Endovascular Management of Chronic Thromboembolic Pulmonary Disease
Introduction
Chronic thromboembolic disease (CTED) is a debilitating complication of pulmonary embolism. Overtime, the organized thrombus gets integrated with pulmonary arterial intima which results in resting pulmonary hypertension, an entity referred to as chronic thromboembolic pulmonary hypertension (CTEPH) or Group 4 pulmonary hypertension, based on the World Health Organization (WHO) classification. This has been reported in 0.56% to 3.2% of all patients with acute pulmonary embolism.1
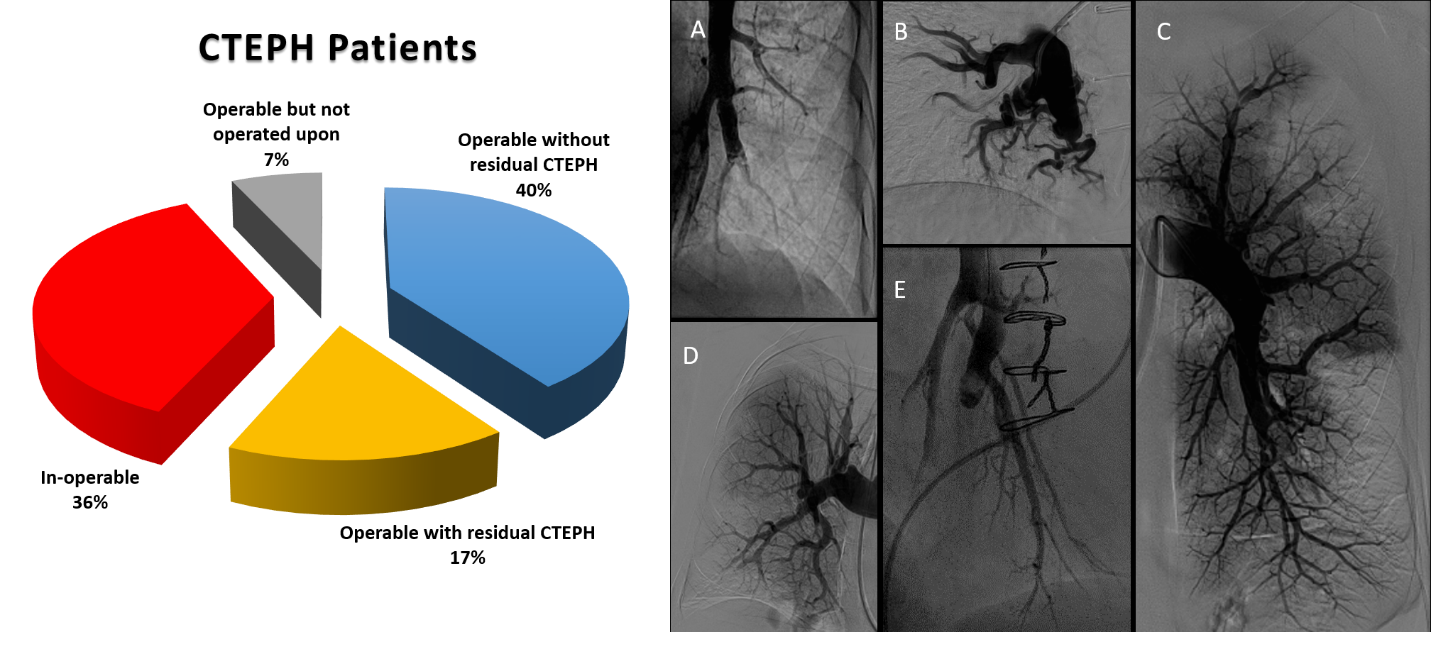
The definitive treatment of choice for this condition is pulmonary thromboendarterectomy (PTE), particularly when the disease involves main, lobar and segmental pulmonary arteries. However, many patients have isolated distal subsegmental disease and therefore are not accessible to surgical thromboendarterectomy. Additionally, there are many patients who are not good surgical candidates due to severe co-morbidities or have residual CTEPH post PTE (Figure 1). Together, these group of patients potentially constitute nearly half of all CTEPH patients2 that are presently eligible for endovascular therapies like balloon pulmonary angioplasty (BPA).
