ACC.21: Late-Breaking Science Brings Practice-Changing Insights
Quick Links: Clinical Spotlight Sessions: Evidence and Perspectives to Support Best Practices • ACC.21 Explores New Research, Ongoing Challenges and Silver Linings of COVID-19 Pandemic • ACC Global Heart Attack Treatment Initiative Shows Benefits in Improving Care in Low-, Middle-Income Countries • Advancing Solutions to Diversity, Equity, Inclusion
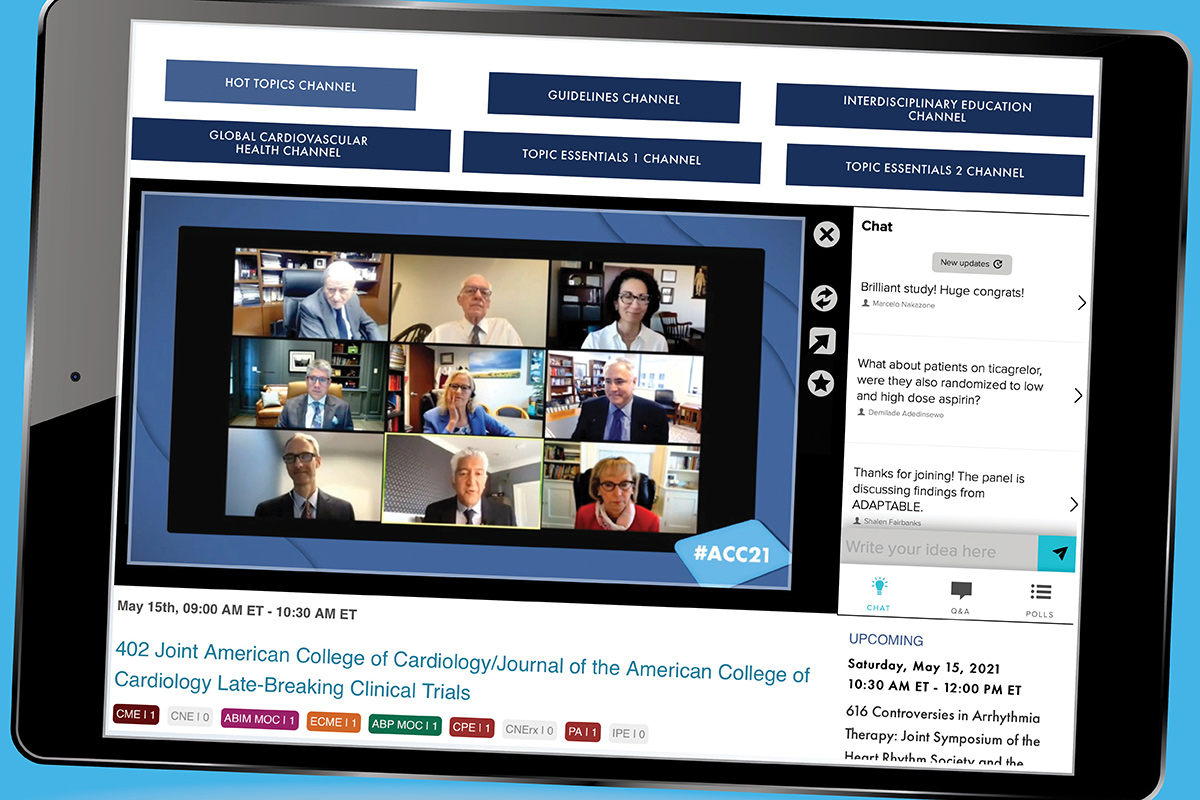
Late-Breaking Clinical Trials and Featured Clinical Research are hallmarks of every ACC Annual Scientific Session and ACC.21 was no different. Findings from the robust lineup of trials presented over the course of the three-day meeting at the very least add valuable contributions to the delivery of care across the spectrum of cardiology, while in many cases delivering practice-changing results.
The much-anticipated ADAPTABLE trial may not have delivered a clear-cut answer about the optimal dose of aspirin for secondary prevention in patients with established atherosclerotic cardiovascular disease, but it was a win for helping to usher in a new era of clinical trial design.
