Physician Wellness for Pediatric and Congenital Cardiologists: What Can We Do Now?
Quick Takes
- Physician burnout is a concern for pediatric and adult congenital cardiologists.
- Burnout is multifaceted, requiring a multipronged approach to move us from present to an ideal future state.
- Physician and academic society involvement at all levels is essential.
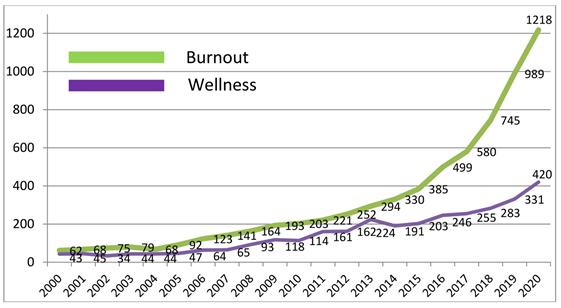
Emphasis has been placed on "wellness" or "wellbeing" in the workplace. "Burnout," a term first coined in the late 1970s and expanded upon by Maslach et al., is the antithesis of wellbeing.1 It has three basic components: high emotional exhaustion, high depersonalization (cynicism), and low personal accomplishment (efficacy). Physicians develop burnout at higher rates than workers in other professions. An early national physician study showed that 45.8% of physicians reported at least one symptom of burnout and were more likely to have symptoms (37.9% vs. 27.8%, p<0.001) and to be dissatisfied with work-life balance (40.2% vs. 23.2%, p<0.001) compared to other workers.2 These findings have been replicated and despite efforts at remediation, levels of physician burnout remain stubbornly high. There has been a surge in the number of publications in this topic.3 (Figure 1)
Figure 1
Reprinted with permission: Vercio C, Loo LK, Green M, Kim Di, Beck Dallaghan GL. Shifting focus from burnout and wellness toward individual and organizational resilience. Teach Learn Med 2021;Feb 15:[Epub ahead of print].
Cardiologists and Burnout
The American College of Cardiology (ACC) has recognized the importance of addressing physician burnout and has incorporated clinician well-being as a "quadruple aim" (along with the three traditional aims of improving population health, enhancing patient experience, and reducing overall costs) in its new strategic plan. Accordingly, the ACC included questions specific to burnout and job satisfaction in its third Professional Life Survey (PLS).4 This showed that 26.8% of adult cardiologists reported being burned out, 19.2% experienced at least one symptom, 6.4% reported chronic symptoms that led to frequently thinking of work frustrations, and 1.2% reported feeling completely burned out to the point of possibly needing outside intervention.5 (Figure 2)
Figure 2
Mehta LS, Lewis SJ, Duvernoy CS, et al. Burnout and career satisfaction among U.S. cardiologists. J Am Coll Cardiol 2019;73:3345-48.