Outcomes of Balloon Pulmonary Angioplasty
Balloon pulmonary angioplasty was initially reported in US in 1988,3 however it was noted to have high complication rates and associated mortality. Therefore, this procedure was very infrequently performed in the US. The procedure has since gained wider adoption in Japan. In fact, to date most of the experience on BPA is from Japan and they have shown a consistent improvement in hemodynamic parameters such as mean pulmonary artery pressures, cardiac outputs, pulmonary vascular resistance and biomarkers like B-type natriuretic peptide (BNP).4 They have also shown significant increase in six-minute walking distances.5 It needs to be kept in perspective that most of these patients treated in Japan with BPA would have been treated with PTE in the US and Europe. Additionally, these observational studies have shown improved survival compared to historical controls.5
Challenges of Balloon Pulmonary Angioplasty
The challenges of BPA are related to complex anatomy of the pulmonary arterial tree, underlying morphology of the recanalized thrombus and lack of dedicated equipment for BPA. Each pulmonary arterial trunk gives rise to numerous tapering branches that are very small compared to the parent vessel. Chronic thromboembolic disease adds to the complexity by further reducing the caliber of these vessels in a non-uniform fashion. Thus, if a branch has ostial total occlusion, sizing the balloon based on the proximal vessel diameter poses a significant risk of rupture and perforation due to the small distal segment of the vessel.
Recanalization of thrombus in the pulmonary artery results in a variety of morphologic lesions with variable angiographic appearances (Figure 1). This makes angiography a very poor imaging modality to assess the severity of stenosis since it only provides one dimensional image of the diseased vessel. As a result, angiographically severe lesions may not always be hemodynamically significant, while milder appearing lesions that are causing significant distal hemodynamic obstruction may easily get missed. Recanalization can also lead to formation of long and tortuous microchannels which can be better seen on histopathological cross section,6 or intravascular ultrasound (IVUS)/ ocular coherence tomography (OCT) imaging.7 Wiring through such microchannels is not always easy. Hence, in case of chronic occlusion such as a pouch-like lesion (Figure 1E) it may be very challenging to wire the distal vessel.
