Peripheral Matters | IVUS in Peripheral Endovascular Interventions: A Multidisciplinary Take on Consensus
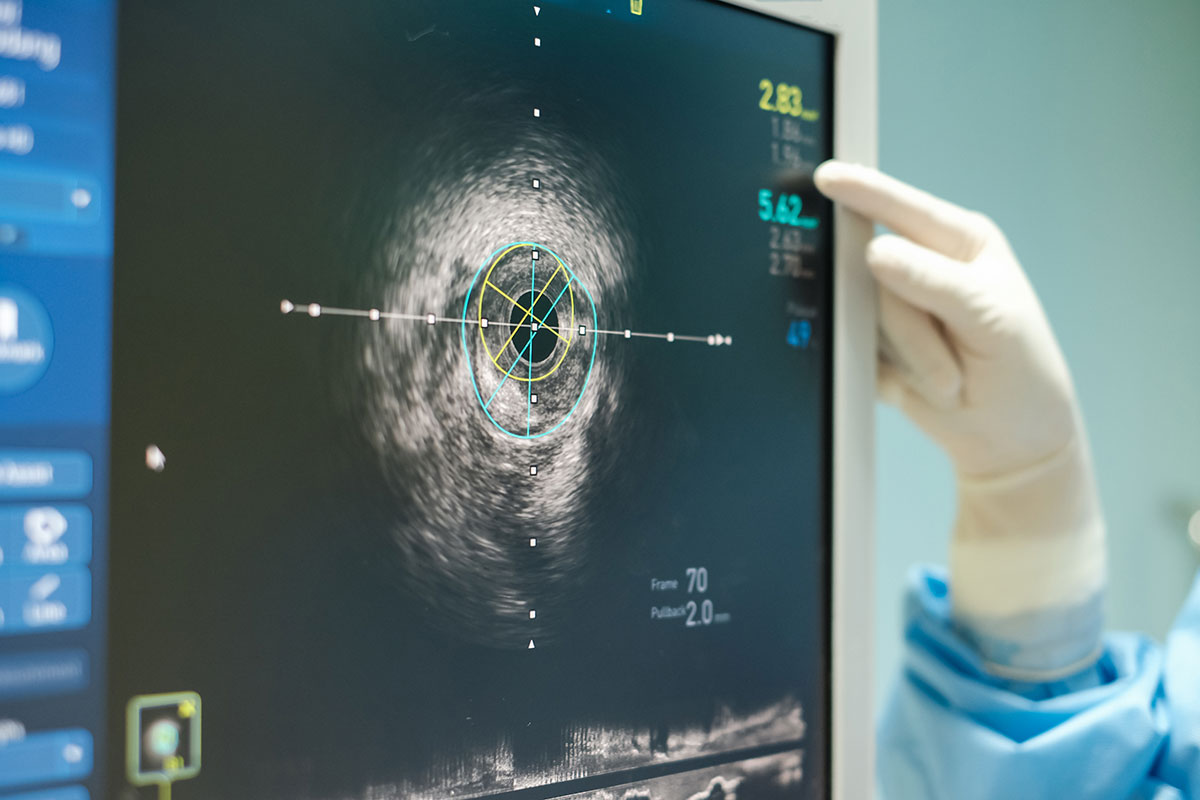
The case for intravascular ultrasound (IVUS) use in peripheral endovascular arterial and venous interventions is building. Observational and randomized data involving PCI have demonstrated that IVUS improves procedural and clinical outcomes, including reduction in major adverse cardiovascular events and even mortality.1-5
IVUS for peripheral endovascular interventions has seen rapid growth due to similar related benefits as seen with PCI. The evidence for using IVUS in this sphere and the enthusiasm to apply this technology continues to grow.
Achieving Multi-Societal Consensus
A recent multidisciplinary consensus involving six major U.S. vascular societies led by the Society for Cardiovascular Angiography & Interventions highlights several important challenges that will need to be addressed as the use of IVUS for peripheral endovascular interventions expands. These include the need for more prospective data, addressing data gaps, understanding implementation barriers, standardization, and defining appropriate use, as well as the need to understand cost effectiveness to align incentives and reimbursement.6
Furthermore, improving current IVUS catheters to facilitate easier imaging interpretation may allow for greater adoption among novice users.
