Online Exclusive | From the Member Sections | Optimizing Care of Patients with Hypertensive Disorders of Pregnancy: Putting an Enterprise Plan into Action
As one form of cardiovascular disease, hypertensive disorders of pregnancy (HDP) is a main contributor to maternal morbidity and mortality and adverse fetal outcomes. Readmissions after delivery for those with HDP are high and thought to be largely preventable. Furthermore, the near- and downstream risk of cardiovascular disease due to HDP is clear based on mounting evidence accumulated over the last 20 years.
Representative Case of HDP
Imagine as a cardiologist or cardiology advanced practice provider (APP), you are asked to consult on the following patient for her post-delivery care. What strategy would you use to guide her post-delivery discharge plan?
History of present illness: A 26-year-old female, gravida 2 para 1, at an estimated gestational age of 26 to 27 weeks, with prior preeclampsia, presented to Labor and Delivery with complaints of headache and severe epigastric pain. On arrival, her blood pressure (BP) was 214/118 mm Hg and subsequently within 15 minutes her BP was 190/110 mm Hg.
Past medical history: Preeclampsia during her first pregnancy, which required a preterm delivery at 34 weeks gestation. She was seen only once after delivery, at four weeks postpartum, which was over a year ago. She has not seen a care provider until this presentation. She denies other medical problems.
Diagnostic testing: Fetal ultrasound is remarkable for severe growth restriction and a complete placenta previa. Labs: CBC remarkable for platelets at 90k, CMP revealed elevated AST, ALT >400, and the urine protein:creatinine ratio was abnormal at 0.5 (normal <0.3.)
Assessment: Preeclampsia with severe features based on severe range of hypertension (systolic BP ≥160 mm Hg or diastolic BP ≥110 mm Hg) and lab abnormalities including an elevated AST/ALT (2-times upper limits of normal) and thrombocytopenia (<100K).
Plan: Due to disease severity, early preterm delivery was warranted. She received an initial dose of corticosteroids to enhance fetal maturation and was started on intravenous (IV) magnesium sulfate for fetal/neonatal and maternal neuroprophylaxis. She underwent emergent Caesarean section delivery, and gave birth to a small, premature infant. Initial BPs were managed with IV antihypertensive agents, which were transitioned before discharge to oral medications that are safe during breastfeeding.
But this is not where her care ends.
Case Study: The Care Continues
- Provide patient and provider education and resources about HDP before hospital discharge
- Ensure aggressive in-hospital BP management prior to discharge:
- Consider a short course of furosemide, 5 days at 20 mg daily
- Threshold for target BP before hospital discharge ≤140/90 mm Hg
- Enroll patient in remote BP monitoring, as able
- Plan follow-up for HTN control, lab, symptom monitoring and ongoing education:
- 72 hours for women with severe HDP
- 7-10 days and 6 weeks for all women with HDP
- 3/6/12 months if patient requires antihypertensive medication
- 6/12 months if no longer requires antihypertensive medication
- Offer virtual visits to enhance access to care
- Reassess any abnormalities in labs that remain at discharge. For excessive edema or congestive symptoms order a BNP
- Be clear on treatment goals: BP <140/90 until 6 weeks post-delivery, then <130/80 long-term
- Provide cardiovascular disease risk factor assessment including: diabetes, high cholesterol, overweight, sedentary lifestyle, smoking, non-heart healthy diet, less than ideal sleep patterns. Offer targeted counseling and resources
- Provide risk screening for atherosclerotic cardiovascular disease (ASCVD):
- Consider referrals as needed: primary care, cardiology (stage II HTN, cardiovascular conditions or symptoms, elevated BNP, high-risk comorbidities) and nephrology (persistent proteinuria (>500 mg/24 hours or urine protein:creatinine >0.5), GFR <60 mL/min)
- Offer guidance on contraception post-delivery to avoid unplanned pregnancies
- Provide medication instruction of any teratogenic medications that may be prescribed should the patient become pregnant again, and which are unsafe if patient breastfeeds
- For future pregnancies, low-dose aspirin is indicated to prevent preeclampsia given patient's history of HDP, starting at 12 weeks gestation; consider preconception counseling
Digital Resources (Intermountain Health)
- Care Process Model for Postpartum Management for Patients with Hypertensive Disorders of Pregnancy
- Executive Summary of the Care Process Model for Postpartum Management for Patients with Hypertensive Disorders of Pregnancy
- High Blood Pressure and Pregnancy Fact Sheet
- High Blood Pressure and Pregnancy Fact Sheet in Spanish
Both clinicians and patients recognize there are gaps in care that should be addressed to improve outcomes of patients with HDP. Here we share our experience of how one large health system is addressing these gaps with a clinical pathway that incorporates the latest evidence along with using the Postpartum Hypertension Clinic Development Toolkit developed by ACC's Reproductive Health and Cardio-Obstetrics Member Section.