Over the median 26.2 months of follow-up, no significant difference was found in cardiovascular events or major bleeding between the 81 mg and 325 mg daily doses among 15,076 patients. The hazard ratio (HR) was 1.02 (95% confidence interval [CI], 0.91-1.14) for the primary effectiveness outcome of the combination of all-cause death or a hospitalization for a myocardial infarction (MI) or stroke (590 vs. 569 patients experiencing an event in the low- and high-dose groups). Results were consistent across subgroups of patients, including age, race/ethnicity, gender, prior use of dual antiplatelet therapy, or coexisting diabetes or chronic kidney disease.
The primary safety outcome of hospitalization for major bleeding occurred in 53 and 44 patients, respectively, in the low- and high-dose groups (HR, 1.18; 95% CI, 0.79-1.77). Both outcomes were time-to-event analyses.
Likely to receive much discussion in sorting through and understanding the results of ADAPTABLE will be the rate of dose switching, which was significantly higher in the high-dose group: 41.6% switched dose at least once, compared with only 7.1% in the low-dose group. This translated to fewer median days of exposure to the assigned dose (434 days vs. 650 days). Discontinuation of aspirin was 7% and 11% in the low- and high-dose groups. Also notable is that most patients (96%) were taking aspirin at baseline (85% taking 81 mg).
While the open-label study design may have been a limitation in providing a definitive answer on the optimal dose of aspirin, the study is a major achievement, because it "provides a demonstration that randomized clinical trials can leverage electronic health record data, direct-to-patient methods, and patient-reported outcomes to address important patient-centered questions," wrote W. Schuyler Jones, MD, FACC, et al., in the New England Journal of Medicine.
LAAOS III firmly sits in the practice-changing camp, showing that left atrial appendage occlusion (LAAO) performed during cardiac surgery reduced the incidence of the primary outcome of stroke and systemic embolism in patients with atrial fibrillation (AFib) and high risk of stroke (CHA₂DS₂-VASc score ≥2).
"The study confirms a new paradigm for stroke prevention for patients with [AFib]," said Richard Whitlock, MD, PhD, the study's lead author. On average, the procedure added <10 minutes to the surgery and demonstrated safety both in the short- and long-term. A standard surgical approach was used, making it unclear whether catheter-based approaches would achieve the same benefit.
The international trial randomized half of the 4,811 patients to LAAO; about two-thirds had valve surgery and 20% had CABG. All received standard anticoagulant medications after surgery.
After a median follow-up of 3.8 years, LAAO lowered the risk of stroke or systemic embolism by 33% overall in patients with AFib or atrial flutter. After the first 30 days post procedure, patients who received LAAO, vs. those who did not, were 42% less likely to suffer a stroke over long-term follow-up. Results were consistent across all subgroups analyzed, with LAAO bringing the same benefits regardless of geographic location, sex, age, type of AFib, type of blood thinner or other variables. The trial was stopped early due to the strength of the observed benefits from the procedure.
A real win for patients is the results of an analysis from the EXPLORER-HCM trial that showed health status was "markedly improved" with mavacamten in patients with symptomatic obstructive hypertrophic cardiomyopathy (HCM).
The randomized trial of 251 patients had previously reported that the once daily novel myosin inhibitor that decreases contractility compared with placebo improved physiologic endpoints (resting and stress outflow gradients) and NYHA functional class at 30 weeks.
In this analysis, the primary outcome of self-reported health status measured by the Kansas City Cardiomyopathy Questionnaire (KCCQ) overall score was greater with mavacamten vs. placebo (p<0.0001) at 30 weeks, with similar benefits across all KCCQ subscales. The proportion of patients with a very large change was 36% vs. 15% with mavacamten vs. placebo, with an estimated absolute difference of 21% and number needed to treat of five. These gains returned to baseline after treatment was stopped.
The greatest benefits were for the physical limitation scale, followed by symptoms, quality of life and social limitations. Not only will these results change the care of patients with HCM, they provide more information for shared decision-making conversations.
Heart Failure: Wins for Rehab, Omecamtiv Mecarbil, More
In the large and growing population of patients with heart failure (HF) that continues to be challenging to manage well, results from several trials provide some hope for improving quality of life as well as reduce events.
A novel 12-week cardiac rehabilitation (rehab) program tailored to address the specific physical impairments of older patients hospitalized with acute HF improved physical functioning along with quality of life and depression compared with usual care, regardless of a patient's ejection fraction (EF), in the REHAB-HF trial.
