Aortic Valve Stenosis: Treatment Disparities in the Underserved
Surgical aortic valve replacement (SAVR) and transcatheter aortic valve replacement (TAVR) are highly effective in treating patients with severe symptomatic aortic stenosis. These cutting-edge innovations have resulted in significant improvements in symptoms, quality of life, and survival in this setting. Nonetheless, access to care is not equal across the spectrum of patients with aortic stenosis. Indeed, only a small proportion of underserved minorities benefit from these interventions. A recently published JACC Council Perspective by Batchelor et al.1 reviews the underlying causes and suggests key strategies to address the disparities in access to care among underserved minorities. The following key points summarize the article.
Who Are the Underserved?
The authors note that in discussing access to care, we must expand our traditional definition of the term underserved. Race, ethnicity, and social determinants of health definitely play major roles, but one must also consider geography (i.e., rural vs. urban) and other factors in this designation because the issue of undertreatment and access to optimal care for patients with structural heart disease is complex.
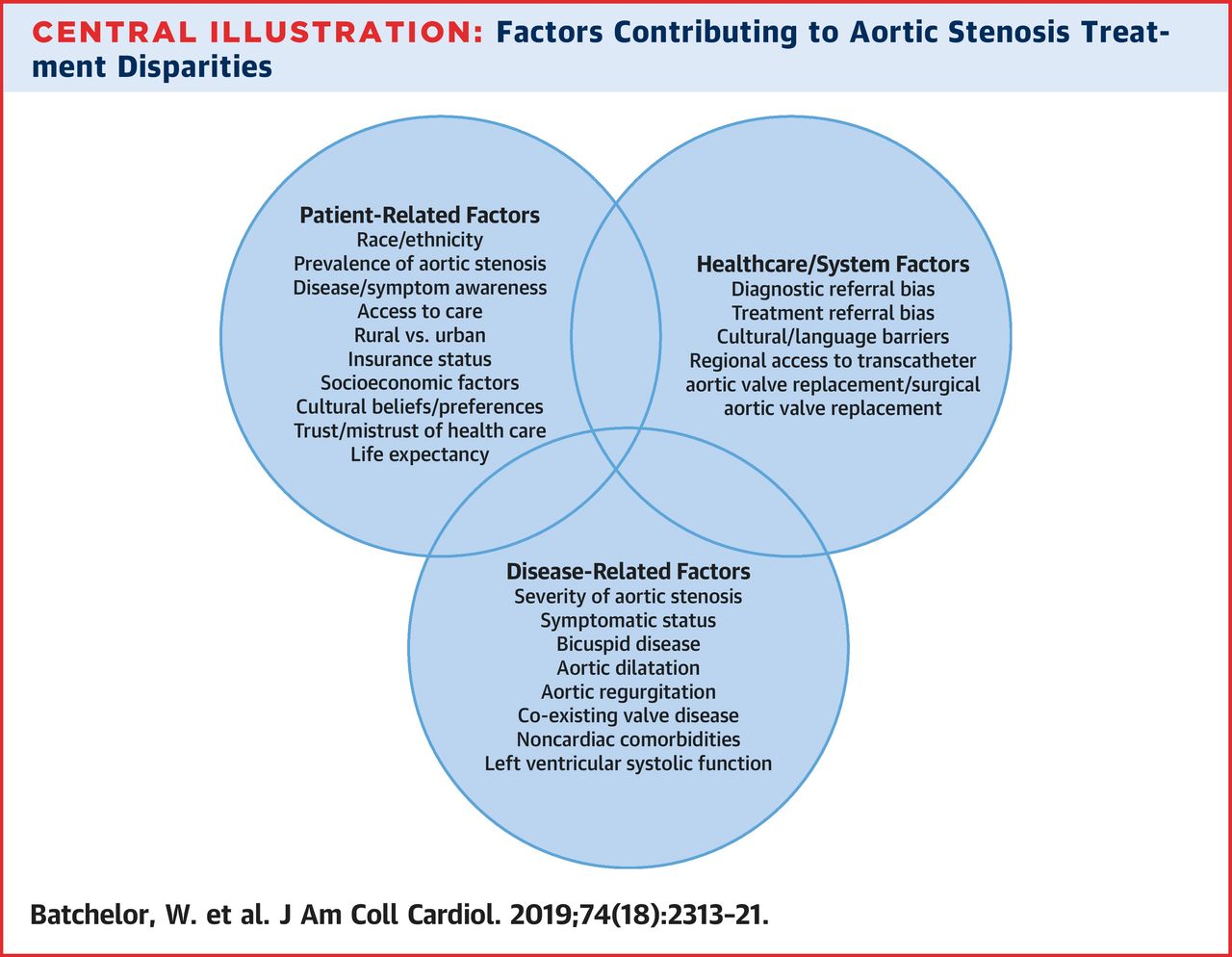
Factors Contributing to Aortic Stenosis Treatment Disparities
Patient-Related Factors
A large number of studies in the literature reports a lower prevalence of aortic stenosis in minorities compared with Caucasians. These differences may be due to disease and symptom awareness, life expectancy, access to healthcare in general (in both rural and urban settings), socioeconomic status, insurance status, and cultural beliefs.
