Prioritizing Health | Proactive Screening Doubles Early CVD Diagnosis in Community
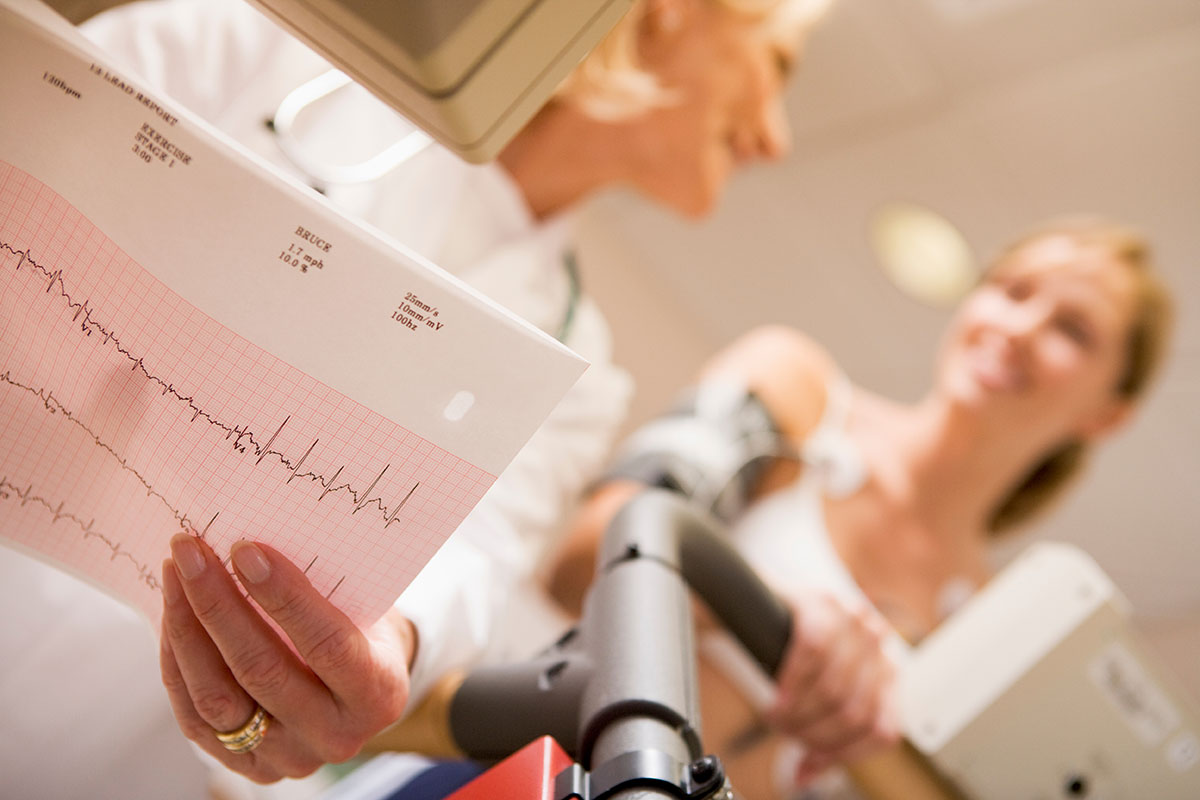
Finding cardiovascular disease earlier means earlier treatment and better prevention and fewer outcomes. An easy systematic screening strategy carried out by primary care clinicians in the RED-CVD trial more than doubled the number of new diagnoses among a high-risk population of patients with type 2 diabetes (T2D) or chronic pulmonary obstructive disease (COPD).
In the trial, presented at ESC Congress 2023, 25 primary care practices across the Netherlands were randomly allocated to provide routine care (control group) or to add an early diagnosis strategy to their usual disease-management programs for T2D and COPD (intervention group). Of the 1,216 patients, 87% had T2D and 20% had COPD; their average age was about 68 years and 40% were women.
The intervention involved three steps:
- A questionnaire on risk factors and symptoms patients completed before their next routine visit.
- For patients who scored above a prespecified threshold on the questionnaire, a physical examination by the practice nurse during a routine visit to assess signs for heart failure (HF), including a 12-lead ECG and NT-proBNP measurements.
