The 6th World Symposium on PH: PH in Left Heart Disease (Part 2)
Part 1 | Part 2 | Part 3 | Part 4 | Part 5 | Part 6 (Coming Soon!)
Pulmonary hypertension (PH) due to left heart disease is a complex condition encompassing different clinical phenotypes, pathophysiology, and prognoses. In an effort to clarify the disease process and provide clinical guidance, Vachiéry et al. propose a simplified phenotypic and hemodynamic approach in light of recent literature findings.1
PH due to left heart disease is defined as elevated pulmonary pressure in response to elevated left atrial pressure. Elevated left-sided pressures can result from different pathologies, but generally speaking, left heart disease comprises three groups:
- Heart failure with reduced ejection fraction
- Heart failure with preserved ejection fraction (HFpEF)
- Valvular heart disease
Among these subsets, PH can exist as the following:
- Isolated post-capillary PH: Pulmonary artery wedge pressure (PAWP) >15 mmHg and mean pulmonary artery pressure (mPAP) >20 mmHg and pulmonary vascular resistance (PVR) <3 Wood units
- Combined pre- and post-capillary PH: PAWP >15 mmHg and mPAP >20 mmHg and PVR ≥3 Wood units
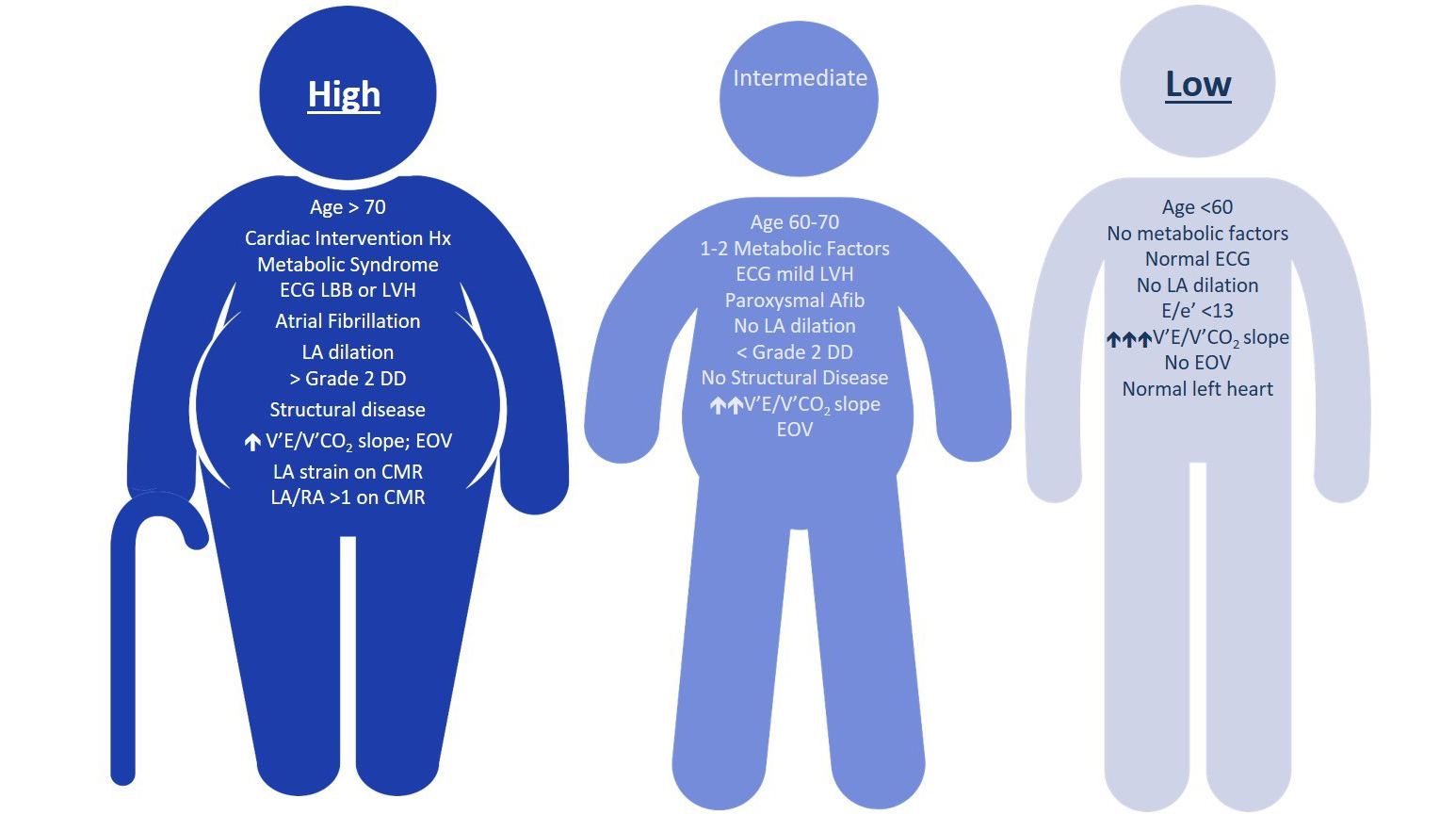
Consistent acquisition of key components during invasive hemodynamic testing with right heart catheterization remains challenging. Also, there is considerable difficulty delineating PH due to left heart disease from pulmonary arterial hypertension (PAH) with HFpEF because PAH patients often have concurrent cardiovascular disease. As such, the authors propose a three-phenotype classification system to refine PH due to left heart disease pre-test probability and stratify which patients require additional invasive studies (Figure 1):
- High probability of left heart disease as a cause of PH. The general management should be guided according to the recommendation for the underlying condition.
