Cover Story | NCDR at 25: Transforming Cardiovascular Care and Saving Lives
Behind the best care lies the best data. For 25 years, the ACC's NCDR has provided these data (and more), helping hospitals, health systems and other facilities optimize patient care, outcomes and operational decisions through data-driven insights, analysis and research.
The NCDR was born out of a quest to answer questions that were beginning to emerge at that time around whether metrics, data collection and outcomes analysis could improve the quality of health care. Members of the ACC's Database Committee, including Bill Weintraub, MD, MACC, Chuck McKay, MD, FACC, H. Vernon Anderson, MD, FACC, and Dick Shaw, PhD, FACC, envisioned the College's first registry – the CathPCI Registry – as more than just a database, but rather a tool for improving quality.
"The future of medicine is increasingly in the hands of those who are effective users of clinical data," said Weintraub, et al., writing in 1997 in JACC about the vision for the registry. Weintraub, often called the "Godfather of NCDR," wasn't wrong.

The future of medicine is increasingly in the hands of those who are effective users of clinical data.
– Bill Weintraub, MD, MACC
Since then, NCDR's reach has grown from the flagship CathPCI Registry into a suite of registries addressing major clinical areas, including acute myocardial infarction (AMI), ICD implantation, lower extremity peripheral vascular interventions, atrial fibrillation (AFib) ablation, TAVR, left atrial appendage occlusion (LAAO) procedures, and pediatric and adult treatment of adult congenital heart disease, as well as outpatient care for cardiovascular conditions.
According to Debra Ness, MS, who served as the first consumer/patient representative on the NCDR Oversight Committee, NCDR's many contributions to improving quality and helping to make richer and more granular evidence and more rapid generation of evidence about what does and doesn't work have contributed to meaningful and tangible benefits to cardiovascular patients over the last 25 years.
Delivering Results
What started as a mission to provide quality benchmarking data on individual hospital performance compared to the national average, has grown over more than two decades into a comprehensive suite of registries that are helping measure and quantify quality improvement, identify and close gaps in guideline-recommended care, and optimize the implementation and use of new treatments and therapies.

You can't improve what you can't measure, and the NCDR provides dozens of measurement points for internal and external comparative studies.
– William J. Oetgen, MD, MBA, MACC
"You can't improve what you can't measure, and the NCDR provides dozens of measurement points for internal and external comparative studies," says William J. Oetgen, MD, MBA, MACC. No other resource provides this wealth of curated data for hospital and health system improvement activities."
Among its many successes, NCDR has played a key role in helping hospitals and health systems reduce door-to-balloon times to guideline-recommended levels; control costs associated with preventable procedural complications like PCI bleeds; reduce avoidable hospital readmissions; and ensure safe and effective implementation of TAVR in the U.S. Not to mention, registry data have been used in hundreds of clinical studies published in leading peer-reviewed medical journals, including JACC, over the last two decades.
"While research is not the principal objective of the registry programs, NCDR has now contributed to more than 500 peer-reviewed papers in the medical literature and has done a lot to advance our understanding of cardiovascular care in the 'real world' – more than any other data source imaginable," says Frederick A. Masoudi, MD, MSPH, FACC.
Partnering For Success
This success and growth of the NCDR is in part due to collaborations across the cardiovascular community, including with the Society of Thoracic Surgeons and the Society for Cardiovascular Angiography and Interventions.
"The NCDR has shown how intersocietal collaboration and cooperation can contribute to the safe and efficacious development of innovative medical technologies that have transformed the practice of cardiovascular surgery and medicine," says Oetgen, who cites the STS/ACC TVT Registry, which celebrated its 10-year anniversary this year, as one of the best examples of collaboration in action. To date, the STS/ACC TVT Registry has captured the outcomes on >400,000 patients undergoing TAVR procedures in the U.S., representing virtually every patient treated in nongovernment institutions and outside of clinical trials.
External influencers like the Centers for Medicare and Medicaid Services (CMS), U.S. Food and Drug Administration, Centers for Disease Control and Prevention, the National Quality Forum, payers, industry stakeholders and innovation partners have also played an important role in NCDR's growth and expansion.

