For the FITs | Cardiology in the Post COVID-19 Era: Less Essential Than Before?
Several times a year I'm invited to speak to underserved youth who aspire to become future health care providers.
During these events, I'm frequently asked: Why did you choose cardiology?
I've always pointed out the heart is (literally) central for maintaining health and that cardiovascular disease continues to be the most significant source of morbidity and mortality in the U.S.
In this regard, I've always felt that through my training I was curating a medical skill set that would remain a critical component of patient care.
Then New York City became the epicenter for the COVID-19 pandemic and I began to question the notion that cardiovascular care was essential.
A New Reality: Coming To Terms

Like many of my colleagues, I went through a reflection process akin to the five stages of grieving. Early on, I was in denial that COVID-19 would impact my way of life: Perhaps this disease would be limited to those on cruise ships and on the West Coast.
When New York City had its first case, I was angry: Why was the spread to NYC allowed to happen and why wasn't the individual from the index case immediately quarantined?
When it became evident that the virus could not be contained, I reassured myself through bargaining: Maybe only those with certain comorbidities were at risk and hospital resources could be temporarily reallocated until the curve flattened.
As the weeks wore on with unthinkable mortality occurring even in the young and healthy, I had to accept the harsh reality: No one was immune from COVID-19 and its treatment would become the focus of the foreseeable future.
Shifting Demand For CV Services
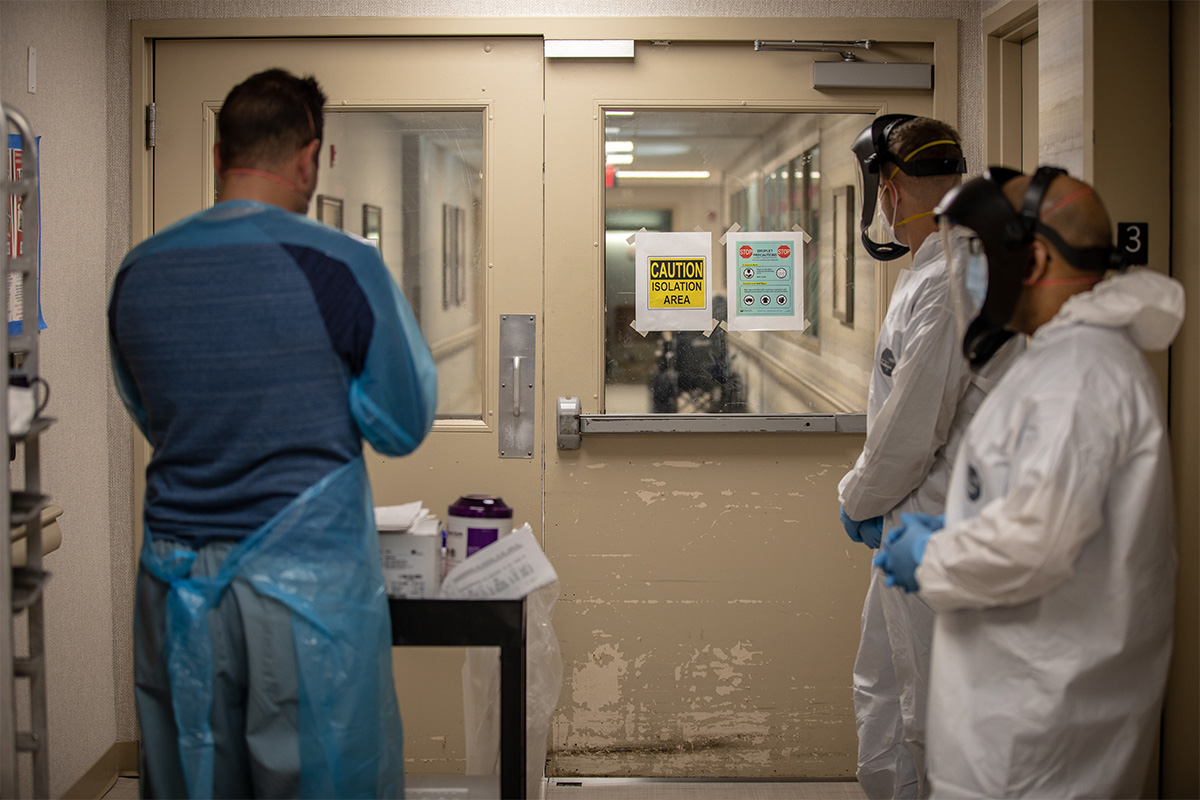
When Mount Sinai Hospital decided to reassign housestaff to the front lines, the cardiology fellows were initially protected to maintain adequate staffing on presumably essential cardiovascular services: it seemed unlikely that patients were going to stop developing heart attacks, congestive heart failure and lethal arrhythmias.
However, the expected burden of cardiovascular disease never materialized.
For any patient, a positive COVID-19 test result became the new "troponin," demanding immediate attention and often superseding further workup of coexisting cardiovascular conditions, especially those involving invasive management.
The majority of STEMIs and ventricular tachycardias that would have otherwise been treated with PCI and ablation were instead managed with thrombolytics and antiarrhythmics, respectively. The nonstop interrogation requests for pacemakers and defibrillators dwindled.
Over time, elective and outpatient office visits and scheduled procedures were deferred. Where did all the cardiology patients go?
Moved to the Front Line