The multicenter, controlled trial randomized 349 patients to a transitional, tailored, progressive rehab intervention that addressed four physical-function domains of strength, balance, mobility and endurance (n=175) or usual care (n=174). Patients ranged in age from 60-99 years; over half were women and 49% were from underrepresented racial or ethnic minority groups. More than half of patients (53%) had HF with preserved ejection fraction (HFpEF) and nearly all had an average of five comorbidities, including hypertension, diabetes, obesity, lung disease and kidney disease. Patients in each group had markedly impaired physical function at baseline, and 97% were frail or pre-frail.
The REHAB-HF program started early – during the patient's hospital stay if possible – and transitioned to three outpatient sessions per week for 12 weeks following hospital discharge. At the three-month follow-up, compared with usual care, patients in the intervention group had notable and significant improvements in physical functioning and quality of life across all the assessments used, including the Short Physical Performance Battery, 6-minute walk test, KCCQ, and a separate depression survey.
In terms of clinical events, no statistically significant differences were seen between groups, including rates of readmission for any reason, with 194 and 213 rehospitalizations occurring in the intervention and usual care groups, respectively. HF-related hospitalizations were not different (94 vs. 110) at six months. The higher number of deaths in the rehab group (21 vs. 16) was not statistically significant.
"The study was not large enough to really look at clinical events. But patient preference surveys show that older patients often value improved function and quality of life independently of rehospitalization and death," said Dalane W. Kitzman, MD, FACC, the study's lead author. An "independently important finding" may be that "exercise also resulted in patients becoming happier – or at least less depressed," wrote Stefan D. Anker, MD, PhD, and Andrew J.S. Coats, MD, FACC, in a related editorial comment in the New England Journal of Medicine. They conclude that the results "provide a compelling argument for the adoption of exercise rehabilitation as standard care, even for elderly, frail patients with acute [HF]."
In patients with HF and reduced ejection fraction (HFrEF), patients with lower baseline EFs had a greater reduction in HF events with the novel selective cardiac myosin activator omecamtiv mecarbil in the GALACTIC-HF trial.
In the primary results, a significant interaction for the effect of the study drug on the primary outcome was seen in patients with an EF ≤28% vs. >28%. Omecamtiv mecarbil (25 mg, 37.5 mg or 50 mg twice daily) vs. placebo in addition to guideline-directed medical therapy reduced the primary composite endpoint of time to first HF event or cardiovascular death.
Across quartiles of baseline EF in this analysis (≤22%; 23-28%; 29-32%; ≥33%), as EF decreased, there was a progressively greater relative and absolute treatment effect: in the lowest quartile (n=2,246) there was a 17% relative risk reduction vs. the highest quartile (n=1,750) (HR, 0.99; interaction as EF by quartiles, p=0.013). The absolute risk reduction in the lowest quartile was 7.4 events per 100 patient-years, vs. no reduction in the highest quartile. The number needed to treat for three years was 11.8 in the lowest quartile.
Compared with placebo, with omecamtiv mecarbil there was no significant difference in systolic blood pressure (SBP), serum potassium or creatinine. In every quartile, there was a significant but similar and minimal reduction in heart rate, and troponin was increased minimally. There was a progressive decrease in NT-proBNP as EF decreased. No differences were seen in serious adverse events or in adjudicated arrhythmic and ischemic events.
An analysis of pooled, patient-level data from the SCORED and SOLOIST-WHF trials in 11,784 patients with both diabetes and HF, sotagliflozin, compared with placebo, "robustly and significantly" reduced the composite of total cardiovascular deaths, hospitalizations for HF and urgent visits for HF across the full range of EF, including HFpEF, over a median period of nine to 16 months. Data from a subgroup of 4,500 patients with a history of HF were also analyzed.
In patients with an EF ≤40%, sotagliflozin treatment reduced risk by 22% in both the entire cohort and in the HF group. For patients with an EF of 40% to 50%, sotagliflozin reduced risk in the entire cohort by 39% and in the HF group by 43%. For patients with HFpEF, the medication reduced risk by 30% in the entire cohort and by 33% in the HF group. All results were statistically significant and were similar for men and women.
