Feature | Navy Cardiology: Serving the Heart of the Military
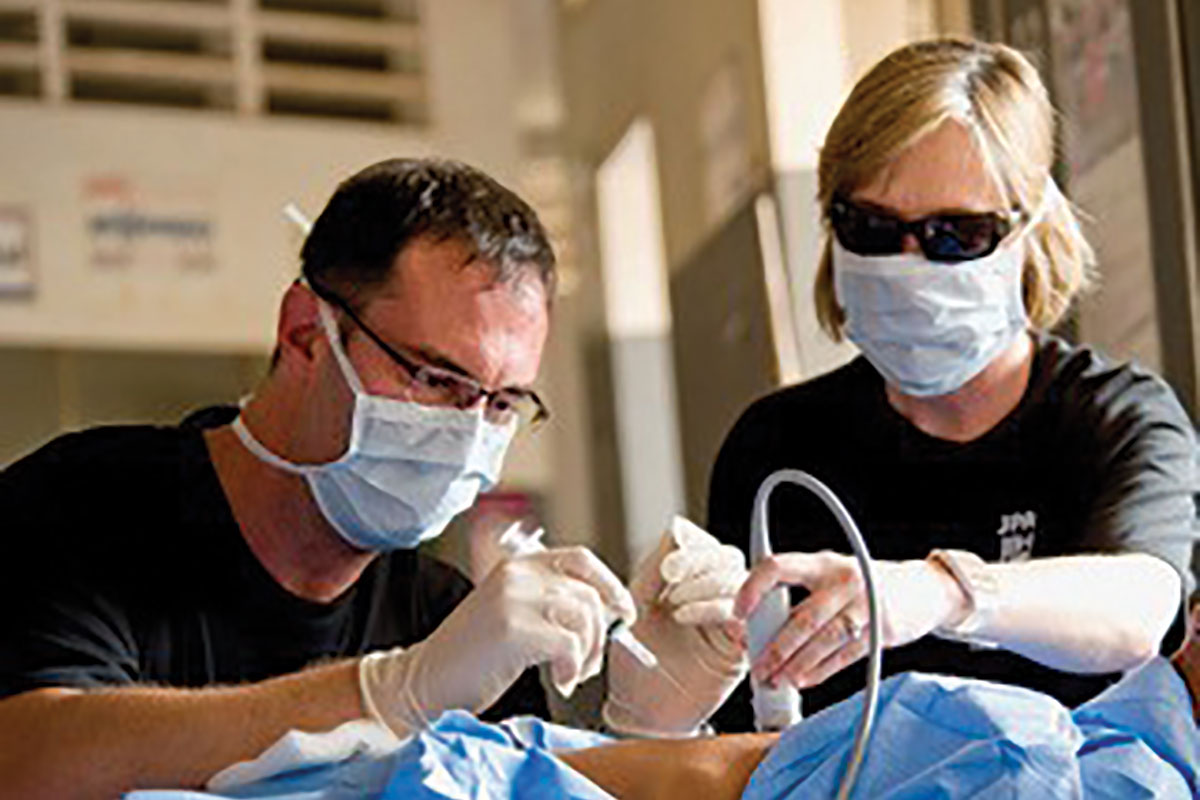 Captain (retired) M. Alaric Franzos, MD, MPH, FACC, in the field.
Captain (retired) M. Alaric Franzos, MD, MPH, FACC, in the field.
Cardiology – and in fact all primary and secondary prevention – looks a little different in the military, which relies on a healthy population to perform hazardous jobs, often in dangerous and remote locations far from advanced medical services. In this second part of a two-part series on Navy Medicine, Cardiology explores the specialized world of military cardiology and its vital role in maintaining a healthy, mission-ready force.
The Warrior Athlete
With more than 340,000 personnel on active duty and another 100,000-plus in ready reserve, the United States Navy is the third largest of the U.S. military service branches in terms of personnel.
"I would say the big difference between the military and the civilian world is that in the civilian world, it's about what's best for the patient. For our service members, we have a dual mission: to do what's right for the patient and what's right for the military regarding the patient and their continued service, and to try to determine how can we help them serve in optimum health," Commander Travis Harrell, MD, FACC, tells Cardiology.