Figure 1
Hemodynamic significant lesions result in a severe discrepancy between proximal and distal pulmonary arterial pressures (Figure 2). Over time, the distal vessels lose the ability to withstand high pressures. Hence revascularization could potentially result in sudden increase in the distal pressure which increases the risk of alveolar hemorrhage. This phenomena has been referred to as reperfusion pulmonary edema and has been the Achilles heel of BPA. The morbidity and mortality associated with pulmonary artery rupture is very high and needs advanced intubation techniques like lung isolation to prevent the blood from flowing into the unaffected lung.8 Lastly, the take-off of the various branches is such that selective cannulation can be very challenging. Hence, there is a huge need for dedicated guides and sheaths for pulmonary circulation. Absence of such dedicated equipment also results in increased use of contrast and radiation during the procedure.
Balloon Pulmonary Angioplasty – Technical considerations
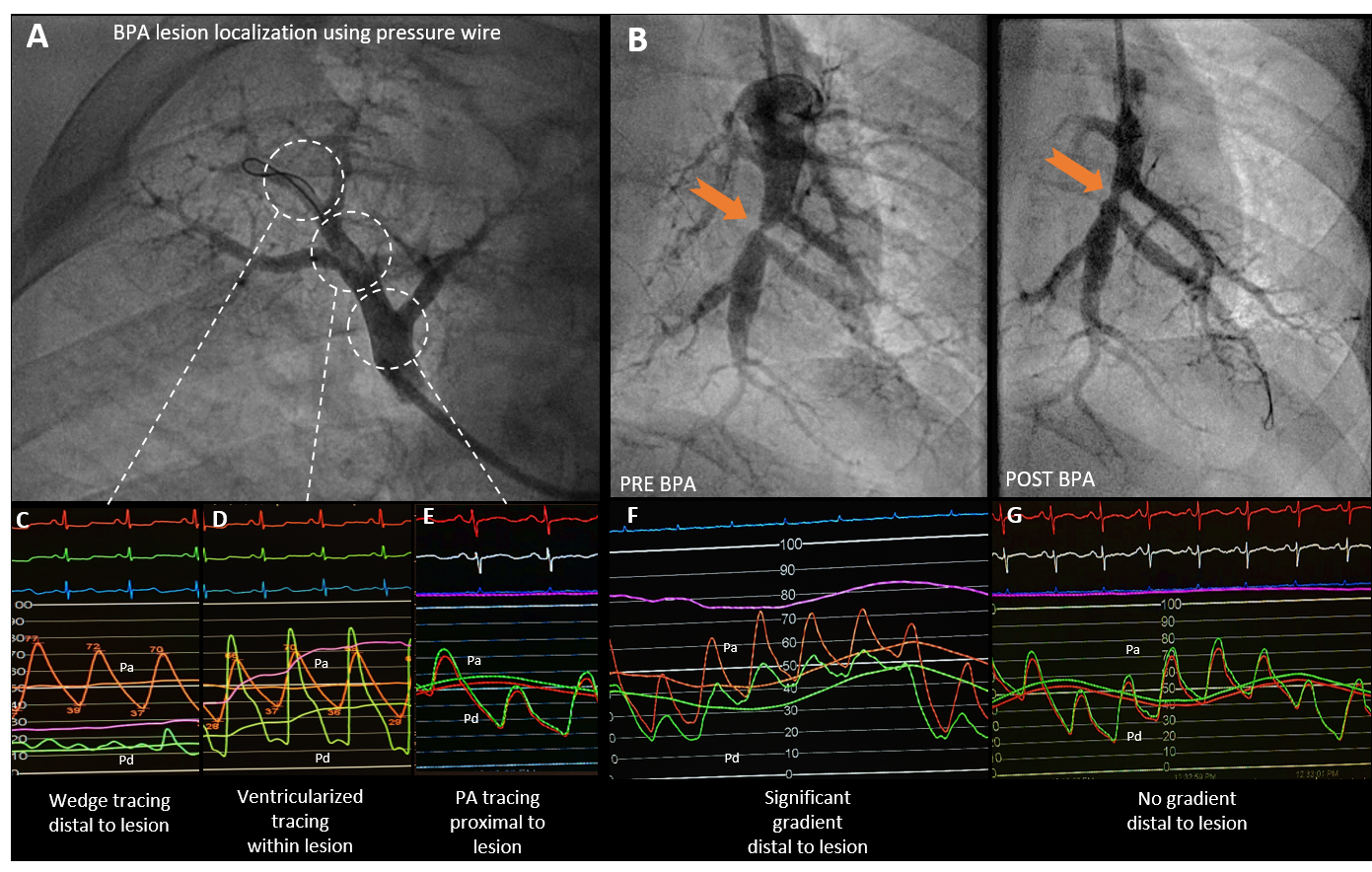
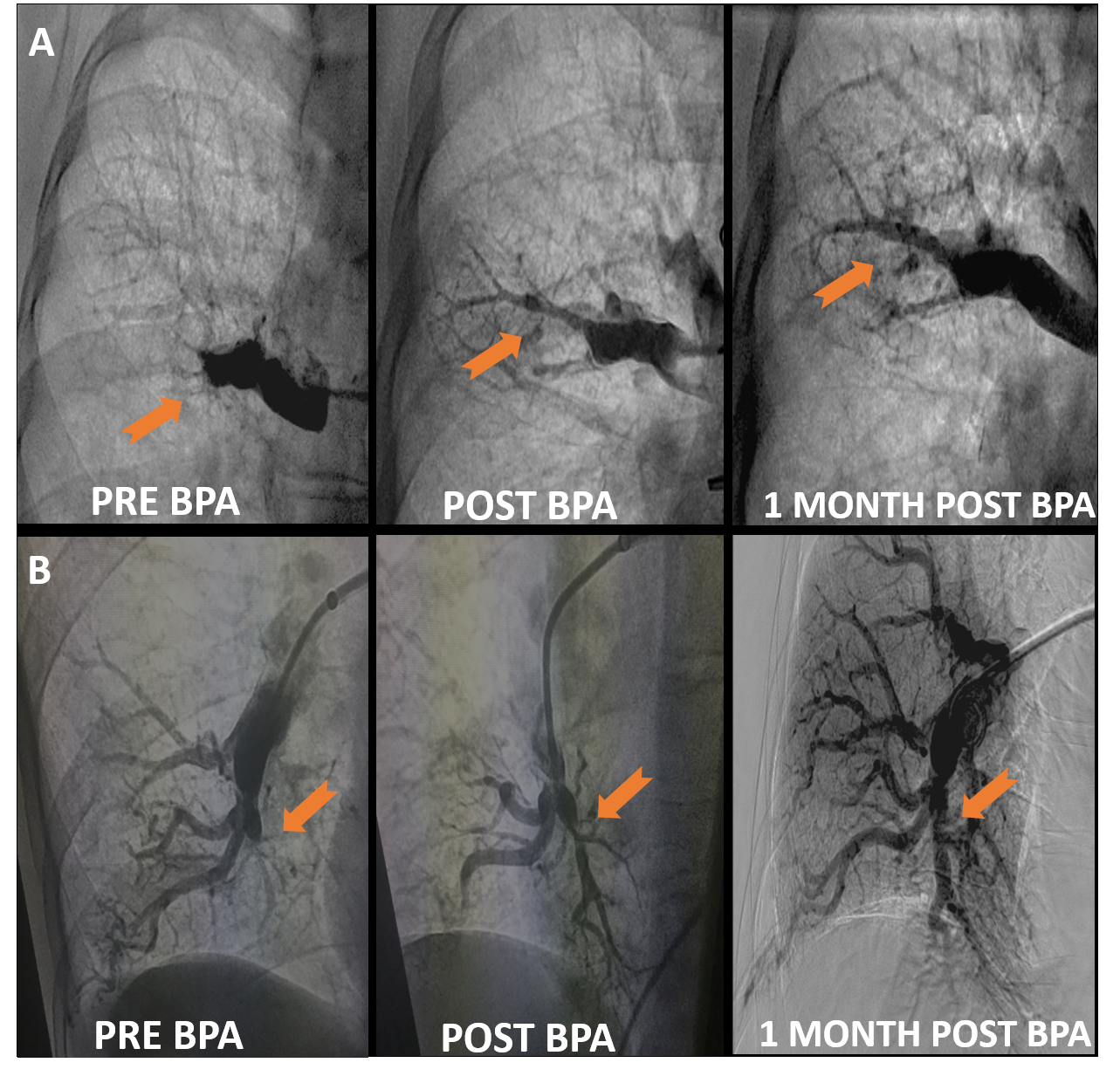
All patients who are referred for BPA are evaluated by our multidisciplinary CTEPH team with baseline studies like ventilation perfusion (VQ) scan, echocardiogram, computed tomography (CT) scan and an invasive pulmonary angiogram. If the team decides that the patient is not a surgical candidate based on anatomic or physiological reasons, he is then referred for consideration of BPA. After an informed consent, which includes the discussion of the unconfirmed benefits as well as risks of pulmonary hemorrhage and death, we perform a right heart catheterization mostly via a femoral approach using a 7F arrow swan that has a 0.035" lumen. We then exchange the swan and the sheath over a 0.035" STORQ™ wire for a 7F 70 cm Flexor® Raabe sheath into the lobar artery. Through this sheath we advance a 6F guiding catheter (usually multipurpose or JR 4) and