Increasing Foundational Evidence Supporting Peripheral IVUS
Observational and randomized data for IVUS in peripheral arterial interventions to date have been promising. In a retrospective analysis of Medicare beneficiaries undergoing peripheral arterial interventions from 2016 to 2019, IVUS use was associated with a reduction in major adverse limb events (95% CI, 0.70-0.75; p<0.0001), as well as all endpoint components including acute limb ischemia (adjusted hazard ratio [HR], 0.82; 95% CI, 0.78-0.87; p<0.0001) and major amputation (adjusted HR, 0.69; 95% CI, 0.66-0.71; p<0.0001).7
This has also been demonstrated in an analysis of a non-U.S. administrative database, using data in Japan from 85,649 patients undergoing peripheral endovascular interventions from 2014 to 2019, of whom 50,925 patients underwent IVUS-guided procedures. A propensity-matched analysis of this cohort found the IVUS group had a lower incidence of amputation at 12 months compared with the non-IVUS group (6.9% vs. 9.3%; HR, 0.80; 95% CI, 0.72-0.89).8
Emerging randomized data suggest benefit, including a single-center prospective trial of 150 patients undergoing femoropopliteal interventions with or without IVUS guidance, which showed higher rates of freedom from binary restenosis (72.4% vs. 55.4%; p=0.008) with IVUS.9
Though they did not demonstrate a difference in clinically driven target vessel revascularization (84.2% vs. 82.4%; p=0.776), this trial was not powered for clinical end points. A subsequent randomized trial of 237 patients from seven sites in Korea found greater improvement in post procedure ankle-brachial indices (0.99 vs. 0.93; p=0.001) among the 119 patients who had IVUS plus angiography compared with the 118 patients who had angiography alone. Improved primary patency at one year was also found (83.8% vs. 70.1%; HR, 0.46; 95% CI, 0.25-0.85; log-rank p=0.01).10
Similar improvement in delineation of venous pathology and optimization of procedural elements have been noted in deep vein and iliocaval interventions. Compared with venography alone, IVUS is more sensitive at detecting venous pathology as noted in an observational study of 152 patients, in which IVUS detected stenoses in cases that venography missed (51% of limbs; p<0.0001) as well as identified more appropriate landing zones.11
While randomized comparative data for IVUS vs. venography alone in venous interventions are scarce, in a single center observational study IVUS was associated with larger venous stent sizes and was associated with fewer reinterventions at early and mid-term follow-up.12
This was replicated in a retrospective analysis of venous stent placements among Medicare beneficiaries from 2017 to 2019, which found that IVUS use was associated with reduced reintervention, hospitalization and stent migration at one year.7

Filling in the Gaps
Several key data gaps in implementing IVUS have been highlighted by Secemsky, et al., in the consensus document.6 For peripheral arterial interventions, notable gaps include lack of data and consensus on the meaning of appropriate IVUS-guided sizing. The authors also note that while post-interventional dissections are more apparent with IVUS, there is not yet consensus on which procedural dissections require active management vs. a conservative approach.
Similarly, for treatment of nonthrombotic iliac vein lesions for venous obstruction, there is a lack of consensus on what degree of stenosis is clinically actionable. While the diameter stenosis was associated with improvement in clinical symptoms in the Vein Obstruction (VIDIO) trial, a threshold for clinical response has not been established and may be patient specific.13 Furthermore, in low pressure venous systems, IVUS-generated luminal dimensions may be dynamic, subject to loading conditions and factors such as respiration.
The real-world application of IVUS shows a high degree of variability in use that is not fully explained by patient or case related factors. In a Centers for Medicare and Medicaid Services (CMS) analysis of IVUS in lower extremity arterial interventions, variation was apparent when stratified by physician specialty, with interventional radiologists being the highest users (30% of procedures) compared with cardiologists, surgeons and other specialties (15-17%).14
Notably, a separate analysis of Medicare beneficiaries undergoing femoropopliteal peripheral vascular intervention replicated these findings, adding that high-volume operators were also more likely to use IVUS (tertile 3 vs. tertile 1: odds ratio, 3.78, [2.43-5.90]).15
Despite overall higher uptake of IVUS in iliofemoral venous interventions, there is variable application for this indication as well. For venous interventions, cardiologists were the highest users (89%), followed by surgeons (77%) and interventional radiologists (41%).7
In both arterial and venous interventions, IVUS use was higher in ambulatory settings compared with inpatient settings.7,14 This may be driven by a number of factors, highlight Secemsky, et al., including a lack of flexibility in inpatient reimbursement systems such as diagnosis-related group that may limit the ability to incorporate novel technologies as they limit expenditure.6
Tackling Costs
While it is true that incorporation of any novel technology, including IVUS, increases upfront expenditure, the additive value of improved patient experience, outcomes and long-term cost-effectiveness need to be carefully considered. The authors of the multi-societal expert opinion emphasize that cost-effectiveness studies to date have not indicated that IVUS use in peripheral arterial interventions has substantially increased costs, citing an analysis of inpatient peripheral arterial interventions from 2006 to 2011, which found a nonsignificant increase in cost of $1,334 (95% CI, −$167 to $2,833; p=0.082) per hospitalization.