Service members are often referred to as warrior athletes or tactical athletes, says Captain (retired) M. Alaric Franzos, MD, MPH, FACC. "And just like in the civilian world, we have our own elite warrior athletes, like Navy Seals or Marine Raiders, who have tremendously difficult jobs that oftentimes require great strength and endurance, and where any significant morbidity can be fatal or even jeopardize the mission. So it's very important that we give some degree of confidence to them and their commanders that they can complete the mission at hand."
To Screen or Not To Screen?
The military stopped universal ECG screening in 2001 because of the unacceptably high false-positive rate and low probability of an event. With the new criteria for ECG interpretation in athletes in 2017, the false-positive rate has dropped from 20-25% to <2%.1
"We have ECG screening programs in place at all the military service academies that combine the AHA's 14-element history and physical with the new recommendations and we're seeing an overall ECG false positive rate of 1.1%," says Franzos.
"Only 0.04% of those screened were found to have a cardiac condition associated with sudden cardiac death (SCD) such as hypertrophic cardiomyopathy (HCM). But in the military, HCM and other SCD-related cardiac conditions convey a risk to the individual and to the unit and mission, making early identification crucial."
One can have heart disease and still serve in the military, Harrell adds, but the parameters differ from the civilian world. "For example, a service member who needs a stent can't be deployed while on dual antiplatelet therapy, but once they are healthy enough to exercise without symptoms and stop the P2Y12 inhibitors, we can return them to deployable status."
Another example might be a relatively benign arrythmia that would in the civilian world probably go untreated. "Our EP labs are pretty busy ablating supraventricular tachycardias and atrial fibrillation because, depending on the antiarrhythmic they are on, they may not be eligible to continue to serve. To avoid this, we might ablate earlier than might happen outside the military," says Harrell. "Of course, all of this is discussed with the service member and done with informed consent."
There are duty standards for joining the military and then another set of medical standards for retention in the event a service member is found to have a medical condition or is injured, says Captain Dylan Wessman, MD, FACC, in an interview. On top of this, each service – Navy, Army, Air Force, Marines – has their own medical standards for performing special duties within that service.
"In the Navy we have the Manual of the Medical Department, MANMED for short, which delineates the physical and medical requirements for Navy and Marine Corps personnel undertaking special duties, like flight, diving, submarine duty or special operations. These standards are notably more conservative than would apply to the average citizen or even a professional athlete who can access medical care relatively quickly."
"Our people go out to sea, they go under the sea, they go to parts of the world that are underdeveloped and they even go to places that may be hostile, so we have to be very selective in who we let do those kinds of things," he adds.
With MANMED running to 23 chapters, it's easy to see why the Navy relies on its specially trained cardiologists and other physicians to evaluate accession, retention, disability and deployability in the service, ensuring the maintenance of a robust and capable force.
Becoming a Navy Cardiologist
 Department of Defense
Department of Defense
There are between 25 and 30 cardiologists in the Navy at any given time, says Wessman, all of whom have permanent duty stations at medical treatment facilities (called, MTFs in Navy parlance) within the continental U.S. "Sometimes we're deployed, to one of the hospital ships or in support of combat operations for a period of time, but we don't have people who are routinely deploying on ships for long periods of time."
Some of the Navy's cardiologists attend medical school at the federal government's Uniformed Services University of the Health Sciences, but many, including Wessman and Harrell, join the Navy through the Armed Forces Health Professions Scholarship program (HPSP).
HPSP will pay tuition and fees for up to four years of school and provide a monthly stipend (currently set at $2,728 a month) to those attending school to be a physician, dentist, optometrist, physician associate or clinical psychologist. The value of the program can easily exceed $300,000 over the four years of medical school.
Scholarship recipients typically incur an Active-Duty Obligation of one year for each year in the program.
"I went to medical school in the civilian sector with an HPSP scholarship and then went on active duty, and completed my internship and residency at Naval Medical Center San Diego. Then I went to Walter Reed for about five years before going back to San Diego for a three-year fellowship in cardiovascular disease," says Harrell, who is currently the program director for the Cardiology Fellowship Program at Walter Reed National Military Medical Center in Washington, DC.
Typically, there are nine cardiology fellows training at the Naval Medical Center and another handful at Walter Reed where the cardiology fellowship program is combined with the Army. Advanced fellowships are completed at civilian programs.
