From The Member Sections | Endovascular Medicine and Interventional Training: Building a Workforce For an Unmet Need
A combined endovascular medicine and interventional fellowship is a subspeciality training program that is most commonly pursued following interventional cardiology training. Such programs typically focus on training in both invasive and noninvasive knowledge and skills pertaining to vascular patient care.
Trainees pursue education in medical, noninvasive and invasive management of a broad cadre of vascular disease conditions. These may include but are not limited to thrombosis; venous disease; peripheral artery disease (PAD) including carotid and renal disease; and nonatherosclerotic arterial disease, including vasculitides, aneurysmal disease and arteriopathies.
Additionally, trainees are provided the opportunity to become confident in mastering interpretation of noninvasive vascular testing; they are then eligible for completing certification through the Registered Physician in Vascular Interpretation examination. Trainees also gain experience to review other forms of noninvasive cross-sectional imaging modalities, including computed tomography angiography and magnetic resonance angiography.
There are only a select few endovascular interventional training programs in the U.S. These include Brown, Columbia, First Coast Cardiovascular Institute, Massachusetts General Hospital, Mt. Sinai Medical Center, University Hospital Cleveland Medical Center, and Yale.
Each program accepts one to three fellows during each recruitment cycle, and the duration of the fellowship is one year. After completion of endovascular medicine and interventional fellowship, trainees are eligible to complete the American Board of Vascular Medicine's Endovascular and Vascular Medicine examinations.
CardioSmart Resources
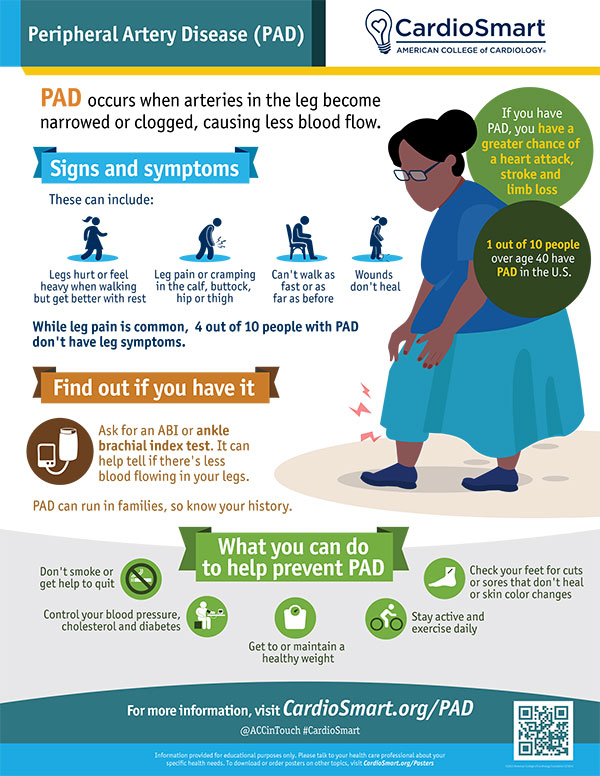
Visit CardioSmart.org/PAD to download this new free infographic, also available in Spanish, and all the PAD resources for patients.
Nationally, there is increasing demand for physicians with expertise in the management of vascular disease. Although PAD comprises only a subset of the patients that vascular experts evaluate, the epidemiology and underdiagnosis of PAD serves as an excellent example for the need for qualified clinicians. Between 12% to 20% of patients over the age of 50 have PAD.1
PAD represents a manifestation of atherosclerotic cardiovascular disease, and approximately 44% of patients with symptomatic PAD also have coronary artery disease and/or cerebrovascular disease; these patients are at highest risk for major adverse cardiovascular events.2,3
In the PARTNERS study conducted in primary care practices in the U.S. in 1999, 83% of patients in the study had PAD, but only 49% of physicians were aware that the patients carried this diagnosis.4 Moreover, medical student and trainee examinations have demonstrate poor to modest knowledge regarding PAD-related assessment.5
Vascular medicine and endovascular intervention are growing rapidly and gaining support and representation among multiple medical communities, including the ACC along with the Society of Vascular Medicine, Society for Cardiovascular Angiography and Interventions, and the Cardiovascular Research Foundation.
Join Your Community
ACC's Member Sections are important communities within your professional home. Click here to learn about the Vascular Disease and the Interventional Sections. Join today and help drive your fields forward.
Over the last decade, there has been a substantial increase in the literature related to medical management of these underrecognized and underserved patients. Additionally, there have been substantial advances in the endovascular technologies available to treat patients with vascular disease.
The longstanding paradigm of fellowship training in cardiology with the addition of a single year of coronary interventional training is no longer adequate to train physicians for the skills and perspective required to diagnose, manage and treat patients with complex vascular diseases.
There remain many unanswered questions regarding best practices in the care of patients with vascular disease, setting the stage for important academic research, and opportunities for fellows and trainees with the appropriate perspective and qualifications to continue to develop the field of vascular medicine.
Training in endovascular intervention is well-suited for physicians who desire to incorporate imaging, medical treatment and interventional therapies. Training in an endovascular medicine and interventional fellowship will enable physicians to provide important perspectives and technical skill to recognize patients with panvascular disease, and to improve care and outcomes in this complex, underappreciated and vulnerable patient population.
This article was authored by Maya Serhal, MD, FACC; Douglas E. Drachman, MD, FACC; Joseph M. Garasic, MD, FACC; Gaurav Parmar, MD, FACC; Kenneth Rosenfield, MD, FACC; Rahul Sakhuja, MD; Ido Weinberg, MD, MSc, FACC; and Robert M. Schainfeld, DO, all at Massachusetts General Hospital in Boston, MA.
References
- Benjamin EJ, Virani SS, Callaway CW, et al. Heart disease and stroke statistics—2018 update: A report from the American Heart Association. Circulation 2018;137: e67-e492.
- Hiatt WR, Fowkes FG, Heizer G, et al. Ticagrelor versus clopidogrel in symptomatic peripheral artery disease. N Engl J Med 2017;376: 32-40.
- Gutierrez JA, Mulder H, Jones WS, et al. Polyvascular disease and risk of major adverse cardiovascular events in peripheral artery disease: A secondary analysis of the Euclid trial. JAMA Netw Open 2018;1:e185239-e185240.
- Hirsch AT, Criqui MH, Treat-Jacobson D, et al. Peripheral arterial disease detection, awareness, and treatment in primary care. JAMA 2001;286:1317-24.
- Bridgwood BM, Nickinson AT, Houghton JS, et al. Knowledge of peripheral artery disease: what do the public, healthcare practitioners, and trainees know? Vasc Med 2020;25:263-73.
Clinical Topics: Vascular Medicine, Atherosclerotic Disease (CAD/PAD)
Keywords: ACC Publications, Cardiology Magazine, Fellowships and Scholarships, Coronary Artery Disease, Cerebrovascular Disorders, Peripheral Arterial Disease
< Back to Listings