In a study of a Japanese claims database between April 2009 and July 2019 of 3,956 patients treated with IVUS plus angiography and 5,889 patients treated with angiography alone, IVUS was associated with a reduction in subsequent revascularization procedures (adjusted HR, 0.25, [0.22-0.28]) and major adverse cardiovascular events (HR, 0.69, [0.65-0.73]).17
This resulted in a mean cost savings per patient of $18,173 [$7,695-$28,595] over the total follow-up period. Further, the upfront cost of IVUS in this study was attenuated to a level no different than angiography alone after one year of follow-up.
A cost-effectiveness analysis of a German health care payer perspective for a willingness to pay €50,000 per incremental quality-adjusted life-year gained with IVUS use was 85.9% over a lifetime.16-18
However, it should be emphasized that despite the plausible long-term benefit on health care costs, the immediate financial impact on individual providers, practices and health systems is likely a barrier and needs to be addressed by both partnering with industry to decrease costs and advocating for payers to improve reimbursement to support future reduced costs.
It is also imperative to consider nonquantifiable value such as decreased radiation exposure to both providers and patients. Moreover, educating operators on appropriate image acquisition and interpretation can minimize inefficiencies such as procedural delays and optimal results can increase the value of health care spending.
Appropriate Use
Other barriers to implementation of IVUS for peripheral endovascular interventions include the relative lack of societal guidance to date on appropriate indications for use. The publication of an expert consensus document in 2022 represented the first effort to characterize appropriate use. The document was generated by structured surveys of 15 experts for arterial and venous interventions.19
The experts then graded the use of IVUS for various interventional scenarios on an appropriateness scale. A contemporary systematic review of the evidence for IVUS in peripheral arterial and venous interventions found that the evidence base for IVUS in peripheral arterial and venous interventions in this study is largely comprised of observational and retrospective studies which have favorable associations for IVUS in the pre-interventional, intra-procedural and post-procedural phases.20
Incorporation of IVUS into peripheral endovascular guidelines remains the next step in providing a framework to harmonize practice more broadly and is reliant on continued generation of high-quality prospective data.
Future Device Innovation
In addition to increasing the prospective evidence to support peripheral IVUS utilization and creating more dedicated training pathways, innovation in peripheral IVUS technology remains an important next step. Many of the legacy IVUS catheters were originally designed for coronary use and have been available for >10 years without significant upgrades.
As such, there remains an opportunity to improve catheter performance and navigation, enhance image quality and improve workflow processes to keep procedural times unaffected. Furthermore, future development of artificial intelligence capabilities can assist with imaging interpretation and help guide new and experienced users to approach peripheral interventions in a standardized fashion.


This article as authored by Ramya C. Mosarla, MD, interventional cardiology fellow at NYU Langone in New York, and research fellow at the Richard A. and Susan F. Smith Center for Outcomes Research in Cardiology at Beth Israel Deaconess Medical Center (BIDMC) in Boston, MA, and Eric A. Secemsky, MD, RPVI, MSc, FACC, director of Vascular Intervention at BIDMC and section head of Interventional Cardiology and Vascular Research at the Richard A. and Susan F. Smith Center for Outcomes Research in Cardiology at BIDMC, and associate professor of medicine at Harvard Medical School.
References
- Hong SJ, Kim BK, Shin DH, et al. Effect of intravascular ultrasound-guided vs angiography-guided everolimus-eluting stent implantation: The IVUS-XPL randomized clinical trial. JAMA 2015;314:2155-63.
- Zhang J, Gao X, Kan J, et al. Intravascular ultrasound versus angiography-guided drug-eluting stent implantation: The ULTIMATE Ttrial. J Am Coll Cardiol 2018;72:3126-37.
- de la Torre Hernandez JM, Baz Alonso JA, Gómez Hospital JA, et al. Clinical impact of intravascular ultrasound guidance in drug-eluting stent implantation for unprotected left main coronary disease: pooled analysis at the patient-level of 4 registries. JACC Cardiovasc Interv 2014;7:244-54.