Not Your Standard CV Career
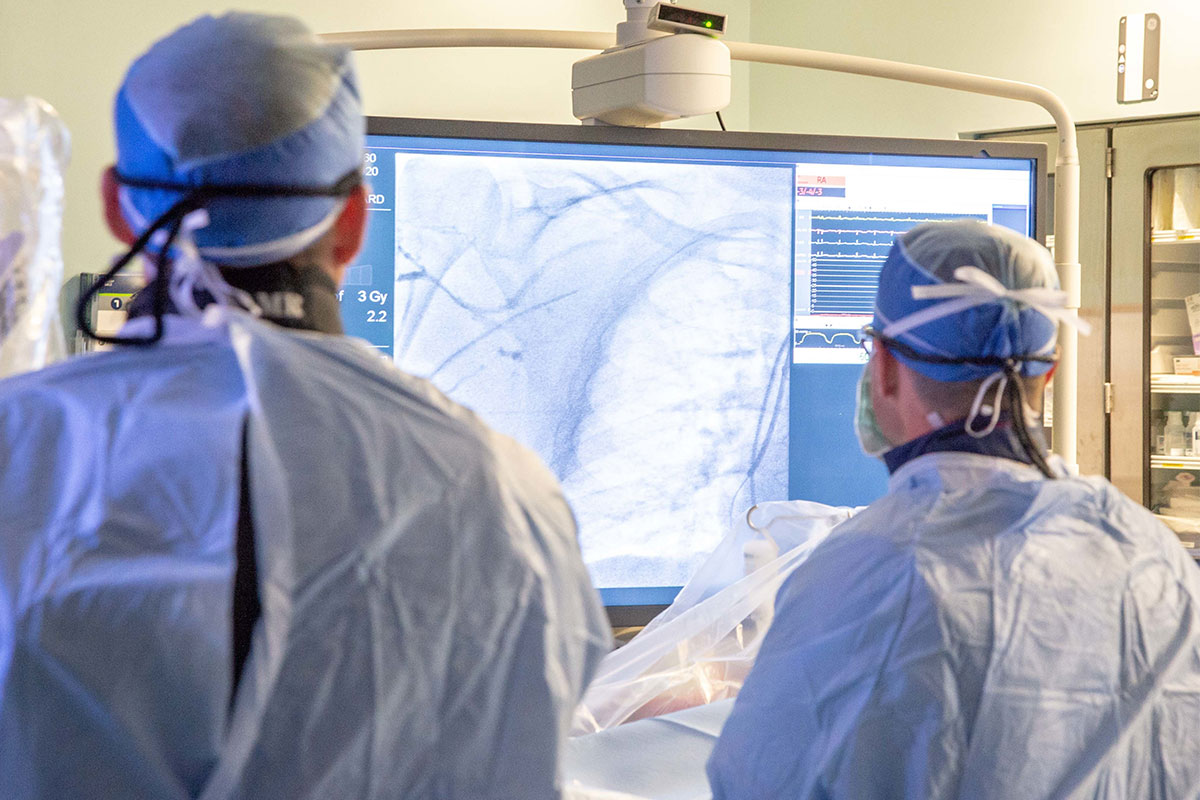 Department of Defense
Department of Defense
"Because we tend to transfer with some regularity, we have unique opportunities to serve and to take on new leadership roles as opposed to being in one place for years on end," says Wessman, who has served as an undersea medical officer, fellowship program director and department head over the course of his 21-year career. He is currently the specialty leader for Navy cardiology, essentially the Navy's top cardiologist.
"Each specialty in the Navy, both medical and surgical, has specialty leaders. We are the first point of contact for any cardiology-related questions from other specialty leaders or from the Bureau of Medicine or the Surgeon General. We help filter information up the chain of command," says Wessman. Specialty leaders also handle questions about someone's fitness for duty due to a cardiology issue, as well as represent their cardiology community to gain favorable decisions such as for allocation of resources.
Franzos, who started his Navy career as a pilot flying submarine hunting missions, has also served as a flight surgeon, chief medical officer at the Pentagon's multispecialty clinic and chief of medicine at Walter Reed.