HDP: The Evidence
HDP is a diagnosis that includes a variety of forms of hypertension (HTN) in the perinatal time including chronic HTN, gestational HTN, preeclampsia, preeclampsia with severe features, and eclampsia (Table).1 A common complication of pregnancy, HDP affects up to 16-20% of pregnant women. It occurs more often in women aged ≥35 years who are Black, non-Hispanic American Indian and Alaska Natives, with low socioeconomic means and living in the South or Midwest regions.2,3
HDP is recognized as a leading cause of postpartum readmission with a doubling of readmission rates from 2010 to 2019.4 Evidence shows that up to 40% of women with HDP will develop chronic HTN, and the diagnosis of HDP serves as a disease marker for increased short-term adverse outcomes including mortality, circulatory shock, peripartum cardiomyopathy, acute kidney injury, preterm labor, stillbirth, and cerebrovascular events during the index admission,5,6 as well as long-term risk of cardiovascular disease.2,7,8 Studies suggest that there is an increased risk of coronary artery disease, myocardial infarction, heart failure and stroke, even in the initial two to five years after a pregnancy complicated by HDP.7,9
Gaps in knowledge and information about the care of women with HDP serve as barriers for those navigating the care transition following a pregnancy, which often results in suboptimal care.10 Even if the information about complications experienced by a patient during pregnancy is effectively communicated to the primary care provider (or gleaned from the medical chart), optimal care and follow-up is dependent on that care provider knowing the associated short- and long-term risks.
A need exists for evidence-based guidelines or standards for postpartum care for HDP, along with consistent, trusted and adequate education and resources for both clinicians and patients that focuses on the seriousness of the condition, with clear blood pressure (BP) thresholds for treatment and urgent care.
With rates of HDP on the rise and the considerable risk of developing chronic HTN and other forms of cardiovascular disease, addressing care during and after delivery is essential. Early aims include early follow-up after delivery to reduce hospital readmission and improve short-term maternal morbidity and mortality. Longer term, consistent follow-up is aimed at modification of risk factors for cardiovascular disease plus early disease detection.11
Innovative models and clinical pathways addressing gaps in care have been proposed that focus on postpartum HTN clinics.12
Additionally, The Postpartum Hypertension Clinic Development Toolkit provides important guidance for starting a clinic. It also addresses aspects of care navigation and follow-up for women after delivery, including 1) BP assessment and management; 2) optimization and management of cardiovascular health; and 3) providing preconception management for any potential future pregnancy.
The use of telehealth with remote BP monitoring as well as virtual visits to facilitate care of busy new mothers also helps increase access.11,12 Given the rising incidence, along with the short-term and long-term risks associated with HDP, this is an area of potential significant impact.
Care Process Model at Intermountain Health
Based on the evidence and many of the needs outlined above, Intermountain Health (a not-for-profit health care system with 385 clinics and 33 hospitals in the Intermountain West) developed a multidisciplinary workgroup to create a system-wide care process model to guide care for patients with HDP after delivery and upon discharge.
Using a literature review and the ACC Postpartum Hypertension Clinic Development Toolkit, we created a clinical pathway, educational tools and an awareness campaign – all of which were reviewed with institutional approval by multidisciplinary teams (maternal fetal medicine, obstetrics, cardiology, nephrology and pharmacy). Guidance is provided on BP targets, medications (including up- and down-titration strategies), and for long-term monitoring and follow-up, including potential referrals. (See Digital Resources sidebar)
BP check and symptom assessment, both by remote patient monitoring and in-person checks; repeat lab evaluations (especially proteinuria and renal assessment); cardiovascular disease risk factor assessment; and patient education are all key components of routine care during visits. Specific process highlights include:
- A 72-hour check for women with severe forms of HDP
- A one-week check for all forms of HDP
- A four-to-six-week check for all patients.
This care process model is now part of key performance indicators for 2026 across our organization.
Looking Ahead
The cardiology community at large needs to understand the short-and long-term implications of HDP. What is clear is that given near- and long-term risk of cardiovascular disease and high maternal morbidity and mortality, education and risk assessment must continue throughout a woman's pregnancy and her lifespan. Understanding the perspectives from patients and care teams and clear multidisciplinary pathways are needed to improve care.
