For the FITs | Critical Care Cardiology Training 101: Considerations For General Cardiology Fellowship and Beyond

The patient population cared for in the modern cardiovascular intensive care unit (CICU) has changed dramatically over the past few decades. Gone are the days when the CICU was primarily a coronary care unit (CCU). With acute coronary syndromes accounting for <10% of current admissions, heart failure and cardiogenic shock are now the bread and butter of the modern CICU.1,2,3
Moreover, according to data from the Cardiology Critical Care Trials Network, the most common current indication for admission to a CICU is respiratory failure, followed by shock (21%).4 Cardiologists practicing in contemporary CICUs must not only have a broad cardiac knowledge base, but also expertise in the management of noncardiac ailments, from sepsis to renal failure.3,5 Enter the evolving field of critical care cardiology (CCC).
The Landscape of CICU Staffing
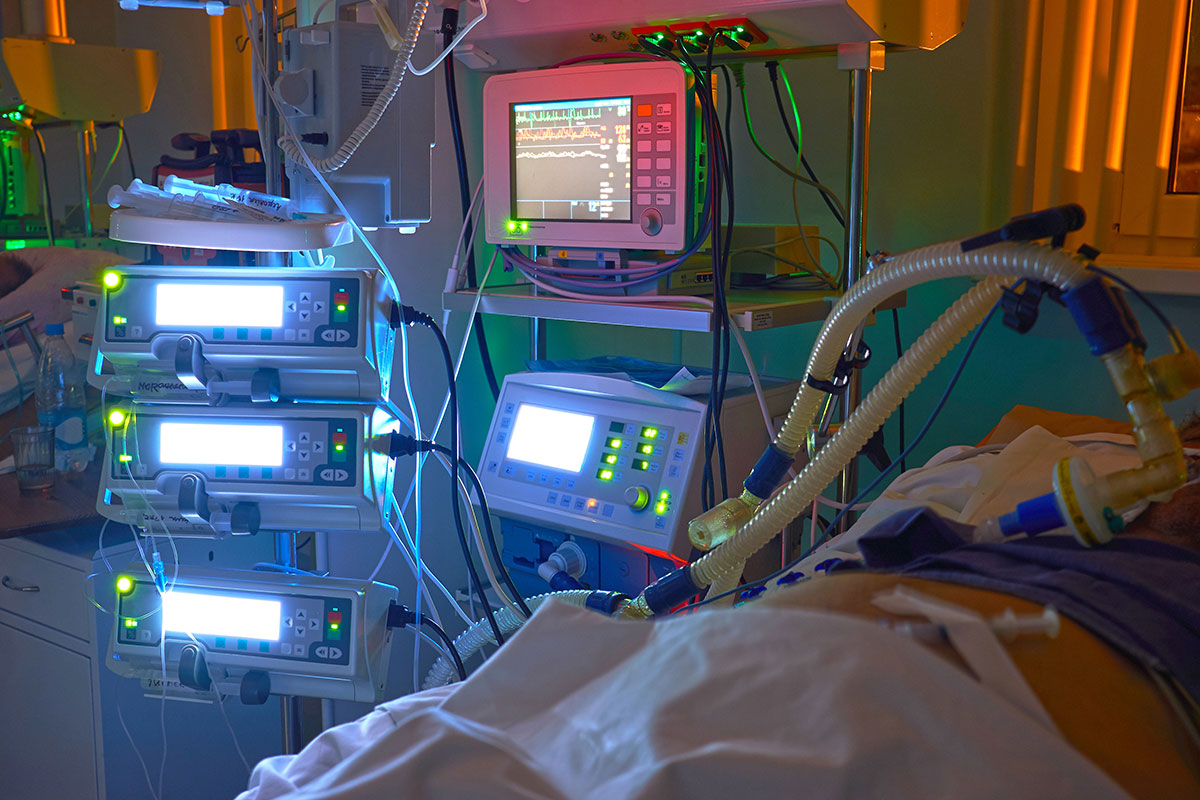
Though interest in CCC is on the rise, the actual number of trainees who have completed both cardiology and critical care medicine (CCM) lags far behind what would be necessary to staff all CICUs with cardiac intensivists alone. However, with the growing complexity of CICU patients and data suggesting that ICU patient outcomes improve with intensivist staffing, there is a general recognition that a transformation in CICU staffing is warranted.2,3,6-9
While some hospitals have moved towards utilizing general intensivists to staff the CICU, there is minimal exposure to cardiovascular critical care during general CCM fellowship.10 In the absence of a dual-trained cardiac intensivist, CICUs employ a variety of models to adequately care for patients with cardiac and noncardiac critical illnesses. This ranges from cardiologist staffing with an ICU consult on select patients to formal co-staffing by cardiologists and intensivists.
While Leapfrog standards do not currently mandate intensivist involvement for all critically ill patients, it is anticipated that this may change.3,11,12 One of the largest barriers to increasing the availability of cardiac intensivists lies in the lack of integrated cardiovascular critical care training pathways.13,14
Statements have been published by the ACC, American Heart Association (AHA) and the European Society of Cardiology that not only recommend incorporation of critical care training in general cardiology fellowship curricula, but also a rise in formal CCM-trained cardiologists.2,6,9,15,16 The following are considerations for those interested in pursuing dual training in cardiology and critical care.