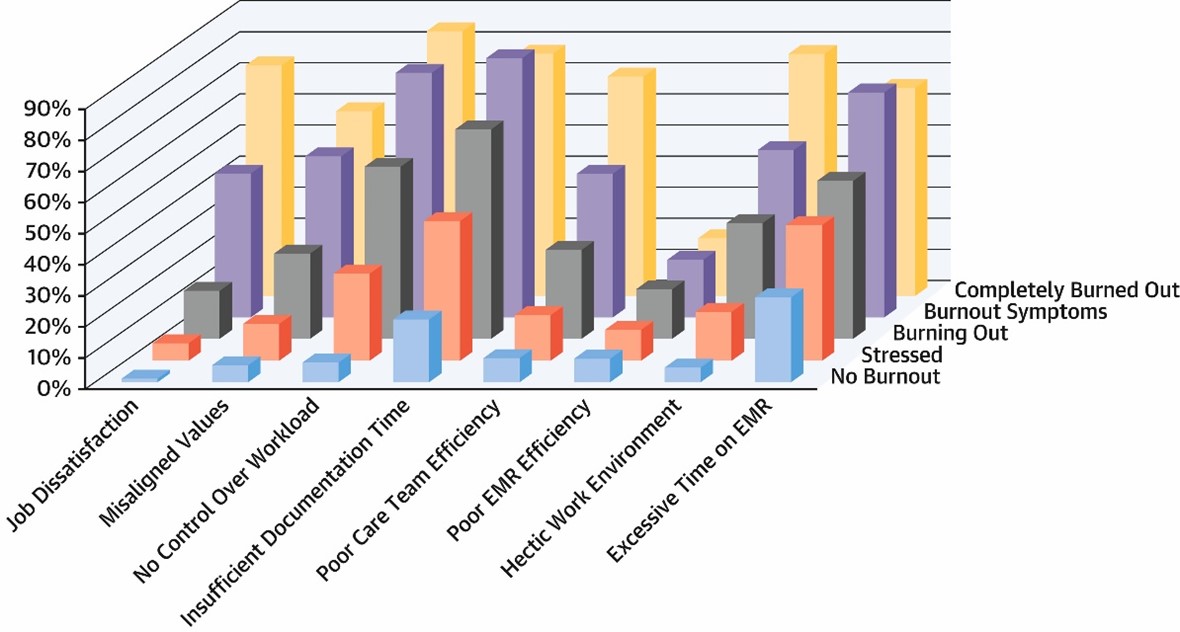
In a study of a large single center group of pediatric cardiologists, two survey tools were employed to evaluate the burnout experience: the Maslach Burnout Inventory, a validated 22-item questionnaire,6 and the Areas of Work-Life Survey, which evaluates six areas of work-life including workload, control, reward, community, fairness and values.7 This revealed emotional exhaustion with 65% of physicians feeling "used up at the end of the workday" at least a few times a month, and 51% "feeling emotionally drained from work" at least a few times a month.8 Workload was similarly a concern in the Areas of Work-Life survey, with 89% of physicians feeling they "worked for prolonged periods of time" and 56% feeling "they have so much work that it takes them away from their personal interests". Key drivers and top overall opportunity themes were identified for intervention at the cardiology divisional level (Figure 3).
Figure 3
Courtesy of Border WL, Asaki Y, Etheridge S, Saidi A.
Understanding Burnout
A review of 182 studies found at least 142 unique definitions of burn-out,9 leading to discrepancies in its reported prevalence. This harms credibility when bringing the problem to administrators at an organizational level or to legislators at a national level. Leiter and Maslach have done work using latent profile analysis to move beyond a binary "burned out versus not burned out" paradigm to one of five distinct experiences: burned out, disengaged, overextended, ineffective, and engaged.10 Although more work is needed in this area, it is clear that the issue is complex and multifaceted. The key is to pick a robust and validated measure that could be assessed at regular intervals to document improvement and adjust wellness strategies based on results.
Moving From the Present to a More Ideal Future State
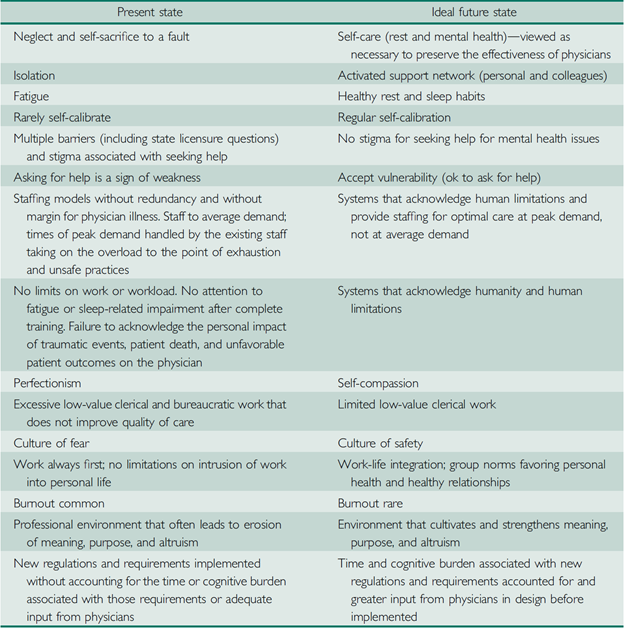
Dr. Tait Shanafelt has brought physician burnout to the forefront. He highlights the incongruence between espoused values (what we say) and artifact (what we do/our behavior) in healthcare and how this has led to a broken professional culture.11 Acknowledgment of this discordance is critical to allow us to move from a broken present state to a more ideal future state (Figure 4).
Figure 4
Reprinted with permission: Shanafelt TD, Schein E, Minor LB, Trockel M, Schein P, Kirch D. Healing the professional culture of medicine. Mayo Clin Proc 2019:94:1556-66.