To clarify, a flight surgeon isn't someone who performs surgery on airplanes, notes Franzos; rather, they serve as the medical providers for pilots and aviation personnel in both the Navy and the Marine Corps. So they can understand the pressures of aviation, Naval flight surgeons complete flight training up to a solo flight. However, most flight surgeons are not Navy pilots like Franzos.
Similarly, an undersea medical officer is a physician trained in the unique physiological stresses of hyperbaric and hypobaric environments, exposure to low-level ionizing radiation, atmospheric control issues, and long periods in isolated environments.
In addition to the diverse array of responsibilities, a military medical career offers subject matter specialists with unique opportunities to make lasting contributions.
For instance, Commander Harrell played a significant role in co-authoring the 2014 and 2020 Veterans Administration/Department of Defense (VA/DoD) Clinical Practice Guideline for the Diagnosis and Management of Hypertension in the Primary Care Setting.
"VA/DoD guidelines are based on an independent systematic view of the evidence for a set of key questions and may be similar or quite different from other guidelines based on the systematic review and the use of GRADE criteria to develop the recommendations," says Harrell. One of the major differences in the hypertension guidelines is the target BP of <130/90 mm Hg for VA/DoD vs. <130/80 mmHg for the AHA/ACC.
For his part, Franzos has left his mark on military medicine in several ways, including contributing to guidelines that have improved and codified the use of medical evaluations for accession, retention and disability, along with guidance on post-COVID return to deployability.
– Commander Travis Harrell, MD, FACC
Before he retired from the Navy, after 30 years of service, Franzos served at the U.S. Navy Bureau of Medicine and Surgery as the deputy chief operations officer and director of force medical readiness. One of the issues he investigated was a series of sudden deaths among sailors and marines for which no obvious cause was apparent.
"As we began to peel back the onion, we found there were multiple circumstances of ECAST, or exertional collapse associated with sickle cell trait, across the Navy, as well as in the Marine Corps and the Air Force. The Army at the time wasn't testing for sickle cell trait, so we didn't know for sure what was happening in their population," relates Franzos.
Franzos and colleagues found a reliable pattern behind ECAST that differs from what's seen with exertional heat stroke or a cardiac collapse: "people would run, they would collapse, they would get up and keep running, collapse again, keep running and really push themselves," he says. "That exertional collapse, where they remained conscious, really differentiated them from sudden cardiac arrest where it's an immediate unconscious collapse.
Most importantly, Franzos and colleagues developed relatively straightforward ways to identify and flag service members with sickle cell trait and an initial management algorithm for ECAST, which are now standard across the military. To his knowledge, there haven't been any further sickle–cell trait-related deaths.
Aging Warriors
"Military life for people in their 40s and 50s can be stressful and take its toll on health behaviors, probably not dissimilar to top-level executives and leaders in the civilian sector," says Harrell. "When you're on a ship for several months with thousands of other sailors or in a submarine that may not surface for weeks at a time, it's difficult to keep up with your health habits."
To better understand the impact of Navy life on cardiovascular risk, Harrell and colleagues initiated the Aging Warrior Study. The study, which is ongoing and plans to enroll up to 1,000 patients, is using cardiac CTA and coronary artery calcium (CAC) scoring to provide a detailed assessment of atherosclerotic burden among sailors and marines.