Should I Pursue Dual-Training in Cardiology and Critical Care?
Ultimately, it is most important to determine what you are looking for in your career. If you're planning on working mostly in CICUs (especially at academic or tertiary care centers), leading a CICU, working in multiple types of ICUs (cardiothoracic [CTICU], medical [MICU], etc.) or conducting CCC-based research, it is wise to pursue an additional year of CCM training.
In addition, while it is currently not a requirement to have formal intensivist training to staff a CICU of any kind, nor be an intensivist to bill for critical care, it is likely that staffing models will undergo major changes over the next decade or two. Thus, if your primary career goal is to work in a CICU, it is worthwhile to complete a CCM fellowship.
What Training Pathways Are Available For Dual-Boards?
Unlike pulmonary critical care (PCC), there are currently no specific combined programs for CCC that trainees can apply to straight out of residency. Instead, one must separately complete cardiology and CCM training. There are multiple ways to achieve this, which can cause confusion for CCC-bound trainees.
From internal medicine-based training, there are two paths to be eligible to sit for CCM boards outside of a PCC fellowship: 1) a two-year ACGME standalone CCM fellowship that can be completed without additional fellowship training, or 2) a one-year CCM fellowship after an internal medicine subspecialty fellowship (such as cardiology). All CCM programs require a minimum of 12 months of clinical training, six months of which must be in ICUs.
Most programs have more than six months of critical care time, and two-year programs do allow for more elective and research time. For the two-year option, a fellow can choose to do their critical care training before or after cardiology, each of which has its own pros and cons, as outlined by Miller, et al.13
While the ACGME website has a list of accredited two-year CCM fellowships, a list of one-year fellowship programs is not readily available. Most CCC-bound trainees utilizing the one-year pathway choose to do so at their home institution. If a program does not have a CCM fellowship outside of PCC, a trainee can work with the PCC leadership to try to arrange a specific track to fit their needs, which can be submitted to the ACGME for approval (this discussion would also need to include consideration of funding for the year).11
Regardless of whether you participate in a formal two-year CCM fellowship, a preexisting one-year CCM fellowship after general cardiology training or a self-arranged one-year fellowship, it is prudent to speak with program leadership to determine whether your year can be tailored towards your career goals.
For example, if you wish to work in both a CTICU and CCU, it can be important to ask the CCM program director about the ability to prioritize additional CTICU time. It would also be important to inquire about the case mix of cardiac surgeries performed at the program to ensure adequate broad exposure.
Similarly, if you are interested in mechanical support and your general training did not have opportunities to directly care for patients with balloon pumps, Impellas and extracorporeal membrane oxygenation (ECMO), you may want to ensure your program has more of this time built into a critical care year.
Evaluating General Cardiology Programs
Get Involved!
Click here to learn more about and join the ACC Critical Care Cardiology Member Section.
For those interested in CCC, a common question is what to look for in a general cardiology program. It's important to remember that a large part of CCC is actually cardiology! Though you will learn advanced airway management, sepsis treatment and renal replacement therapies during a formal critical care year, the cardiology portion of CCC must be acquired during general fellowship. Thus, when applying to general cardiology programs, it is important to ensure you will have access to sufficiently broad training that is best in line with your career goals. Here's a set of questions to ask program directors and fellows where you interview to help assess each program.
What is the fellow's role in the CCU?
Is the unit open or closed? What types of decisions do fellows make autonomously vs. ask for attending input? Do fellows work with residents and/or advanced practice providers?
What types of patients are treated in the CICU?
Are patients on mechanical support cared for in the CCU or CTICU? Will there be exposure to intra-aortic balloon pumps, Impellas, durable left ventricular assist devices (LVADs) and ECMO? If these are handled in the CTICU, is there an opportunity to rotate through the CTICU or co-manage them on heart failure rotations? Is there a transplant/VAD program? Are patients with pulmonary hypertension managed in the CICU or MICU? How much exposure is there to right heart failure?
Does the program have a pre-designed training pathway for CCC?
If so, what is the process for applying to this track? Is it possible to speak with the CCM fellowship director to talk more about the program and application pathway? If there is no formal CCC pathway, have previous fellows been able to arrange an ACGME-accredited CCM year and would your general cardiology program support this?
Are there attendings in the CICU who are dual trained in cardiology and critical care?
If possible, being able to learn from dual trained mentors and seek their guidance can enhance your training experience.
What procedures do general fellows perform in the CICU?
Are pulmonary artery lines commonly used? Are they placed at the bedside by general fellows? Are dialysis lines, transvenous pacing and/or IABPs placed by general fellows?
How much hands-on time with pacemaker interrogation and programming do general fellows get?
Do general fellows learn how to turn tachycardia therapies on and off? Are there any opportunities to gain experience with anti-tachycardia pacing? These skills can be invaluable for the CICU attending as these situations are often emergent and an electrophysiologist may not be in house!
If desired, can I feasibly reach Level II echocardiography training during general fellowship?
