The 6th World Symposium on PH: Chronic Thromboembolic PH (Part 4)
Part 1 | Part 2 | Part 3 | Part 4 | Part 5 | Part 6 (Coming Soon!)
Chronic thromboembolic pulmonary hypertension (CTEPH) (World Health Organization Group 4) is defined as follows:
- Hemodynamic findings of mean pulmonary artery pressure ≥25 mmHg, pulmonary artery wedge pressure ≤15 mmHg, and pulmonary vascular resistance ≥3 Wood units
- In the presence of chronic, organized thrombi or emboli in the pulmonary arteries that persist despite at least 3 months of effective anticoagulation
The precise pathogenesis of CTEPH remains unclear but appears to be incited by acute pulmonary embolism with resultant altered vascular remodeling and endothelial dysfunction in the pulmonary arterial system. Chronic thromboembolic disease is characterized by similar symptoms and perfusion defects but without pulmonary hypertension at rest. CTEPH is an underdiagnosed condition that often presents with non-specific symptoms and requires a high index of clinical suspicion. Lung ventilation/perfusion scintigraphy is the screening test of choice; however, this test is infrequently ordered despite guideline recommendations.
Diagnosis is made by the following:
- History revealing signs and symptoms suggestive of CTEPH.
- Transthoracic echocardiography revealing evidence of pulmonary hypertension.
- VQ scan is the initial imaging test of choice. It has a high sensitivity and specificity. If there is no evidence of mismatched perfusion defect, CTEPH is effectively excluded.
- Computed tomography pulmonary angiogram then confirms diagnosis and assesses operability.
- Right heart catheterization and digital subtraction angiography are used to obtain invasive hemodynamics and determine accessibility of thrombi.
Treatment
- Lifelong anticoagulation therapy.
- Definitive therapy should be made by an expert CTEPH team.
- Operable with acceptable risk/benefit: pulmonary thromboendarterectomy (treatment of choice).
- Non-operable or operable with unacceptable risk/benefit: Targeted medical therapy and/or balloon pulmonary angioplasty (BPA).
- Persistent/recurrent symptomatic pulmonary hypertension: consider re-do surgery versus targeted medical therapy and/or BPA.
- Riociguat is approved for inoperable CTEPH (CHEST [A Study to Evaluate Efficacy and Safety of Oral BAY63-2521 in Patients With CTEPH]1).
- Macitentan also showed benefit for inoperable CTEPH (MERIT-1 [Clinical Study to Assess the Efficacy, Safety and Tolerability of Macitentan in Subjects With Inoperable Chronic Thromboembolic Pulmonary Hypertension]2).
- Unclear benefit of medical therapy as a bridge to pulmonary thromboendarterectomy surgery or as a bridge to BPA. Combining endarterectomy with BPA either as a hybrid or stepwise approach is being evaluated at select expert programs.
Summary
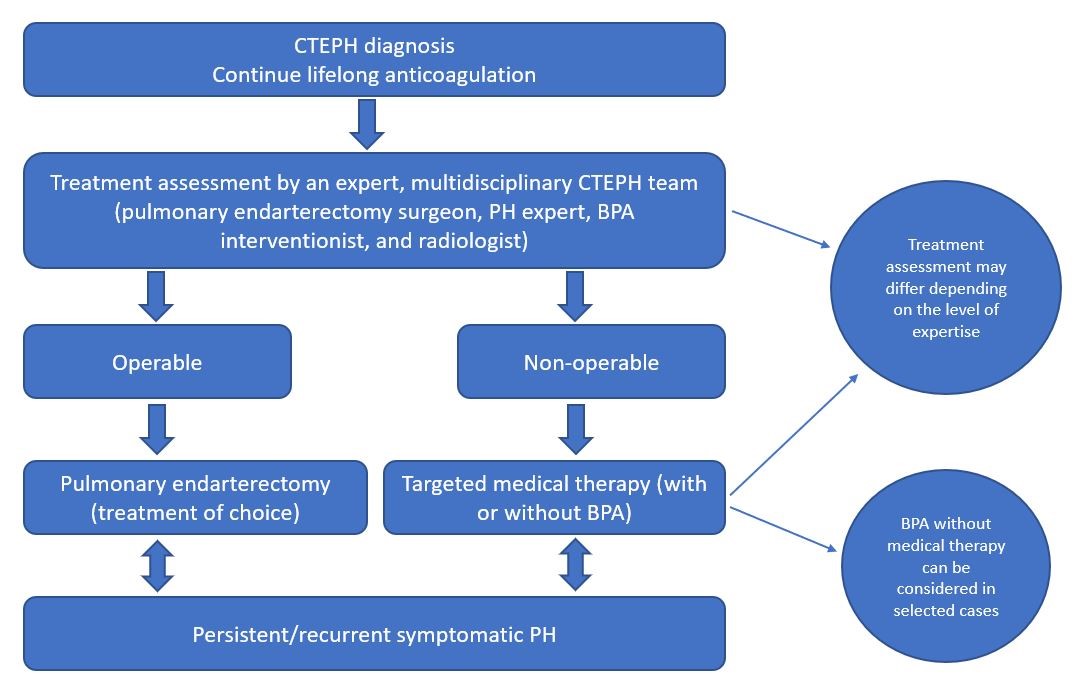
Pulmonary endarterectomy remains the treatment of choice for operable CTEPH. For those deemed inoperable, the best level of evidence supports initiation of medical therapy and consideration for BPA.
Figure 1: CTEPH Revised Treatment Algorithm3
References
- Ghofrani HA, D'Armini AM, Grimminger F, et al. Riociguat for the treatment of chronic thromboembolic pulmonary hypertension. N Engl J Med 2013;369:319-29.
- Ghofrani HA, Simonneau G, D'Armini AM, et al. Macitentan for the treatment of inoperable chronic thromboembolic pulmonary hypertension (MERIT-1): results from the multicentre, phase 2, randomised, double-blind, placebo-controlled study. Lancet Respir Med 2017;5:785-94.
- Kim NH, Delcroix M, Jais X, et al. Chronic thromboembolic pulmonary hypertension. Eur Respir J 2019;53:1801915.
Keywords: Hypertension, Pulmonary, Pulmonary Artery, Pulmonary Wedge Pressure, Angiography, Digital Subtraction, Endarterectomy, Pyrimidines, Pulmonary Embolism, Pyrazoles, Sulfonamides, Vascular Resistance, Angioplasty, Echocardiography, Cardiac Catheterization, Perfusion Imaging, Tomography
< Back to Listings