Table. Classification of Hypertensive Disorders of Pregnancy1
Subtypes of HDP |
Definition |
| Chronic HTN | HTN diagnosed prior to 20 weeks gestation |
| Gestational HTN | HTN with new SBP ≥140 mm Hg and/or DBP ≥90 mmHg on at least 2 occasions, 4 hours apart, diagnosed at/after 20 weeks gestation. |
| Preeclampsia | New onset HTN, with SBP ≥140 mm Hg and/or DBP ≥90 mm Hg on at least 2 occasions, 4 hours apart and proteinuria or protein:creatinine ratio ≥0.3 or urine dipstick ≥2+ protein. |
| Preeclampsia with severe features | Preeclampsia with thrombocytopenia, impaired liver function (at least 2x normal or severe right upper quadrant or epigastric pain unaccounted for by other diagnosis); acute kidney injury, pulmonary edema, persistent cerebral or visual disturbances. HELLP syndrome (Hemolysis, Elevated liver enzymes and Low Platelets). |
| Chronic HTN with superimposed preeclampsia | Sudden increase in previously controlled BP or escalation of therapy with any of the following: new onset proteinuria or sudden increase in proteinuria in patients with known proteinuria before or early in pregnancy, and/or significant new end-organ dysfunction with preeclampsia after 20 weeks gestation. |
| Chronic HTN with superimposed preeclampsia with severe features | A sudden increase in previously controlled BP, or SBP ≥160 mm Hg and/or DBP ≥110 mm Hg despite escalating therapy, with any/or all: thrombocytopenia, impaired liver function or severe epigastric pain, new-onset or worsening renal insufficiency, pulmonary edema, persistent cerebral or visual disturbances. |
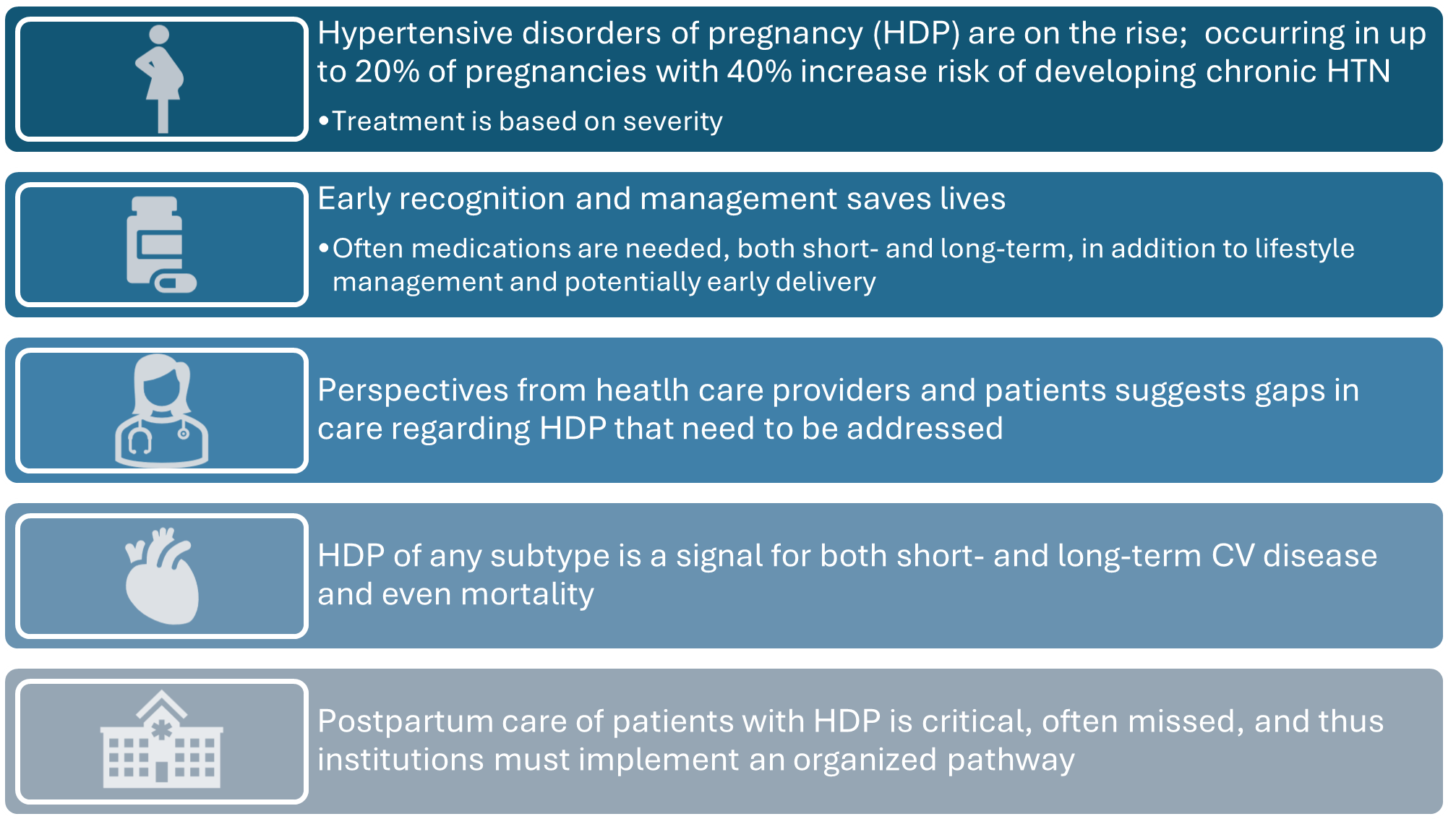
Figure. Key Points About HDP
This article was authored by Kismet Rasmusson, DNP, Advanced Heart Failure and Transplant, clinical professor, co-leader of the Women's Heart Clinical Council; Kirstin Hesterberg, DO, FACC, noninvasive cardiologist, co-founder of cardio-obstetrics program in Denver, Peaks; Donna Dizon-Townson, MD, Maternal Fetal Medicine, medical director of Quality in Obstetrics and Maternal-Fetal Medicine, Women's Health Clinical Council and Vizient OB Quality Steering Committee; and Sarah Iannacone, PharmD, Ambulatory Clinical Pharmacist, member Women's Heart Council; all at Intermountain Health.
References
- August P. Treatment of hypertension in pregnant and postpartum patients. January 26, 2026; Available here. https://www.uptodate.com/contents/treatment-of-hypertension-in-pregnant-and-postpartum-patients