High quality cardiovascular care is a team sport and NCDR has operated, from the beginning, with a broad definition of 'team.
– Janet Wright, MD, FACC
Industry buy-in was among the key drivers of the STS/ACC TVT Registry's early success "given the uncertainties … of introducing an innovative medical device into clinical practice," according to a recent article by David R. Holmes Jr., MD, MACC, and Michael J. Mack, MD, MACC.
Other examples include the linking of data from the STS/ACC TVT Registry, EP Device Implant Registry (formerly the ICD Registry) and the LAAO Registry with CMS national coverage determinations over the years to provide evidence development and proof of compliance with reimbursement criteria. The National Quality Forum has also endorsed performance measures from several registries that are used in NCDR's voluntary public reporting effort, which publicly reports certain NCDR metrics to help patients make informed choices and enables participating sites to demonstrate their commitment to quality improvement.
Most recently, the College has been working with Carta Healthcare, a health care analytics company and an ACC Innovation Program partner, to bring an artificial intelligence solution to help mitigate the strain on time and resources associated with registry-related data collection and submission.
"High quality cardiovascular care is a team sport and NCDR has operated, from the beginning, with a broad definition of 'team,'" says Janet Wright, MD, FACC. "Excellence in cardiovascular care and health outcomes requires complementary contributions from all specialties, many federal and state agencies, payers, and the device and pharmaceutical sectors. Over its history, NCDR leaders have listened to the needs of their stakeholders. The results are registries, processes and support services that meet or exceed those needs for access to timely data and expertise, insights into key issues in cardiovascular care, and educational opportunities ready-made for clinicians, practices and health systems."
Looking Ahead
"NCDR's leadership and staff along with participants have grown a culture of quality improvement throughout the cardiovascular community," says Wright. "Through collaborations with experts and other societies, NCDR has provided the metrics, the mechanisms, and the megaphone to ensure high performance among clinical teams and the best outcomes for patients. In addition, NCDR has facilitated the spread of best practices and learning opportunities highly valued by cardiovascular care teams worldwide."

Looking ahead to the next 25 years, there's a real opportunity to leverage the timely data, expertise and real-world insights to foster and grow a true local, national and international learning health care environment.
– Ralph G. Brindis, MD, MPH, MACC
So how do we sustain these successes and also continue to meet the future needs of hospitals and health systems and the clinicians and patients they serve? As the U.S. health care system continues to transition to a value-based model, the need to track health care outcomes through registry programs like the NCDR is only more critical. In addition, the COVID-19 pandemic has further highlighted the critical global need to address health equity and social determinants of health. The NCDR has a real opportunity to help lead and drive solutions in this area.
"When I think about opportunities for NCDR, I think there are great frontiers out there," says Ness. "I would like to see the results of the information that's generated from the registries result in better tools for clinicians, but also something that patients are more aware of and can potentially use." According to Ness, this could involve embedding information in patient or participating practice portals, or closer alliances with community health centers.
On a similar note, Wright says the time is now to bring together the clinical and social determinants of cardiovascular health to drive action. "As ACC continually builds upon its strong foundation in prevention, NCDR can help lead the way in driving success in measures that matter through collaborations with state and local health departments and other public health organizations rooted in communities across the country," she says.

The Quality Summit also celebrated the 25th Anniversary of the NCDR. "We have much to celebrate," said Ralph G. Brindis, MD, MPH, MACC. "The growth of the NCDR registry portfolio from the very first registry – the CathPCI Registry – in 1997 to our current suite of registries has helped hospitals and other facilities around the world improve their patient outcomes and play a central role in transforming cardiovascular care through use of robust risk adjustment, hospital and physical benchmarking, and important feedback. The Quality Summit was the perfect place to kick off this next chapter."
Continuing to leverage new technologies to ease data burden and streamline clinician and even patient access is also important. "Merging NCDR data with CMS administrative data, cost data, and/or data from electronic health records will promote further value for participants through obtaining better longitudinal patient follow-up and valuable lessons learned through cost analyses and treatment efficiencies," says Ralph G. Brindis, MD, MPH, MACC. He also advocates for increasing patient assessments and involvement through patient-reported outcomes embedded in the registries.
More broadly, both Brindis and Masoudi stress the strength of the NCDR in providing local, national and global insights and real-world evidence that can deliver true care transformation and improvements in heart health for all.
"The growth of the NCDR registry portfolio from the very first registry – the CathPCI Registry – in 1997 to our current suite of registries has helped hospitals and other facilities around the world improve their patient outcomes and play a central role in transforming cardiovascular care through use of robust risk adjustment, hospital and physical benchmarking, and important feedback," says Brindis. "Looking ahead to the next 25 years, there's a real opportunity to leverage the timely data, expertise and real-world insights to foster and grow a true local, national and international learning health care environment."
Reflections on NCDR

Debra Ness, MS: "The focus on equity and the impact of everything we do on patient populations is the next frontier. We need to routinely build health equity into anything/everything we do. We need to partner with patients; practice transparency and accountability; and find ways to build trust with diverse populations that have very good reasons to not be trusting. Everything needs to be looked at through the equity lens."

William J. Oetgen, MD, MBA, MACC: "My biggest source of NCDR pride was always the fabulous and brilliant collaboration between the NCDR member leaders and the ACC nurse-manager and technical staff at the Heart House. It was a pleasure to see, and I count them all as my most treasured professional colleagues.

