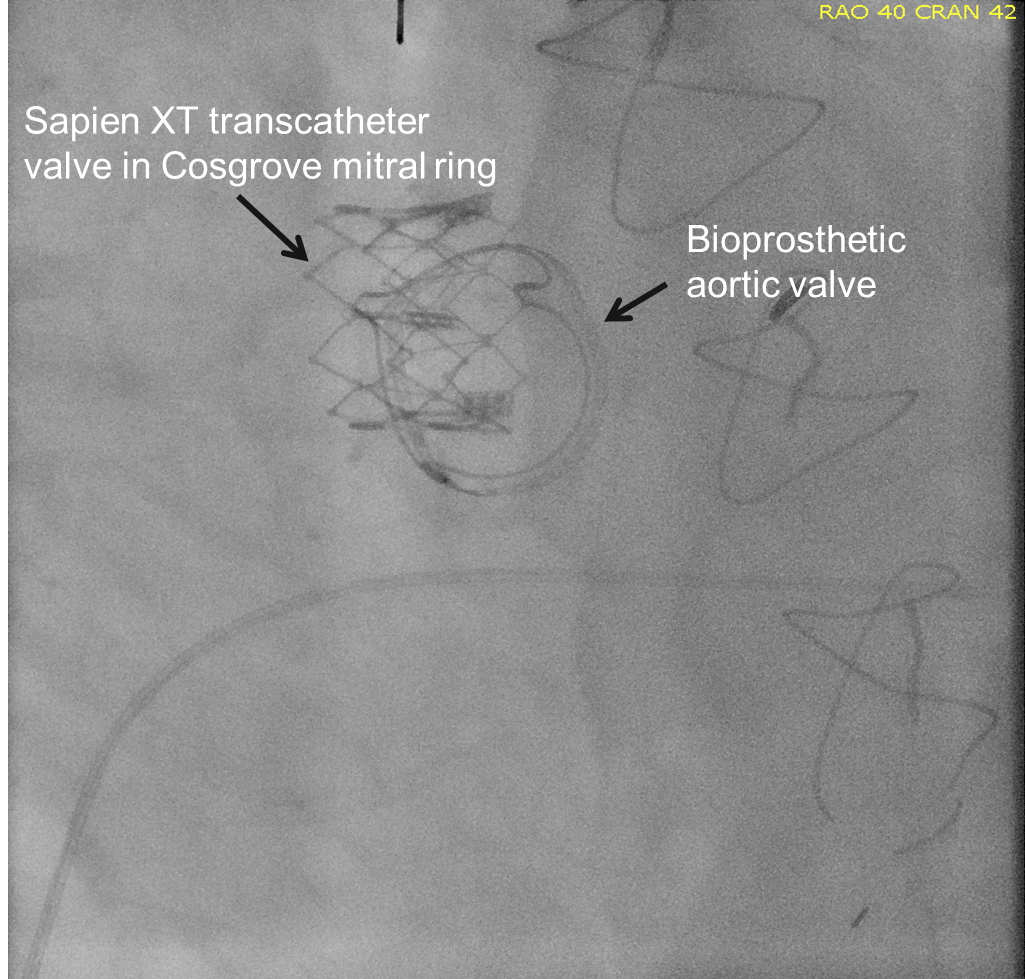
A transvenous pacemaker is placed in the right ventricle. Percutaneous access is obtained via the right femoral vein and an introducer sheath is placed in the right atrium. The mitral annular ring is visualized under fluoroscopy (Figures 1A and 1B). Under transesophageal guidance, a transseptal puncture was performed and an 8.5 Fr introducer is placed in the left atrium positioned towards the mitral valve. A guidewire is placed across the mitral valve and positioned in the left ventricle, and the interatrial septum is dilated using a 14 mm balloon. A 26 mm balloon-expandable transcatheter heart valve is then loaded onto the wire and docked in the inferior vena cava. The valve is positioned in the mitral annulus under fluoroscopic and transesophageal echocardiographic guidance and deployed under rapid pacing (Figures 2, 3A, and 3B).