- Kim BK, Shin DH, Hong MK, et al. Clinical impact of intravascular ultrasound-guided chronic total occlusion intervention with zotarolimus-eluting versus biolimus-eluting stent implantation: Randomized study. Circ Cardiovasc Interv 2015;8:e002592.
- Lawton JS, Tamis-Holland JE, Bangalore S, et al. 2021 ACC/AHA/SCAI guideline for coronary artery revascularization. J Am Coll Cardiol 2022;79:e21-e129.
- Secemsky EA, Aronow HD, Kwolek CJ, et al. Intravascular ultrasound use in peripheral arterial and deep venous interventions: Multidisciplinary expert opinion from SCAI/AVF/AVLS/SIR/SVM/SVS. J Vasc Interv Radiol 2024;35:335-48.
- Divakaran S, Meissner MH, Kohi MP, et al. Utilization of and outcomes associated with intravascular ultrasound during deep venous stent placement among medicare beneficiaries. J Vasc Interv Radiol 2022;33:1476-84.e2.
- Setogawa N, Ohbe H, Matsui H, Yasunaga H. Amputation after endovascular therapy with and without intravascular ultrasound guidance: A nationwide propensity score-matched study. Circ Cardiovasc Interv 2023;16:e012451.
- Allan RB, Puckridge PJ, Spark JI, Delaney CL. The impact of intravascular ultrasound on femoropopliteal artery endovascular interventions: A randomized controlled trial. JACC Cardiovasc Interv 2022;15:536-46.
- Ko Y-G. Comparison of IVUS-guided vs. angiography-guided angioplasty for the outcomes of drug-coated balloon in the treatment of femoropopliteal artery disease: IVUS-DCB. Presented at ACC.24.
- Montminy ML, Thomasson JD, Tanaka GJ, et al. A comparison between intravascular ultrasound and venography in identifying key parameters essential for iliac vein stenting. J Vasc Surg Venous Lymphat Disord 2019;7:801-7.
- Tran LM, Go C, Zaghloul M, et al. Intravascular ultrasound evaluation during iliofemoral venous stenting is associated with improved midterm patency outcomes. J Vasc Surg Venous Lymphat Disord 2022;10:1294-1303.
- Gagne PJ, Gasparis A, Black S, et al. Analysis of threshold stenosis by multiplanar venogram and intravascular ultrasound examination for predicting clinical improvement after iliofemoral vein stenting in the VIDIO trial. J Vasc Surg Venous Lymphat Disord 2018;6:48-56.e1.
- Divakaran S, Parikh SA, Hawkins BM, et al. Temporal Trends, practice variation, and associated outcomes with IVUS use during peripheral arterial intervention. JACC: Cardiovasc Interv 2022;15:2080-90.
- Deery SE, Goldsborough E, Dun C, et al. Use of Intravascular ultrasound during first-time femoropopliteal peripheral vascular interventions among medicare beneficiaries. Ann Vasc Surg 2022;80:70-7.
- Panaich SS, Arora S, Patel N, et al. Intravascular ultrasound in lower extremity peripheral vascular interventions: Variation in utilization and impact on in-hospital outcomes from the nationwide inpatient sample (2006-2011). J Endovasc Ther 2016;23:65-75.
- Soga Y, Ariyaratne TV, Secemsky E, et al. Intravascular ultrasound guidance during peripheral vascular interventions: Long-term clinical outcomes and costs from the Japanese perspective. J Endovasc Ther 2023:15266028231182382.
- Lichtenberg M, Mustapha J, Tan YZ, et al. Cost-effectiveness analysis of intravascular ultrasound-guided peripheral vascular interventions in patients with femoropopliteal peripheral artery disease. Vasa 2024;53:135-44.
- Secemsky EA, Mosarla RC, Rosenfield K, et al. Appropriate use of intravascular ultrasound during arterial and venous lower extremity interventions. JACC Cardiovasc Interv 2022;15:1558-68.
- Natesan S, Mosarla RC, Parikh SA, et al. Intravascular ultrasound in peripheral venous and arterial interventions: A contemporary systematic review and grading of the quality of evidence. Vasc Med 2022;27:392-400.
Clinical Topics: Invasive Cardiovascular Angiography and Intervention, Noninvasive Imaging, Interventions and Imaging, Angiography, Echocardiography/Ultrasound, Nuclear Imaging
Keywords: Cardiology Magazine, ACC Publications, Ultrasonography, Interventional, Cost-Benefit Analysis, Percutaneous Coronary Intervention, Angiography
