Poll Results: Management of DAPT Post ACS
Quick Takes
For patients undergoing PCI for ACS, comparison of short DAPT to de-escalation of DAPT demonstrated:
- No difference in all-cause death, while short DAPT reduced major bleeding risk, and de-escalation was associated with reduced net adverse cardiovascular event(s) (NACE).
- These results imply that that DAPT strategies can potentially be optimized by matching patient risk characteristics to treatment strategies.
This Poll was stimulated by a recent publication1 assessing the comparative risk of treatment strategies to reduce bleeding risk without increasing thrombotic events compared to more traditional, extended dual antiplatelet treatment (DAPT). While prior studies have noted benefits for the two modified DAPT regimens, no comparative data were previously available on the comparative efficacy of the two regimens. To compare the two strategies, a meta-analysis was performed including 29 studies which met predefined criteria representing 50,602 patients.
In patients with acute coronary syndrome (ACS) undergoing percutaneous coronary intervention (PCI), there was no difference in all-cause death between short DAPT and de-escalation. De-escalation reduced the risk for net adverse cardiovascular event (NACE), while short DAPT decreased major bleeding. These data characterize two contemporary strategies to personalize DAPT based on treatment objectives and patient risk profile.
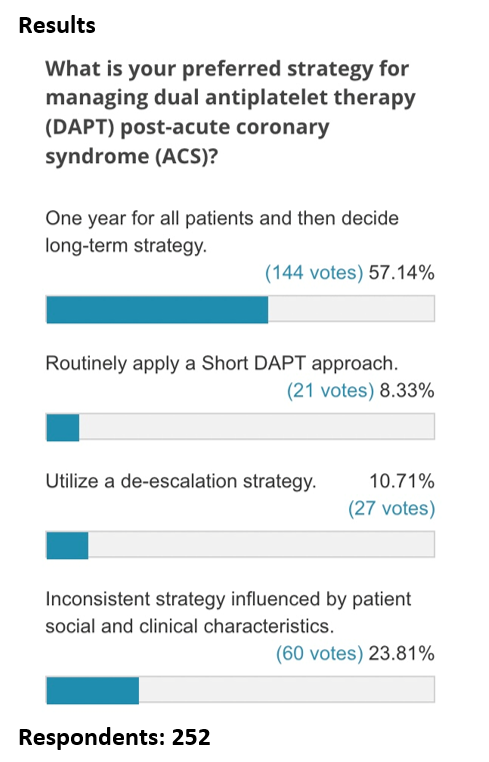
The poll sought to determine how physicians approach this clinical scenario. Over half of respondents (57%) follow the traditional 1 year or longer approach, while 8-10% of respondents each chose one of the modified DAPT regimens. Interestingly, nearly one quarter of respondents chose a patient centric approach based on clinical patient characteristics. Derived from the meta-analysis by Laudani et al.,1 a more flexible patient guided risk profile may be the optimal approach.
References
- Laudani C, Greco A, Occhipinti G, et al. Short duration of DAPT versus de-escalation after percutaneous coronary intervention for acute coronary syndromes. JACC Cardiovasc Interv 2022;15:268–77.
Clinical Topics: Acute Coronary Syndromes, Invasive Cardiovascular Angiography and Intervention, Interventions and ACS
Keywords: Platelet Aggregation Inhibitors, Percutaneous Coronary Intervention, Acute Coronary Syndrome, Hemorrhage, Patient-Centered Care, Surveys and Questionnaires, Physicians
< Back to Listings