Ralph G. Brindis, MD, MPH, MACC: "In terms of NCDR's successes in our first 25 years so much comes to mind! First, was the vision, optimism and foresight of ACC leadership to start the endeavor! Previous attempts at cardiovascular registries were unsuccessful and financially unsustainable due to a multitude of reasons. It is exciting to see how this vision has grown from a group of leading hospital and physician "early adopters" to be embraced by a broad constituency of stakeholders including hospitals, physicians, industry, regulatory agencies, purchasers, payers and patients!"
Masoudi Reflects on 25 Years of Quality Improvement With NCDR

Frederick A. Masoudi, MD, MSPH, MACC, has been involved with NCDR since 2007, first as a member of the ICD Registry Research and Publication Committee and then serving as the longtime chair of the NCDR Oversight Committee. His continued work with the NCDR family of registries along with his professional commitment to quality improvement makes him uniquely qualified to discuss NCDR's 25-year history and consider what the next 25 years of NCDR will mean for the future of cardiovascular care.
What first prompted you to become involved in NCDR's family of registries?
What attracted me to the registries was my fundamental interest in how to improve quality and transform care, and an appreciation that this can only be done with the availability of standardized, clinical data. I recognized early that this data needs to be collected in a standardized way to truly characterize the quality of care that patients receive and to truly understand the factors that may relate to the outcomes they experience in the hospital and beyond.
What are some of NCDR's greatest accomplishments over the last 25 years?
What attracted me to the registries was my fundamental interest in how to improve quality and transform care, and an appreciation that this can only be done with the availability of standardized, clinical data.
– Frederick A. Masoudi, MD, MSPH, MACC
The NCDR has done a number of remarkable things that reflect the College's dedication to its Mission to transform cardiovascular care and improve heart health for every patient. To think that a professional society is going to lead its members to think about quality in an environment where there is very little financial incentive to do so is a real tribute to the ACC and NCDR. Another big accomplishment has been the NCDR's responsiveness to the coverage with evidence development program from the Centers for Medicare and Medicaid Services (CMS). The NCDR has allowed hospitals to participate in these decisions in a meaningful way, and in so doing answer questions that are of key importance to CMS.
While research is not the principal objective of the registry programs, NCDR has now contributed to more than 500 peer-reviewed papers in the medical literature and has done a lot to advance our understanding of cardiovascular care in the "real world" – more than any other data source imaginable. Ultimately, NCDR has provided support for quality improvement in a way that has touched the lives of more than 100 million individuals, which is truly its biggest accomplishment.
What has been the highlight of your time working with NCDR registries?
The highlight for me has been participating in the ACC Quality Summit conference because I always find it such a refreshing and renewing experience. It provides such a perspective on the community of people who are dedicating themselves to improving patient care. There is so much enthusiasm, so much promise, so much mutual aspiration to do better, that it is hard to match the energy and inspiration that comes from the conference.
What do you believe the future of NCDR looks like?
Ultimately, NCDR has provided support for quality improvement in a way that has touched the lives of more than 100 million individuals, which is truly its biggest accomplishment.