We saw a significant reduction in the primary endpoint irrespective of patients' [EF] at study entry," said Deepak L. Bhatt, MD, MPH, FACC, principal investigator for the study. "The benefit for patients with HFpEF is striking – this is the first trial to find a significant benefit in this population. We believe that these results merit a recommendation that patients who have both diabetes and HFpEF should be treated with sotagliflozin or another medication in its class."
Bhatt noted that a limitation of the study is that the results apply only to patients with HF who also have diabetes. The researchers had intended to also analyze the effect of sotagliflozin in patients with HF who did not have diabetes; however, this analysis was not performed because both the SCORED and SOLOIST-WHF trials were terminated early due to loss of funding at the onset of the COVID-19 pandemic.
Turning to patients with advanced HFrEF, the LIFE study failed to show that sacubitril/valsartan was superior to valsartan for lowering NT-proBNP or improving other clinical outcomes. The multicenter randomized trial was stopped early, in March 2020, because of the high risk for adverse outcomes in this vulnerable population during the COVID-19 pandemic. The statistical plan was revised and specified 335 patients so none of the collected clinical endpoints would be impacted.
At baseline, the EF was ≤20%, SBP was about 113 mm Hg, estimated glomerular filtration rate was 63.6 mL/min/1.73m2 in the combination arm and 65.7 mL/min/1.73m2 in the valsartan arm, and NT-proBNP was 1,931 pg/ml and 1,818 pg/ml in the respective arms. Neither treatment regimen reduced the median NT-proBNP below the baseline level, and no difference was seen for secondary endpoints.
"We make the assumption that all [HF] patients are the same and therefore will respond the same to all therapies," said Douglas L. Mann, MD, FACC, the study's lead author. "However, the patient population with advanced [HF] is different from patients with less advanced [HF] because of the end organ changes that occur in the heart and kidneys. These end organ changes limit the ability of the failing heart to respond to conventional therapies to the same extent as occurs in patients with milder forms of [HF]."
PARADISE-MI was designed to tell us whether sacubitril/valsartan could reduce HF-related events compared with good old ACE inhibition when given within a week of an acute MI. Results presented at ACC.21 showed the ARNI combination treatment did not outperform ramipril. Sacubitril/valsartan did not significantly reduce the composite primary outcome of cardiovascular death, HF hospitalization or outpatient HF requiring treatment.
The international, multicenter trial randomized patients with an EF ≤40% and/or pulmonary congestion, plus one of eight additional risk-enhancing factors like AFib, prior MI, diabetes, etc., to sacubitril/valsartan (n=2,830) or ramipril (n=2,831). Most achieved the full dose of their assigned medication and continued it throughout the trial, which had a median follow-up of 23 months. None of the patients had a history of HF and most were taking antiplatelet therapy and medication to lower blood pressure and cholesterol.
The rate of the composite primary endpoint was 10% lower with sacubitril/valsartan than with ramipril, falling short of the prespecified threshold of a 15% reduction required to demonstrate statistically significant improvement.
"Although we did not significantly reduce our primary endpoint, there were consistent findings that sacubitril/valsartan could represent an incremental improvement over ramipril," said Marc A. Pfeffer, MD, PhD, FACC, the study's lead author.
Sacubitril/valsartan was well-tolerated, had a favorable safety profile and was associated with a trend toward improvement in the trial's secondary endpoints, including cardiovascular death or HF hospitalization; HF hospitalization or outpatient treatment for HF; cardiovascular death, nonfatal MI or nonfatal stroke; cardiovascular death and total HF hospitalizations, MI or stroke; and all-cause death.
"This trial may not change guidelines, but it should make physicians even more comfortable using sacubitril/valsartan in their patients with [HF]," said Pfeffer.
AFib: Rhythm vs. Rate Control; Finerone; More
Is it possible to reduce HF events in patients with AFib and HF with a rhythm control strategy using catheter ablation rather than rate control with drugs and/or a pacemaker? The RAFT-AF trial showed the two strategies were similar for the primary composite outcome of time to death or HF progression.
In what the investigators say is the first of its kind, the trial included patients with AFib plus HFrEF (n=240) and with HFpEF (n=171). The findings suggest rhythm control may be beneficial for patients with HFrEF, though more research is needed to confirm this trend.