Ironically, not long after writing my article for the May issue of Cardiology on the value of exposing future cardiologists to noncardiology-related conditions, I was deployed as a frontline provider to one of the many, newly converted COVID-19 ICUs.
Although I was eager to help, I was unsure how relevant I would be: it had been many years since I had to recall the nuances of adjusting ventilator settings in acute respiratory distress syndrome (ARDS), titrating an insulin drip in diabetic ketoacidosis (DKA), and initiating tube feedings.
Eventually, I applied my electrophysiology (EP) knowledge towards reading QTc intervals prior to hydroxychloroquine use, placing central lines prior to dialysis, and performing point of care ultrasounds to assess volume status.
While I still believe the length of subspecialty training can be abbreviated, I developed a newfound appreciation for how comprehensive my training had been.
Return to Normal?

Over the last month, the number of COVID-19 cases have steadily decreased. The COVID-19 ICUs have been largely disbanded, house staff has been sent back to their prior training programs, and elective office visits and procedures have resumed.
However, there has not been a significant reappearance in cardiology cases. It is not obvious what caused the initial disappearance of cardiovascular disease during the COVID-19 pandemic and it is even less clear what continues to suppress the burden of cardiovascular disease now that the pandemic is resolving.
Undoubtedly, patients will be reluctant to seek medical attention, but it is difficult to think that alarming cardiac symptoms like crushing chest pain, worsening dyspnea and unexplained syncope can be continuously ignored.
In New York City, most EP laboratories have resumed operational capabilities but procedure volumes have returned to only a fraction of normal capacity. It doesn't help that a significant number of the scheduled cases tend to be elective (such as atrial fibrillation ablation), dictated heavily by patient preference (such as left atrial appendage occlusion), or have debatable indications (from "negative" trials such as CABANA).
As a fellow, my most immediate concern is the impact of the decreased caseload on my training competency. But the more important question related to my career trajectory is whether cardiology will ever recover. Thankfully, I still have another year of EP fellowship remaining, but the looming fear of a second wave of COVID-19 infections this winter season does not bode well.
With education slowly becoming a priority and summer camps going virtual, health care professions will undoubtedly be a topic of interest for the next generation of college-bound students. When I am asked "Why did you choose cardiology?" on the next Zoom call, my answer may not be as obvious.
Clinical Topics: Arrhythmias and Clinical EP, COVID-19 Hub, Heart Failure and Cardiomyopathies, Invasive Cardiovascular Angiography and Intervention, Implantable Devices, EP Basic Science, SCD/Ventricular Arrhythmias, Atrial Fibrillation/Supraventricular Arrhythmias, Novel Agents, Statins, Acute Heart Failure
Keywords: ACC Publications, Cardiology Magazine, COVID-19, Internship and Residency, Fellowships and Scholarships, Pandemics, Point-of-Care Systems, Respiratory Distress Syndrome, Respiratory Distress Syndrome, Hydroxychloroquine, Atrial Fibrillation, Reading, Cardiovascular Diseases, Patient Preference, Diabetic Ketoacidosis, Troponin, New York City, Outpatients, severe acute respiratory syndrome coronavirus 2, Percutaneous Coronary Intervention, Cardiology, Arrhythmias, Cardiac, Anti-Arrhythmia Agents, Tachycardia, Ventricular, Defibrillators, Heart Failure, Cardiology, Patient Care, Morbidity, Respiration Disorders, Health Personnel
< Back to Listings