- Referral to a cardiologist or open access echocardiography, based on the assessment of Steps 1 and 2 by the PCP.
The primary outcome was a composite of newly detected cases of HF, atrial fibrillation (AFib) and coronary artery disease (CAD) at one year after the baseline visit. Secondary endpoints included newly initiated treatments.
At one year, 50 of 624 patients in the intervention group and 19 of 592 patients in the control group were newly diagnosed with at least one primary outcome disease. HF was the most common new diagnosis (4.5%) in the intervention group, followed by CAD (2.6%) and AFib (2.1%) – more than twofold the rates for each in the control group. No major differences in medication use at follow-up were observed between the groups.
"An easy-to-implement strategy more than doubled the number of new diagnoses of HF, AFib and CAD in high-risk patients," said Amy Groenewegen, MD, of the University Medical Centre Utrecht. "Because there are so many adults in the community with COPD or type 2 diabetes, this approach could translate into tens of thousands of new diagnoses when applied at large. In the Netherlands, for example, screening the more than 920,000 patients with COPD and/or type 2 diabetes could identify over 44,000 patients with at least one previously undiagnosed cardiovascular condition."
SGLT2 Inhibitors Don't Improve Survival in COVID: Meta-Analysis

A meta-analysis conducted by the World Health Organization Rapid Evidence Appraisal for COVID-19 Therapies Working Group found that SGLT2 inhibitors did not lead to lower 28-day all-cause mortality compared with usual care or placebo in patients hospitalized with COVID-19. The study, presented at the ESC Congress 2023, included aggregate data from the DARE-19, RECOVERY and ACTIV-4A trials which evaluated SGLT2 inhibitors in this setting.
Overall, these trials randomized 6,096 participants to SGLT2 inhibitors (n=3,025) and to usual care or placebo (n=3,071), across the U.S., UK, Brazil, Canada, Mexico, Argentina, India, Spain, Nepal, Indonesia, Vietnam, South Africa and Ghana. The average age of participants ranged between 62 to 73 years, 39% were women and 25% had type 2 diabetes at randomization.
In the SGLT2 inhibitor group vs. usual care or placebo group, there were 351 deaths vs. 382 deaths, for a summary odds ratio of 0.93 for SGLT2 inhibitors, with consistency across trials. This finding corresponded to an absolute mortality risk of 11.7% for SGLT2 inhibitors compared with an assumed mortality risk of 12.4% for usual care or placebo, according to the researchers.
Similar results were seen for in-hospital and 90-day all-cause mortality, although data were available from only the DARE-19 and ACTIV-4A trials. No significant differences were seen for progression to acute kidney injury, requirement for dialysis or death and progression to invasive mechanical ventilation, extracorporeal membrane oxygenation or death at 28 days.
"We found no convincing evidence that administration of SGLT2 inhibitors, compared with usual care or placebo, reduces 28-day all-cause mortality, or improves other pre-specified efficacy outcomes," said Mikhail Kosiborod, MD, FACC. "No new safety signals were observed with the use of SGLT2 inhibitors in this patient population, and their routine discontinuation during acute illness for patients that receive them for other indications such as heart failure, chronic kidney disease, or type 2 diabetes does not appear to be warranted."
Tools You Can Use

Build a customized risk-lowering plan for your patients by estimating and monitoring change in 10-year ASCVD risk using ACC's ASCVD Risk Estimator Plus.
Enhance conversations with patients about common heart problems using CardioSmart's Heart Explorer, with its enhanced high-resolution cardiac graphics and animations.
Visit ACC.org/MobileResources to download them today (and explore all the apps available for download).
Clinical Topics: Arrhythmias and Clinical EP, Heart Failure and Cardiomyopathies, Atherosclerotic Disease (CAD/PAD), Atrial Fibrillation/Supraventricular Arrhythmias, Acute Heart Failure
Keywords: ACC Publications, Cardiology Magazine, Cardiovascular Diseases, Atrial Fibrillation, Diabetes Mellitus, Type 2, Coronary Artery Disease, Heart Failure
< Back to Listings