During a median follow-up of 37 months, 23.4% of patients in the rhythm control arm and 32.5% of those in the rate control arm died or had progressive HF requiring acute HF treatment (HR, 0.71; p=0.066). Among patients with HFrEF, 22.8% and 37.1% of the rhythm and rate control arms experiences a primary outcome event (HR, 0.63 vs. HR, 0.88 in HFpEF).
The trial used a PROBE design and was conducted in Canada, Sweden, Brazil and Taiwan, but was stopped early due to lower than expected enrollment and event rate and perceived futility, limiting its statistical power.
A prespecified analysis from FIDELIO-DKD showed that the novel drug finerenone reduced new-onset AFib in patients with chronic kidney disease and type 2 diabetes by 31% (p=0.016), a reduction seen at six months and sustained throughout the trial. The incidence per 100 patient-years was 1.20 with finerenone vs. 1.72 with placebo. Results were similar across prespecified patient subgroups.
It's often debated and now there is some evidence: alcohol consumption significantly increases the risk of an AFib episode. The HOLIDAY trial found that just one glass of wine, beer or other alcoholic beverage was associated with twofold greater odds of an AFib episode within the next four hours, and there was a threefold increase risk in those who consumed two or more drinks in one sitting. Furthermore, every 0.1% increase in inferred blood alcohol concentration over the previous 12 hours was associated with 38% greater odds of an AFib episode, and total alcohol consumption over time also predicted the chance AFib would occur.
Lightening Round
VOYAGER PAD found in a prespecified analysis that total event burden was significantly reduced with rivaroxaban on top of aspirin in patients with peripheral artery disease (PAD) who had lower extremity revascularization. An estimated 4.4 primary endpoint events and 12.5 vascular events were prevented with rivaroxaban for every 100 patients over three years. TIMI major bleeding was increased by 43% with rivaroxaban.
An initial report from SAFE-PAD found that paclitaxel-coated devices were noninferior to non-drug coated devices for mortality in Medicare beneficiaries who had femoropopliteal revascularization.
RAPID-TnT did not find that rapid, high-sensitivity cardiac troponin T in patients with suspected acute coronary syndrome but no ischemia on the initial ECG improved cardiovascular outcomes at one year.
In FLOWER-MI, for patients with STEMI and multivessel disease, complete revascularization guided by fractional flow reserve (FFR) did not have significant benefit over an angiography-guided strategy for risk of death, MI or urgent revascularization at one year. Conducted in France, the FFR-guided strategy was more expensive.
After TAVR, apixaban was not found to be superior to standard of care in the ATLANTIS trial for the primary endpoint, a composite of all-cause death, stroke, MI, valve thrombosis, pulmonary or systemic embolism, deep vein thrombosis or major bleeding, which occurred in 18.4% of the apixaban and 20.1% of the standard care groups.
RADIANCE-HTN TRIO showed that renal denervation was effective and safe in treatment-resistant hypertension, providing a greater reduction in daytime SBP at two months, with no difference in major adverse effects. Also compared with the sham procedure, 24-hr ambulatory SBP, nighttime ambulatory SBP and office SBP were all significantly lower with RDN.
Visit ACC.org/ACC2021 for full details of all these trials and more, along with perspectives from the ACC.org team, led by Kim A. Eagle, MD, MACC. Want more context and perspective? Listen to the ACC Cardiology Hour with Valentin Fuster, MD, PhD, MACC. Also explore the abstracts and posters from ACC.21, all available on demand.
Clinical Spotlight Sessions: Evidence and Perspectives to Support Best Practices
Every cardiovascular professional is challenged to keep pace with the constantly changing treatment landscape with new evidence disseminated almost daily through medical journals and scientific meetings. Four Clinical Spotlight Sessions held during ACC.21 – and now available on demand – focused on helping clinicians put new data and emerging therapies in context and understand their place in the treatment of their patients. Together these sessions shine a light on emerging science and best practices in the areas of sodium-glucose cotransporter 2 (SGLT2) inhibitors in cardiovascular disease, new heart failure (HF) treatments, lipids and new nonstatins, and anticoagulation.
SGLT2 inhibitors are the pill that pack a punch, says Javed Butler, MBBS, FACC, in the "Tracking the CV Impact of SGLT2i's: Practice Essentials" session. In his review of the journey of a drug developed to treat diabetes becoming a new therapy for the treatment of HF, Butler also reviews the epidemiology of HF and the pathophysiologic link between diabetes and HF. What is the impact of making an SGLT2 inhibitor the fourth pillar in the treatment of HF with reduced ejection fraction (HFrEF), along with an ARNI, beta-blocker and mineralocorticoid receptor antagonist? A number needed to treat of four to save one life over 24 months, says Michelle Kittleson, MD, FACC.