- Intermediate probability of left heart disease as a cause of PH. Invasive characterization may be performed in patients with risk factors for PAH (e.g., systemic sclerosis), chronic thromboembolic PH, or in cases of unexplained dyspnea. The presence of right ventricular abnormalities also requires invasive assessment because it may influence management.
Figure 1: Pre-Test Probability of PH due to Left Heart Disease Based on Clinical Phenotype
Resting Hemodynamic Evaluation of PH due to Left Heart Disease
If a patient exhibits an appropriate phenotype to warrant invasive hemodynamic studies, the following are proposed:
- Right heart catheterizations should be performed in stable, non-critically ill patients and should be performed using proper leveling techniques, namely leveling at the mid-chest and "zero"ing the transducer to atmospheric pressure. Patients should be positioned supine with legs flat and pressures recorded during spontaneous breathing (no breath-hold).
- Measure PAWP at end expiration and during end diastole (i.e., typically as the mean of the a-wave) for accurate assessment of PVR with special consideration during atrial fibrillation (when it is appropriate to measure PAWP 130-160 ms after the onset of QRS and before the V-wave).
- Large V-waves should be reported because this strongly suggests left heart disease regardless of resting PAWP.
- If there are discrepancies or ongoing diagnostic uncertainty, provocative testing with exercise testing or fluid challenge to elucidate the diagnosis is useful, particularly to distinguish between healthy subjects and HFpEF or to uncover PH due to left heart disease in patients with PAWP at the upper limit of normal (ULN) (i.e., 13-15 mmHg).
Provocative Hemodynamics
In patients with resting PAWP 13-15 mmHg and high/intermediate probability of PH with HFpEF, provocative testing should be considered to uncover PH due to HFpEF:
- For technical reasons and reliability of pressure recording, a fluid challenge is preferred over exercise in the approach to differential diagnosis.
- An increase of PAWP >18 mmHg after fluid loading in patients with resting values between 13 and 15 mmHg and intermediate/high probability of HFpEF may be considered abnormal.
- The ULN of mPAP during an incremental dynamic exercise challenge has been suggested at >30 mmHg with a cardiac output (CO) <10 L•min−1, which corresponds to a total PVR (total peripheral resistance = mPAP/CO) of 3 Wood units.
- The ULN of PAWP during exercise is thought to be between 15 and 25 mmHg, but higher values can be recorded in elderly subjects. A cut-off value of 25 mmHg is suggested for the diagnosis of heart failure, although PAWP >25 mmHg has been found in elderly individuals free of apparent cardiovascular disease.
- A flow-adjusted measure of PAWP may be more appropriate than PAWP (i.e., PAWP/CO).
Calculations
- Diastolic pressure gradient = diastolic pulmonary artery pressure – Wedge pressure
- Transpulmonary pressure gradient (TPG) = mPAP – Wedge pressure
- PVR = (mPAP – Wedge pressure) / CO
- Pulmonary arterial compliance = stroke volume / (systolic pulmonary artery pressure – diastolic pulmonary artery pressure)
- Pulmonary artery elastance = systolic pulmonary artery pressure / stroke volume
Prognostic Factors
- ↑ Pulmonary artery elastance and ↓ pulmonary arterial compliance associated with worse prognosis
- ↑ TPG, PVR, and diastolic pressure gradient associated with worse outcomes
- ↑ PAWP/CO slope (>2 mmHg•L−1•min−1 is associated with reduced functional capacity, higher N-terminal pro-brain natriuretic peptide, and reduced heart failure-free survival)
Treatment of PH due to Left Heart Disease
- Mainstay of treatment is optimization of underlying left heart disease.
- No PAH therapies have been shown to be beneficial and may even lead to worse outcomes, specifically sildenafil in valvular heart disease post-intervention patients and macitentan in combined pre- and post-capillary PH.
PH in Patients With End-Stage Heart Failure
- Presence of PH signals poor prognosis after transplant. In the context of heart transplantation, PH is associated with an increased 30-day mortality in patients with TPG >15 mmHg and PVR >5 Wood units. Risk of morbidity and mortality increases with progressive elevation in mPAP, TPG, and PVR.
- It is recommended to perform right heart catheterization in all candidates before listing and at 3- to 6-month intervals in listed patients, especially in the presence of reversible PH or worsening heart failure.
- Acute vasodilator testing should be performed if systolic pulmonary artery pressure >50 and TPG ≥15 or PVR >3 Wood units.
- Left ventricular unloading with left ventricular assist device rapidly reverses PH due to left heart disease. Left ventricular assist device recipients with at least one post-implant right heart catheterization without PH likely require less frequent assessments.
References
- Vachiéry JL, Tedford RJ, Rosenkranz S, et al. Pulmonary hypertension due to left heart disease. Eur Respir J 2019;53:1801897.
Keywords: Hypertension, Pulmonary, Pulmonary Wedge Pressure, Stroke Volume, Pulmonary Artery, Natriuretic Peptide, Brain, Atrial Fibrillation, Risk Factors, Blood Pressure, Atrial Pressure, Heart-Assist Devices, Diagnosis, Differential, Diastole, Reproducibility of Results, Sulfonamides, Pyrimidines, Vascular Resistance, Heart Failure, Heart Transplantation, Cardiac Catheterization, Scleroderma, Systemic, Heart Valve Diseases, Dyspnea, Vasodilator Agents, Atmospheric Pressure
< Back to Listings