– Frederick A. Masoudi, MD, MSPH, MACC
My hope is that other areas of medicine beyond the registries that already exist will think hard about adopting this approach to improving care. I think we also acknowledge that participation in a program like NCDR requires a tremendous amount of commitment and time and effort, particularly as it relates to collecting the data required by this clinical granularity that is so important to the work we do. For this reason, addressing the data burden by identifying novel, tech-enabled approaches to collecting data is important.
We also need to figure out better approaches to collect data more completely – potentially directly from the patient involved – and think more about the impact of cardiovascular disease beyond those issues that are currently easy to measure. I also think part of the future is in better characterizing the patient's experience. And finally, we need to understand the value of care. We have focused a lot on quality, but in a time of increasingly scarce resources, we need to be thinking about prioritizing those things that best improve quality and do so at the lowest possible cost.
Medical Education on YouTube?
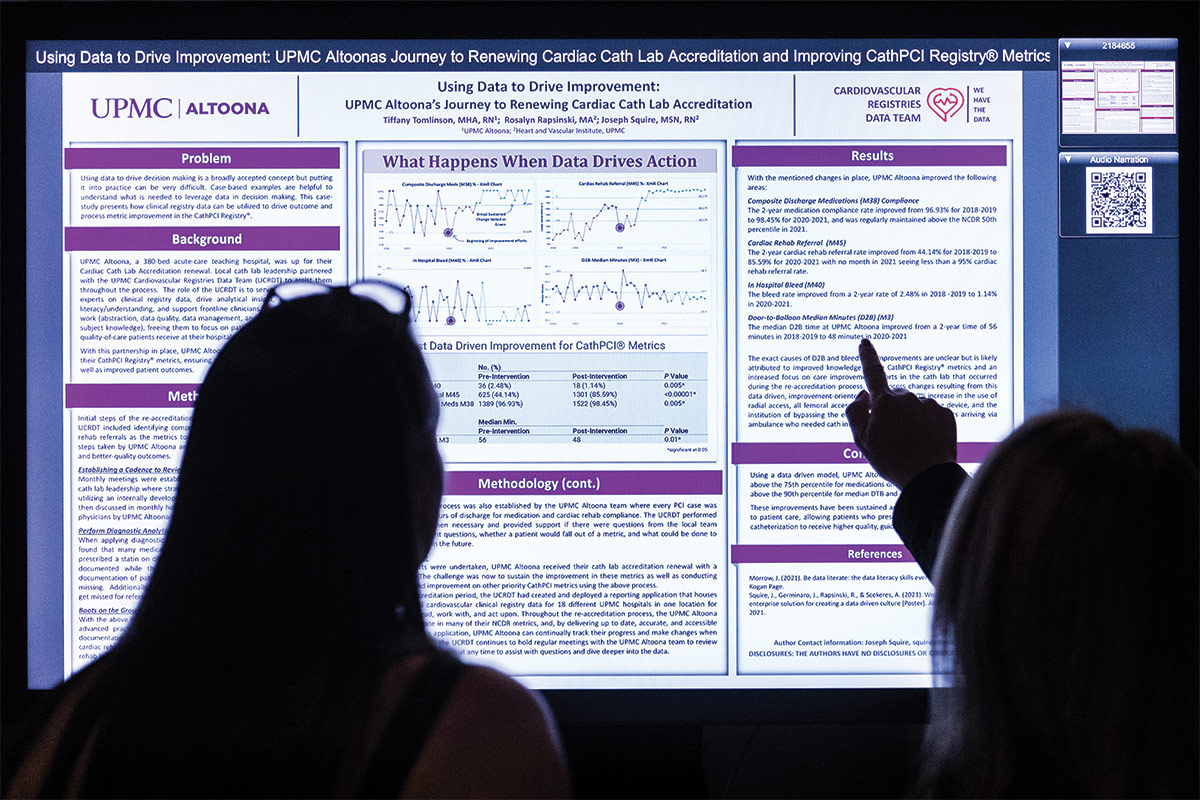
Are YouTube videos a high-quality educational resource for patients contemplating an ICD? The accuracy – or lack thereof – was among the topics addressed as part of the robust poster and abstract presentations that took place during the ACC Quality Summit 2022.
According to the researchers, the study demonstrates an opportunity for medical institutions to help patients by implementing new strategies to improve video content, quality and visibility as more patients seek online resources for patient education. Click here for the full story.
Quality Summit Celebrates Current Achievements
Looks to Future of NCDR and Accreditation
Effectively equipping clinicians, hospitals, health systems and other facilities and stakeholders with tools and best practices for designing, leading and ultimately achieving quality care was the focus of this year's ACC Quality Summit, which took place Sept. 14-16 in Los Angeles.
Over the course of three days, participants had the opportunity to take part in hands-on education and workshops, network and share best practices with colleagues from across the U.S., and gain insights and inspiration from cardiovascular leaders and experts, including the opening plenary and the Ralph G. Brindis Keynote speaker, Frederick Masoudi, MD, MSPH, MACC, on the many ways patient data can drive process improvement initiatives.
Chaired by David Winchester, MD, FACC, the Summit was divided into four tracks looking at the present and future directions of NCDR and ACC Accreditation Services; best practices in cardiovascular care; leadership roles in quality improvement; and how to measure success to improve patient outcomes. General sessions addressed topics related to using NCDR data to understand inequities in care, rebuilding the cardiovascular team post COVID, and how innovative technology can and will change the cardiovascular landscape.
Meanwhile, registry, leadership and accreditation-focused tracks looked at issues like medication management in patients undergoing left atrial appendage occusion; choosing the best atrial fibrillation ablation strategy; building a successful structural heart program; improving cardiac rehabilitation referrals; and more.
Here are a few of our favorite images capturing highlights from the meeting. Have your own? Share them with @ACCinTouch and use #CardiologyMag.
Clinical Topics: Congenital Heart Disease and Pediatric Cardiology, COVID-19 Hub, Congenital Heart Disease, CHD and Pediatrics and Quality Improvement
Keywords: ACC Publications, Cardiology Magazine, National Cardiovascular Data Registries, Registries, CathPCI Registry, LAAO Registry, AFib Ablation Registry, STS/ACC TVT Registry, Heart Defects, Congenital, COVID-19
< Back to Listings