- Rasmusson K, et al. Abstract 4353928: Long-Term Cardiovascular Risks Based on Stratification by Severity of Hypertension Disorders of Pregnancy Disease. Circulation 2025; 152(Suppl_3): p.A4353928-A4353928.
- Ford N, Cox S, Ko J, et al.Hypertensive disorders in pregnancy and mortality at delivery hospitalization - United States, 2017–2019. April 29, 2022. Available here. https://www.cdc.gov/mmwr/volumes/71/wr/mm7117a1.htm.
- Deshpande A, et al. Temporal changes in hospital readmissions for postpartum hypertension in the US, 2010 to 2019; a serial cross-sectional analysis. PLOS ONE. 2025;20(1):e0316944.
- Countouris M, et al. Hypertension in Pregnancy and postpartum: current standards and opportunities to improve care. Circulation. 2025;151(7):490-507.
- Alhuneafat L, et al. Examining maternal and fetal outcomes across various subtypes of hypertension during pregnancy. Int J Cardiol Cardiovasc Risk Prev. 2025;25:200413.
- Honigberg MC, et al. Long-term cardiovascular risk in women with hypertension during pregnancy. J Am Coll Cardiol. 2019;74(22):2743-2754.
- Executive Summary: Reproductive Services for Women at High Risk for Maternal Mortality Workshop, February 11-12, 2019, Las Vegas, Nevada. Am J Obstet Gynecol. 2019;221(4): B2-b5.
- Malek AM, et al. Maternal coronary heart disease, stroke, and mortality within 1, 3, and 5 years of delivery among women with hypertensive disorders of pregnancy and pre-pregnancy hypertension. J Am Heart Assoc.2021;10(5):e018155.
- Wetzler SR, et al. Lived experience of hypertensive disorders of pregnancy: Identifying barriers and improving care. A systematic review and meta-analysis. Int J Gynecol Obstetr. 2025;170(2):576-587.
- Hauspurg A, Jeyabalan A. Postpartum preeclampsia or eclampsia: defining its place and management among the hypertensive disorders of pregnancy. Am J Obstet Gynecol. 2022;226(2s):S1211-s1221.
- Countouris ME, Koczo A. Reproductive healthcare access and the cardiologist's role addressing hypertensive disorders of pregnancy and cardiovascular risk. JACC Adv.2023;2(9):100665.
Clinical Topics: Diabetes and Cardiometabolic Disease, Prevention, Vascular Medicine, Hypertension
Keywords: Cardiology Magazine, ACC Publications, CM-Mar-2026, Pregnancy, Hypertension, Pregnancy-Induced, Cardio-Obstetrics, Hypertension