Dig deeper into HF treatment and the steps to optimize guideline-directed medical therapy with the session, "What's New in HF Pharmacotherapies: The What, How, and Wow." Leading experts review the role of SGLT2 inhibitors and how to add this new agent to current therapies in patients with HFrEF, as well as the use of sacubitril/valsartan in HF with preserved ejection fraction (HFpEF). The current evidence for emerging HF pharmacotherapies, including vericiguat in HFrEF, omecamtiv mecarbil, finerone and mavacamten, is reviewed by Nasrien Ibrahim, MD, FACC, and Carolyn S.P. Lam, MBBS.
The ever-expanding wide spectrum of lipid-lowering options for patients with atherosclerotic cardiovascular disease has substantially changed treatment strategies. "The Evolving Lipids Landscape: Current and Emerging Nonstatins" session, led by Salim Virani, MD, FACC, reviews lipid management in high-risk patients and practical approaches to patient selection and clinical implications of nonstatin therapies, including through case studies. The session also explores emerging risk assessment and the expanding toolbox including the potential with bempedoic acid, the PCSK9 inhibitor inclisiran, and the emerging role of Lp(a), Apo C-III, and ANGPTL3.
Test yourself and expand your knowledge of the best anticoagulation treatment strategy for your patients in a fast-paced session, "Anticoagulation Trivia from A to V: Management Strategies Across the Board," led by Geoffrey Barnes, MD, MSc, FACC. This cross-cutting interactive session covers the guideline-driven use of oral anticoagulants for atrial fibrillation, including initiation, dosing and management, especially pre- and post-PCI. Also addressed is the assessment and development of an anticoagulation treatment plan for patients with peripheral artery disease; identifying the anticoagulant drug, dose and duration for venous thromboembolism; and evaluating the acute to long-term anticoagulation needs for patients with COVID-19.
These free online courses are available on demand in ACC's Clinical Spotlight Series hub. Be sure to claim your continuing education credits and MOC points. Visit ACC.org/SpotlightSeries for these courses and more.
ACC.21 Explores New Research, Ongoing Challenges and Silver Linings of COVID-19 Pandemic
Given the continued focus on understanding, managing and treating COVID-19 in order to begin emerging from the pandemic, ACC.21 provided a global platform for reviewing the latest research, sharing of best practices and lessons learned, and discussions about new and emerging challenges and opportunities facing clinicians and patients globally.
A two-part COVID-19 Intensive offered unique insights into top-of-mind issues, including vaccine development, clinical trial conduct, the rapid pivot to virtual technologies and video for patient care and learning, and more. Additionally, leading experts from across the cardiovascular care team shared first-hand lessons in leadership and spoke to the important role global collaboration has played and continues to play in expediting research and optimizing patient care and outcomes.
The ACC was also honored to have Michelle A. Albert, MD, MPH, FACC, present the Louis F. Bishop Keynote as part of the Intensive, with a focus on health equity in cardiovascular health care as part of the Intensive (See side bar). Albert is professor of medicine and associate dean of admissions at the University of California, San Francisco, and director of the UCSF Center for the Study of Adversity and Cardiovascular Disease. She is also president of the Association of Black Cardiologists and president-elect of the American Heart Association.
The latest research was also the focus of several Late-Breaking Clinical Trial and Featured Clinical Research presentations. For example, findings from the DARE-19 trial found that compared with placebo, dapagliflozin did not significantly reduce the risk of organ failure or death or improve recovery in patients hospitalized with COVID-19 who were at high risk of developing serious complications. However, while researchers acknowledged the results were not statistically significant, they did note numerically fewer patients treated with dapagliflozin experienced serious adverse events and that the SGLT2 inhibitor was well tolerated, with numerically fewer serious adverse events than placebo.
Mikhail Kosiborod, MD, FACC, the study's principal investigator, said the "findings show that dapagliflozin is well-tolerated in patients hospitalized with COVID-19, with no new safety issues being observed" and suggested "this should have implications for clinical practice given that the results do not support discontinuation of SGLT2 inhibitors in this setting, as long as patients are monitored."