Though it may not be necessary to obtain formal Level II training (ability to read and bill transthoracic echocardiography [TTE] reads), it is very important to be facile with bedside TTE. The ability to obtain Level II training during general fellowship is a good proxy for how much hands-on experience you will get with an echo probe! Do general fellows or imaging fellows perform transesophageal (TEEs)? TEEs are also a large part of CTICU management, so it is beneficial to get this experience, but not necessary.
What is the role of the general fellow in the cath lab?
During cath lab rotations, ask what is the breakdown of femoral vs. radial access. While undoubtedly it is possible to gain proficiency in femoral access outside the cath lab setting, it is favorable to be able to learn femoral access in non-urgent situations from the experts in vascular access! Other questions to ask: Will I be able to participate in balloon pump and/or Impella insertions? What about pericardiocenteses?
Is there any flexibility in tailoring the CCM year towards critical care cardiology?
This question is best when it's possible to speak with the critical care medicine fellowship director or previous CCC trainees. Also ask whether it's possible to spend more time in the CTICU or cardiac ORs learning about bypass and honing TEE skills? What elective time is built into the program?

This article was authored by Allison Levin, MD, MSc, a second-year cardiology fellow at Duke University. She earned her Bachelor of Arts in neuroscience from Columbia University, where she earned a MSc in biostatistics and her medical degree. Levin completed her internship at the University of Pennsylvania and her residency at Massachusetts General Hospital in Boston.
Do you have an idea for an article for this section? Want to write an article? Reach out to Levin on Twitter @Dr_ALevin or email cardiologyeditor@acc.org.
References
- Watson RA, Bohula EA, Gilliland TC, et al. Prospective registry of cardiac critical illness in a modern tertiary care cardiac intensive care unit. Eur Heart J Acute Cardiovasc Care 2019;8:755-61.
- Morrow DA, Fang JC, Fintel DJ, et al. Evolution of critical care cardiology: Transformation of the cardiovascular intensive care unit and the emerging need for new medical staffing and training models. Circulation 2012;126:1408-28.
- Katz JN, Minder M, Olenchock B, et al. The genesis, maturation, and future of critical care cardiology. J Am Coll Cardiol 2016;68:67-79.
- Bohula EA, Katz JN, van Diepen S, et al. Demographics, care patterns, and outcomes of patients admitted to cardiac intensive care units: The Critical Care Cardiology Trials Network prospective North American multicenter registry of cardiac critical illness. JAMA Cardiol 2019;4:928-35.
- Sinha SS, Sjoding MW, Sukul D, et al. Changes in primary noncardiac diagnoses over time among elderly cardiac intensive care unit patients in the United States. Circ Cardiovasc Qual Outcomes 2017;10:e003616.
- van Diepen S, Fordyce CB, Wegermann ZK, et al. Organizational structure, staffing, resources, and educational initiatives in cardiac intensive care units in the United States. Circ Cardiovasc Qual Outcomes 2017;10:e003864.
- Pronovost, PJ, Angus DC, Dorman T, et al. Physician staffing patterns and clinical outcomes in critically ill patients: A systematic review. JAMA 2002;288:2151-62.
- Levy MM, Rapoport J, Lemeshow S, et al. Association between critical care physician management and patient mortality in the intensive care unit. Ann Intern Med 2008;148:801-9.
- O'Malley RG, Olenchock B, Bohula-May E, et al. Organization and staffing practices in US cardiac intensive care units: a survey on behalf of the American Heart Association Writing Group on the Evolution of Critical Care Cardiology. Eur Heart J Acute Cardiovasc Care 2013;2:3-8.
- Hill T, Means G, van Diepen S, et al. Cardiovascular critical care: A perceived deficiency among U.S. trainees. Crit Care Med 2015;43:1853-8.
- Yuriditsky E, Pradhan D, Brosnahan SB, et al. Cardiovascular critical care training: A collaboration between intensivists and cardiologists. ATS Sch 2022;3:522-34.
- Gasperino J. The Leapfrog initiative for intensive care unit physician staffing and its impact on intensive care unit performance: A narrative review. Health Policy 2011;102:223-8.
- Miller P, Kenigsberg B, Wiley B, et al. Cardiac critical care. J Am Coll Cardiol 2019;73:1726-30.
- O'Brien CG, Barnett CF, Dudzinski DM, et al. training in critical care cardiology within critical care medicine fellowship: a novel pathway. J Am Coll Cardiol 2022;79: 609-13.
- Hasin Y, Danchin N, Filippatos GS, et al. Recommendations for the structure, organization, and operation of intensive cardiac care units. Eur Heart J 2005;26:1676-82.
- O'Gara P, Adams J, Drazner M, et al. COCATS 4 Task Force 13: Training in critical care cardiology. J Am Coll Cardiol 2015;65:1877-86.
Clinical Topics: Cardiovascular Care Team
Keywords: ACC Publications, Cardiology Magazine, Fellowships and Scholarships, Cardiologists, Critical Illness, Internship and Residency, Extracorporeal Membrane Oxygenation, Intensive Care Units, Cardiology, Workforce, Knowledge Bases
< Back to Listings