Involvement at Every Level
Despite a rising awareness, there has been frustratingly little progress in decreasing the rate of burnout with current interventions. A large meta-analysis that included both randomized trials and cohort studies showed that intervention resulted in a decrease in the rate of burnout of only 10%.12 In response to a growing urgency, wellness programs designed to increase resiliency with individually focused sessions have been implemented. While these initiatives are well-intentioned and may offer helpful tools to manage stress,13 a narrowly focused response that includes only physician-directed interventions are unlikely to resolve a much larger systemic problem. Since the problem of physician burnout is multifactorial, solutions must be as well.
Physician burnout should be tackled at five key levels: at the Personal/Individual Level, with the dedication of more resources and training for personal resilience; at the Cardiology Division Level, with regular surveys and engagement of division chiefs;8 at the Organizational Level with comprehensive strategies to promote engagement and reduce burnout;14 at the National Level, with recommendations and frameworks to address the issue such as that provided by the National Academy of Medicine;15 and finally, at an Academic Society Level. This is where the ACC has stepped up and the Board of Trustees has incorporated an initiative to improve clinician wellness in its 2020 to 2023 Strategic Plan.16 The goal is to have all adult congenital and pediatric cardiologists be more informed regarding physician wellness, making it a part of our everyday conversation and engaging at every level to heal our professional culture and enable all of us to have long, fruitful and rewarding careers in medicine.
References
- Maslach C, Jackson SE. The measurement of experienced burnout. J Occup Behav 1981;2:99-113.
- Shanafelt TD, Boone S, Tan L, et al. Burnout and satisfaction with work-life balance among US physicians relative to the general US population. Arch Intern Med 2012;172:1377-85.
- Vercio C, Loo LK, Green M, Kim DI, Beck Dallaghan GL. Shifting focus from burnout and wellness toward individual and organizational resilience. Teach Learn Med 2021;Feb 15:[Epub ahead of print].
- Lewis SJ, Mehta LS, Douglas PS, et al. Changes in the professional lives of cardiologists over 2 decades. J Am Coll Cardiol 2017;69:452-62.
- Mehta LS, Lewis SJ, Duvernoy CS, et al. Burnout and career satisfaction among U.S. cardiologists. J Am Coll Cardiol 2019;73:3345-48.
- Maslach C, Leiter MP. Maslach Burnout Inventory Manual. 3rd ed. Palo Alto, CA: Consulting Psychologists Press; 1996.
- Leiter MP, Maslach C. Areas of worklife: a structured approach to organizational predictors of job burnout. Res Occup Stress Well Being 2003;3:91-134.
- Dasgupta S, Dave I, McCracken CE, Mohl L, Sachdeva R, Border W. Burnout and work-life balance among pediatric cardiologists: a single center experience. Congenit Heart Dis 2019;14:350-55.
- Rotenstein LS, Torre M, Ramos MA, et al. Prevalence of burnout among physicians: a systematic review. JAMA 2018;320:1131-50.
- Leiter M P, Maslach C. Latent burnout profiles: a new approach to understanding the burnout experience. Burnout Research 2016;3:89-100.
- Shanafelt TD, Schein E, Minor LB, Trockel M, Schein P, Kirch D. Healing the professional culture of medicine. Mayo Clin Proc 2019;94:1556-66.
- West CP, Dyrbye LN, Erwin PJ, Shanafelt TD. Interventions to prevent and reduce physician burnout: a systematic review and meta-analysis. Lancet 2016;388:2272-81.
- Patel RS, Sekhri S, Bhimanadham NN, Imran S, Hossain S. A review on strategies to manage physician burnout. Cureus 2019;11:e4805.
- Shanafelt TD, Noseworthy JH. Executive leadership and physician well-being: nine organizational strategies to promote engagement and reduce burnout. Mayo Clin Proc 2017;92:129-46.
- The National Academies of Sciences Engineering, and Medicine, National Academy of Medicine, Committee on Systems Approaches to Improve Patient Care by Supporting Clinician Well-Being. Taking action against clinician burnout: a systems approach to professional well-being. National Academies Press (US) 2019;Oct 23:[Epub ahead of print]..
- Valentine CM. Tackling the quadruple aim: helping cardiovascular professionals find work-life balance. J Am Coll Cardiol 2018;71:1707-09.
Clinical Topics: Prevention, Stress, Congenital Heart Disease and Pediatric Cardiology
Keywords: Job Satisfaction, Work-Life Balance, Workload, Workplace, Frustration, Burnout, Professional, Health Promotion, Reward, Medicine
< Back to Listings