A separate study based on data from ACC's 2020 Well-Being Survey highlighted how the COVID-19 pandemic has taken a significant toll on cardiovascular clinicians, many of whom provide direct care to patients with or at greater risk of the virus. According to the study authors, the prevalence of burnout among cardiovascular professionals nearly doubled when comparing pre- to peak COVID-19 pandemic levels.
Outside of the Intensive and release of new research, other separate live and on-demand sessions explored additional groundbreaking changes in the multidisciplinary care of patients and varied ways that clinicians around the world are leveraging technology and innovation to improve their well-being, publish research, teach the next generation and build connections with each other. Specific sessions include: Art with Heart: Tales of Creativity in Cardiology; Global Perspectives on Value-Based Care; Wellness and COVID-19: Heal Thyself to Heal and Cure; COVID-19 and Echocardiography; Management of Pediatric Cardiology and Cardiac Surgery in the Post-COVID World; Thrombosis and Prevention in COVID-19; and more.
Search COVID-19 in the Program for a complete listing of COVID-related sessions. Access ACC's COVID-19 Hub for the latest clinical guidance, research, expert commentary and perspectives, and patient and clinician resources at ACC.org/COVID19. Find complete coverage of ACC.21 Late Breaking Clinical Trials and Featured Clinical Research at ACC.org/ACC2021.
ACC Global Heart Attack Treatment Initiative Shows Benefits in Improving Care in Low-, Middle-Income Countries
The ACC Global Heart Attack Treatment Initiative (GHATI) had measurable positive impacts on care delivery for heart attacks in low- and middle-income countries, according to data from the program's first year presented during a Featured Clinical Research presentation at ACC.21.
The ACC launched GHATI in 2019 to improve heart attack outcomes in low- and middle-income countries by encouraging adherence to guideline-directed medical therapy. While a person who suffers a heart attack in the U.S. or Europe has a 95-97% chance of survival, the odds are significantly worse in low- and middle-income countries, where the chance of survival is 80-90%.
Data from the first year of the program, reflecting STEMI treatment metrics and outcomes for more than 2,000 patients at 18 medical centers in 13 countries on four continents, reveal that around 90% of hospital admissions for a heart attack adhered to guideline-directed medical therapy. At the same time, the average time patients spent in transit to the hospital decreased by 38 minutes; cardiac arrest upon arrival decreased by 4.6%; and the time from first medical contact to the use of a device to open blocked arteries improved by 28%. All these factors are known to improve outcomes after a heart attack.
While the study is not a randomized controlled trial and cannot definitively attribute the improvements to the program, feedback from participants and a robust body of previous research on quality improvement suggests that the program has helped to encourage positive change, according to the researchers.
"It is obvious that there are chances to improve the systems and lower rates of cardiovascular death in low- and middle-income countries, and indeed in all countries," said Benny J. Levenson, MD, PhD, FACC, immediate past chair of GHATI. "We were pleased that the results, at one year, were heading in the right direction. We intend to continue to grow this program to be a model for many other countries to improve systems of care for heart attack and ultimately make a big impact on reducing mortality."
GHATI brings together ACC experts from around the world, including members of the College's Assembly of International Governors, with cardiology teams at participating institutions to establish systems for tracking patient encounters and collecting data on outcomes. Levenson said the program will continue to expand into more sites and countries, including top-performing medical centers and higher-income countries.
"The benefit to participating institutions starts with participating," Levenson said. "Places that have never collected data are now doing so. This leads to a culture change, because people and institutions learn to look closely at their practices and discuss their results with others. Just by gathering data, we can start to see a positive effect."
The ACC GHATI Work Group is led by Chair Cesar Herrera, MD, FACC, the Americas Representative for ACC's Assembly of International Governors, and B. Hadley Wilson, MD, FACC, chair-elect of the ACC Governance Committee.
"GHATI has been a real team effort, both by members of the Assembly of International Governors and within the ACC GHATI working group providing the program leadership," said Levenson.
More information about GHATI is available at ACC.org/GHATI.