selectively cannulate a segmental vessel and perform a baseline angiogram. The location of these selective angiograms is decided based on the baseline studies like CT scan, VQ scan and non-selective pulmonary angiogram. Once we identify the lesion, we advance a pressure wire across the lesion and measure the distal pressure and the waveform. The distal waveform in a lesion mostly resembles a pulmonary capillary wedge tracing (Figure 2c). Figure 2 shows examples of patients undergoing pressure wire guided BPA at our Center while Figure 3 shows positive remodeling over time following BPA. Some lesions may have a baseline pulsatile flow distal to the lesion but with a significant gradient (Figure 2f).
Figure 2
Figure 3
Angiographic localization of lesions is often challenging. Therefore, for angiographically ambiguous lesions, a slow pullback of the pressure wire is performed. As the wire is slowly pulled back into the lesion, the distal waveform suddenly changes from a wedge tracing (Figure 2c) to a ventricularized tracing (Figure 2d). Further wire pullback proximal to the lesion changes the waveform to a pulmonary arterial pressure tracing (Figure 2e). Following this the wire is advanced again into the distal vessel. The balloon pulmonary angioplasty is then performed over the pressure wire usually with a small over-the-wire balloon such as a 2.0x12 mm non-compliant balloon, and its effect on distal pressure is monitored continuously. We continue to inflate till the distal pressure is close to but not greater than mean pressure of 35mmHg. The sudden increase in distal alveolar vessel pressure of greater than 35 mmHg mean has been shown to be associated with higher incidence of reperfusion pulmonary edema and alveolar hemorrhage.4 Once a pulsatile flow is achieved distal to the lesion, the same lesion could be further dilated during subsequent sessions till the gradient resolves. Many at times, lesions are such that the pressure wire is not able to cross the occlusion or stenosis (in authors experience it is close to 40%). In such instances, we cross these lesions with regular 0.014" wires like BMW or RUNTHROUGH® and then exchange them for a pressure wire using an over-the-wire (OTW) balloon.