Post-deployment transesophageal echocardiogram demonstrates excellent position and function of the transcatheter valve with no evidence of significant residual mitral stenosis (mean diastolic gradient 4 mm Hg at heart rate of 85 beats per minute), mild paravalvular mitral regurgitation, and small atrial septal defect at the site of the transseptal puncture. Hemostasis of the femoral vein is achieved using a purse string suture and manual pressure.
The patient experiences no intraprocedural or postprocedural complications and is discharged to an inpatient rehabilitation service on postoperative day seven. At two months follow-up post-procedure, the patient reports no shortness of breath and no interim cardiac events.
Figure 1A: Bioprosthetic Aortic Valve and Mitral Annular Ring on Fluoroscopy
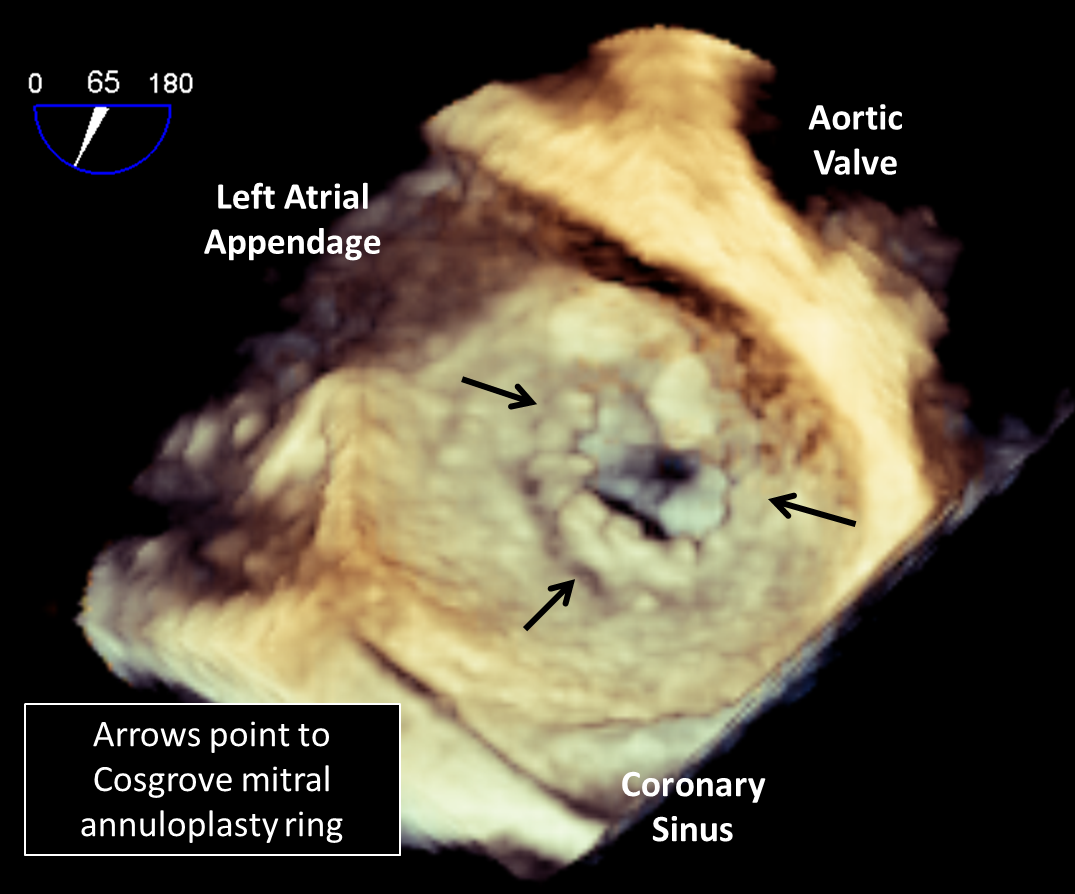
Figure 1B: Bioprosthetic Aortic Valve and Mitral Annular Ring on 3-D Transesophageal Echocardiogram
Figure 2: Deployment of Sapien XT Valve in Mitral Annular Ring
Figure 3A: Post Deployment of Sapien XT Valve in Mitral Annular Ring on Fluoroscopy
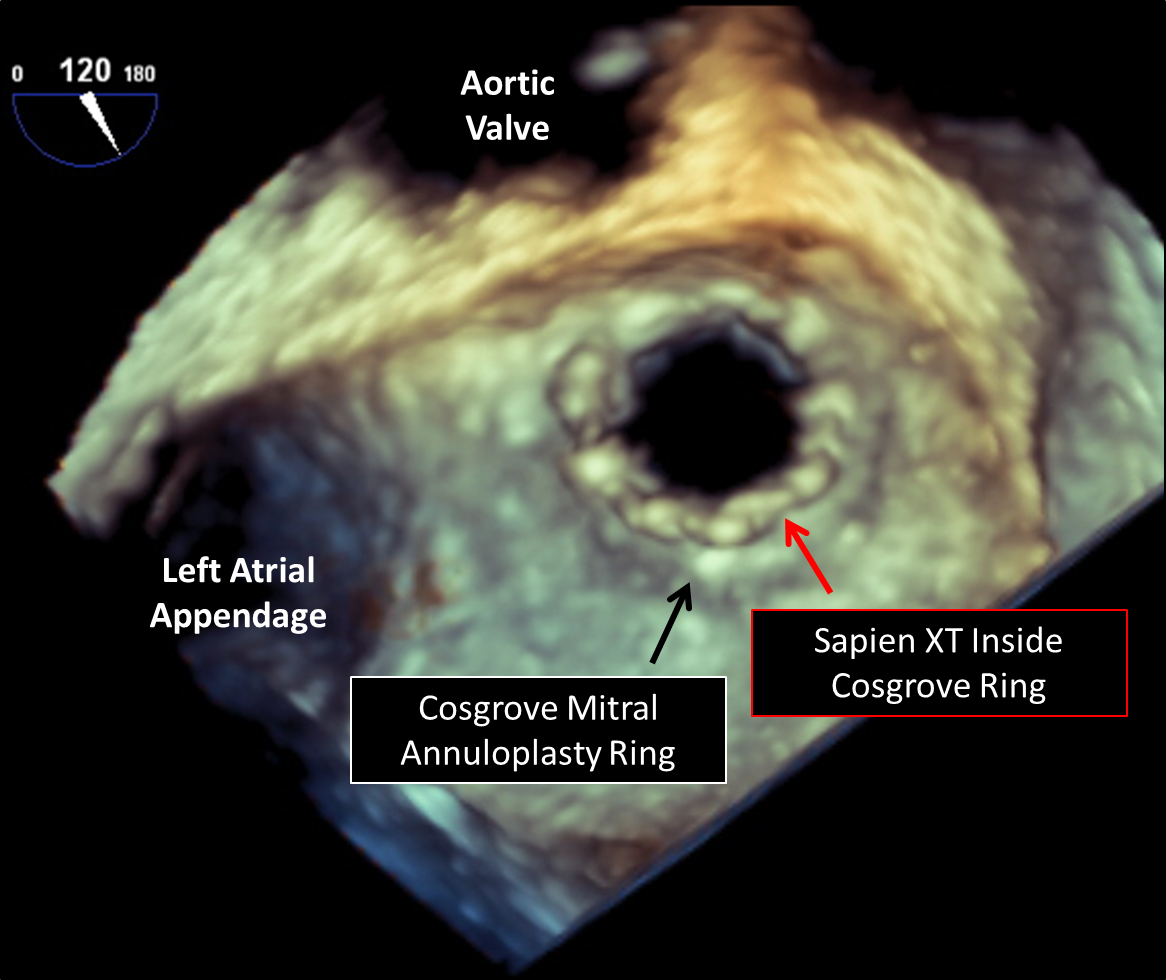
Figure 3B: Post Deployment of Sapien XT Valve in Mitral Annular Ring on 3-D Transesophageal Echocardiogram
Which of the following statements is correct regarding sex and transcatheter heart valve replacement?
Show Answer