Advancing Solutions to Diversity, Equity, Inclusion

Diversity, equity and inclusion are more than just words – all three tangibly impact both the receipt and delivery of care and ultimately patient outcomes. ACC.21 offered an opportunity for global conversations on ways social determinants of health, structural disparities, health economic factors, and lack of diversity in the profession directly effect patients and clinicians worldwide. Even more importantly, ACC.21 provided a forum for advancing solutions and driving action.
Leading experts shared their perspectives on overcoming racial/ethnic variations in care and how to improve quality for all, as well as how best to overcome the underrepresentation of women and other under-served populations in clinical trials. COVID-19, which has only further served to underscore health care inequities, was also an important topic. Additionally, on-demand sessions offered deeper dives into these topics, including how to incorporate and align diversity, equity, inclusion and belonging with standards of professionalism and ethics.
"In the months and years ahead, we must stay committed to help cardiovascular professionals and patients overcome challenges posed by histories of social, racial, and economic inequality," said ACC Immediate Past President Athena Poppas, MD, MACC, during the Opening Showcase. "COVID-19 has only served to underscore these persistent disparities. We must lead. This is the power of the ACC global community."
Filter the ACC.21 Program by "Diversity, Equity and Inclusion" for a complete listing of sessions. Click here (ACC.org login required) for a listing of ACC.21 Heart2Heart Conversation podcasts, which include conversations on achieving gender equity in cardiology and global perspectives on value-based care.
Clinical Topics: Acute Coronary Syndromes, Anticoagulation Management, Arrhythmias and Clinical EP, Cardiac Surgery, Cardiovascular Care Team, COVID-19 Hub, Dyslipidemia, Geriatric Cardiology, Heart Failure and Cardiomyopathies, Invasive Cardiovascular Angiography and Intervention, Prevention, Stable Ischemic Heart Disease, Atherosclerotic Disease (CAD/PAD), Anticoagulation Management and ACS, Anticoagulation Management and Atrial Fibrillation, SCD/Ventricular Arrhythmias, Atrial Fibrillation/Supraventricular Arrhythmias, Aortic Surgery, Cardiac Surgery and Arrhythmias, Cardiac Surgery and Heart Failure, Cardiac Surgery and SIHD, Lipid Metabolism, Nonstatins, Acute Heart Failure, Interventions and ACS, Interventions and Imaging, Interventions and Structural Heart Disease, Interventions and Vascular Medicine, Angiography, Nuclear Imaging, Chronic Angina
Keywords: ACC Publications, Cardiology Magazine, ACC21, ACC Annual Scientific Session, Acute Coronary Syndrome, Alcohol Drinking, Angiography, Angiotensin-Converting Enzyme Inhibitors, Atrial Appendage, Atrial Fibrillation, Anticoagulants, Atrial Flutter, Aspirin, Blood Pressure, Cardiac Rehabilitation, Cardiac Surgical Procedures, Cardiac Surgical Procedures, Cardiac Myosins, Cardiomyopathies, Cardiomyopathy, Hypertrophic, Cardiovascular Diseases, Catheter Ablation, Cholesterol, Catheters, Confidence Intervals, Confidence Intervals, Coronary Artery Bypass, Creatinine, COVID-19, SARS-CoV-2, Decision Making, Denervation, Depression, Diabetes Mellitus, Diabetes Mellitus, Type 2, Electrocardiography, Electronic Health Records, Ethnic Groups, Follow-Up Studies, Embolism, Fractional Flow Reserve, Myocardial, Glomerular Filtration Rate, Heart Rate, Heart Failure, Frail Elderly, Hospitalization, Hospitals, Length of Stay, Lung Diseases, Medicare, Lower Extremity, Minority Groups, Medical Futility, Myosins, Myocardial Infarction, Numbers Needed To Treat, Outpatients, Obesity, Paclitaxel, Pacemaker, Artificial, Patient Discharge, Patient Readmission, Patient Preference, Peripheral Arterial Disease, Physicians, Platelet Aggregation Inhibitors, Potassium, Patient-Centered Care, Pyrazoles, Pyridones, Quality of Life, Reference Standards, Ramipril, Renal Insufficiency, Chronic, Risk, Risk Factors, Self Report, Secondary Prevention, ST Elevation Myocardial Infarction, Stroke, Stroke Volume, Standard of Care, Thrombosis, Venous Thrombosis, Troponin, Troponin T, Transcatheter Aortic Valve Replacement, Vulnerable Populations