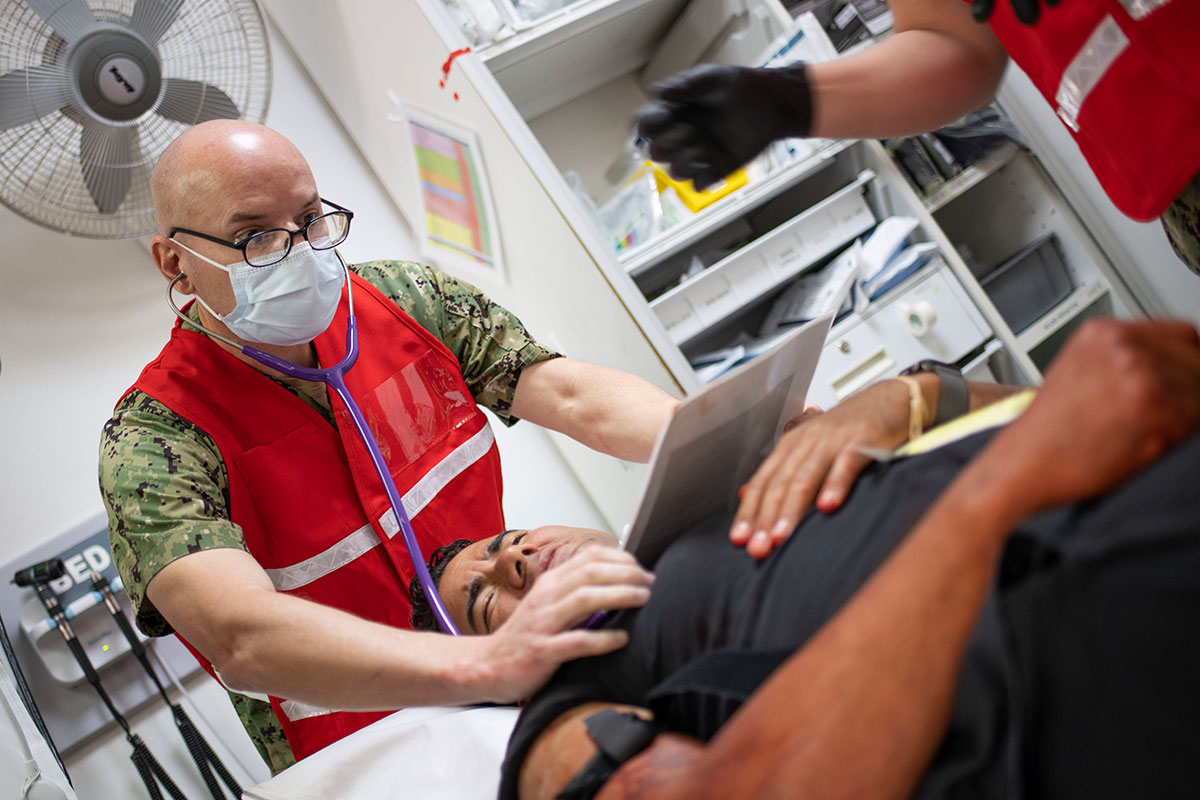 Department of Defense
Department of Defense
Eligible participants include asymptomatic, active-duty service members meeting these criteria: males >40 and females >50 years with at least one traditional risk factor, and males >50 and females >55 years regardless of risk factors.
"We want to understand the rate of atherosclerosis in this population because, for example, if a ship captain or technical expert has a coronary event in the field, we may not be able to medevac them. Plus there's a change in readiness and capability and that can quickly become a mission-critical problem," says Harrell.
Initial findings on 100 patients (median age, 47 years) presented at ACC.21, showed the median 10-year risk for atherosclerotic cardiovascular disease (ASCVD) was 4.6%. The median CAC score was 0, but coronary atherosclerosis was detected in 50% of participants and in 13% of participants with a CAC score of 0.
Vulnerable- or high-risk plaques were observed in 13% of participants. Of the patients with atherosclerosis, 92% had calcified lesions, 52% had single-vessel disease and 48% had involvement of two or more vessels.
"Our initial findings showed that half of study participants, who were all asymptomatic and otherwise in good health, had detectable coronary atherosclerosis, a higher than expected prevalence in this population and not what we expected to see given their ASCVD and Framingham risk scores," says Harrell.
"When I showed the scans to some study participants, they described years of active duty with multiple deployments," and in between serving in senior staff positions with long hours and the stress of accountability for managing the organization. "After many years of this, it's not uncommon to have some poor lifestyle habits," he adds.
Guideline-directed medical therapy has been initiated in appropriate study participants who will be followed for several years to determine if identification of coronary disease can lead to improved outcomes.
"We want to see if we can have a downstream impact on the health of the Navy, in particular, but other services as well, to make the force healthier because when our senior people have a problem it becomes an organizational problem," says Harrell.
The intricacies of military cardiology and its impact on the health of service members highlights the crucial role of military cardiologists. Their ongoing research, skills and dedication not only improve individual lives but also bolsters the strength and readiness of our armed forces.
This article was authored by Debra L. Beck, MSc.
Clinical Topics: Prevention
Keywords: ACC Publications, Cardiology Magazine, Military Personnel, Fellowships and Scholarships, Cardiovascular Diseases, Secondary Prevention
< Back to Listings