Healthcare/System Factors
Underserved minorities may face substantial referral and treatment biases after receiving a preliminary diagnosis of aortic stenosis from primary care. The root causes of bias are multifactorial and include physician bias and the effects of cultural and/or language barriers.
Disease-Related Factors
Various disease-related factors (severity of aortic stenosis, co-existing aortic dilatation, left ventricular systolic dysfunction, comorbidities, etc.) may also govern the decision to proceed with aortic valve replacement. Whether underserved minorities are more likely to have disease-related factors that render them less likely to undergo treatment is currently unknown. Despite this, it is important to note that underserved minorities who do receive SAVR and TAVR tend to have short-term outcomes that are overall very favorable.
Strategies to Narrow the Treatment Gap
Performance-Measure-Based Quality Improvement
Evaluation of health care providers' performance can be done via examination of patients' electronic health records. For example, determining whether minorities with symptomatic aortic stenosis are adequately referred to the optimal intervention can provide constructive feedback and change behavior.
Promoting Culturally Competent Competition and Team-Based Care
A multidisciplinary heart valve team with an appropriate cultural competency training should be involved in the decision-making process along with the patient. The heart team plays a central role in establishing a strong patient-physician relationship by addressing patient/family concerns and ensuring language concordance and culturally sensitive care.
Improving Patient Access to Health Care, Education, and Research
Access to interventional cardiology and cardiothoracic surgery specialties should be made widely available in underserved areas. In addition, educational campaigns should reach both rural and urban areas to increase disease awareness. Finally, it is important to ensure that clinical trials have adequate minority representation in order to reduce the research gap.
The authors conclude that only a concerted effort from all stakeholders will lead to equitable and broad application of the novel therapies that patients with aortic stenosis and other forms of structural heart disease so desperately need.
References
- Batchelor W, Anwaruddin S, Ross L, et al. Aortic Valve Stenosis Treatment Disparities in the Underserved: JACC Council Perspectives. J Am Coll Cardiol 2019;74:2313-21.
Clinical Topics: Cardiac Surgery, Cardiovascular Care Team, Invasive Cardiovascular Angiography and Intervention, Noninvasive Imaging, Valvular Heart Disease, Aortic Surgery, Cardiac Surgery and VHD, Interventions and Imaging, Interventions and Structural Heart Disease, Angiography, Nuclear Imaging
Keywords: Angiography, Coronary Angiography, Transcatheter Aortic Valve Replacement, Aortic Valve, Cultural Competency, Life Expectancy, Quality Improvement, Dilatation, Quality of Life, Social Determinants of Health, Aortic Valve Stenosis, Heart Valve Prosthesis, Comorbidity, Physician-Patient Relations, Electronic Health Records, Primary Health Care, Decision Making, Insurance Coverage, Referral and Consultation, Health Services Accessibility, Health Personnel, Social Class, Aortic Valve Stenosis
< Back to Listings