As of July 1st, 2019, our Center has performed 65 BPA sessions on 33 patients. Early data on 17 patients undergoing 66 BPA interventions during 30 sessions (2.2 BPA/session) showed a mean improvement in six-minute walk distance (6MWD) from 342.4 meters to 429.3 meters following completion of BPA sessions. Overall, New York Heart Association (NYHA) functional class improved from Class III to Class II at first month follow up. The mean distal arteriolar pressure per lesion improved from 12.3 mmHg to 28.5mmHg. Amongst this early cohort, the only complication noted was one episode of small volume (<50ml) hemoptysis.
Conclusion
Balloon pulmonary angioplasty has emerged as an adjunctive therapy for patients with inoperable or residual CTEPH. Pressure wire guided BPA can not only help localize angiographically ambiguous lesions but also reduce risk of reperfusion injury. Selection of patients for BPA as well as treatment planning and follow up should involve a multidisciplinary team approach at experienced CTEPH centers. Large clinical trials are needed to further substantiate available observational data on its safety and efficacy. Further dedicated equipment for BPA could help improve procedural challenges and minimize complications in future.
References
- Mahmud E, Madani MM, Kim NH, et al. Chronic thromboembolic pulmonary hypertension: evolving therapeutic approaches for operable and inoperable disease. J Am Coll Cardiol 2018;71:2468-86.
- Mayer E, Jenkins D, Lindner J, et al. Surgical management and outcome of patients with chronic thromboembolic pulmonary hypertension: results from an international prospective registry. J Thorac Cardiovasc Surg 2011;141:702-10.
- Voorburg JA, Cats VM, Buis B, Bruschke AV. Balloon angioplasty in the treatment of pulmonary hypertension caused by pulmonary embolism. Chest 1988;94:1249-53.
- Kataoka M, Inami T, Kawakami T, Fukuda K, Satoh T. Balloon pulmonary angioplasty (percutaneous transluminal pulmonary angioplasty) for chronic thromboembolic pulmonary hypertension: a Japanese perspective. JACC Cardiovasc Interv 2019;12:1382-88.
- Aoki T, Sugimura K, Tatebe S, et al. Comprehensive evaluation of the effectiveness and safety of balloon pulmonary angioplasty for inoperable chronic thrombo-embolic pulmonary hypertension: long-term effects and procedure-related complications. Eur Heart J 2017;38:3152-59.
- Ogawa A, Matsubara H. Balloon pulmonary angioplasty: a treatment option for inoperable patients with chronic thromboembolic pulmonary hypertension. Front Cardiovasc Med 2015;2:4.
- Inohara T, Kawakami T, Kataoka M, et al. Lesion morphological classification by OCT to predict therapeutic efficacy after balloon pulmonary angioplasty in CTEPH. Int J Cardiol 2015;197:23-25.
- Rivers-Bowerman MD, Zener R, Jaberi A, et al. Balloon pulmonary angioplasty in chronic thromboembolic pulmonary hypertension: new horizons in the interventional management of pulmonary embolism. Tech Vasc Interv Radiol 2017;20:206-15.
Clinical Topics: Diabetes and Cardiometabolic Disease, Heart Failure and Cardiomyopathies, Invasive Cardiovascular Angiography and Intervention, Noninvasive Imaging, Prevention, Pulmonary Hypertension and Venous Thromboembolism, Vascular Medicine, Heart Failure and Cardiac Biomarkers, Pulmonary Hypertension, Interventions and Imaging, Interventions and Vascular Medicine, Angiography, Echocardiography/Ultrasound, Nuclear Imaging, Hypertension
Keywords: Aneurysm, Pulmonary Artery, Natriuretic Peptide, Brain, Tomography, Optical Coherence, Constriction, Pathologic, Endarterectomy, Pulmonary Embolism, Hypertension, Pulmonary, Thrombosis, Angiography, Vascular Resistance, Hemodynamics, Cardiac Output, World Health Organization, Angioplasty, Ultrasonography, Interventional
< Back to Listings