Cover Story | Critical Care, Cardiology and COVID: 20/20 Vision on Pandemic Experience and a Nascent Critical Care Cardiology Subspecialty
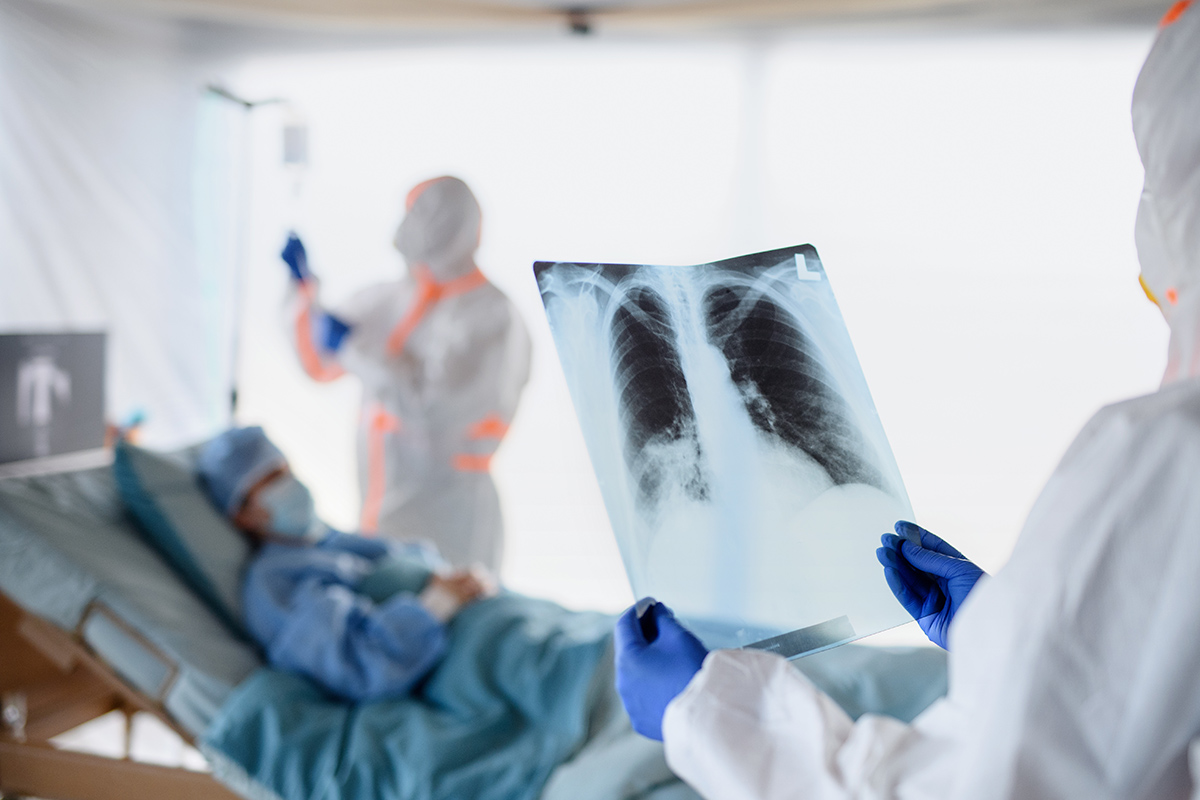
The second week of March 2020 in Boston – when temperatures finally exceeded 60 degrees Fahrenheit – was not greeted by discarding winter coats, resuming outdoor recreation and blooming flowers. Rather, it heralded the first admissions of critically ill patients with COVID-19 at my hospital, along with uncertainty and a flurry of conference calls, briefings and emergency planning efforts.
Massachusetts General Hospital (MGH) where I practice is an urban academic medical and research center, as well as a thousand-bed general hospital, guided by its founding mission: "When in distress, every person becomes our neighbor."
My colleagues in pulmonary and critical care, emergency medicine, and infectious disease were paramount in the institutional response to meet our charge to our surrounding community. Importantly, cardiovascular professionals, and resources in our cardiology division, filled key institutional roles responding to the COVID-19 pandemic.
I am a critical care cardiologist and was attending in our 16-bed cardiac intensive care unit (CICU) during the second and third weeks of March. In the institutional triage grid, our CICU became the first nonmedical ICU dedicated to the care of critically ill COVID-19 patients, given existing cardiology/critical care presence, 24/7 house officer coverage, available negative pressure rooms, and collective expertise of staff, nurses and respiratory therapists in respiratory failure and acute respiratory distress syndrome.
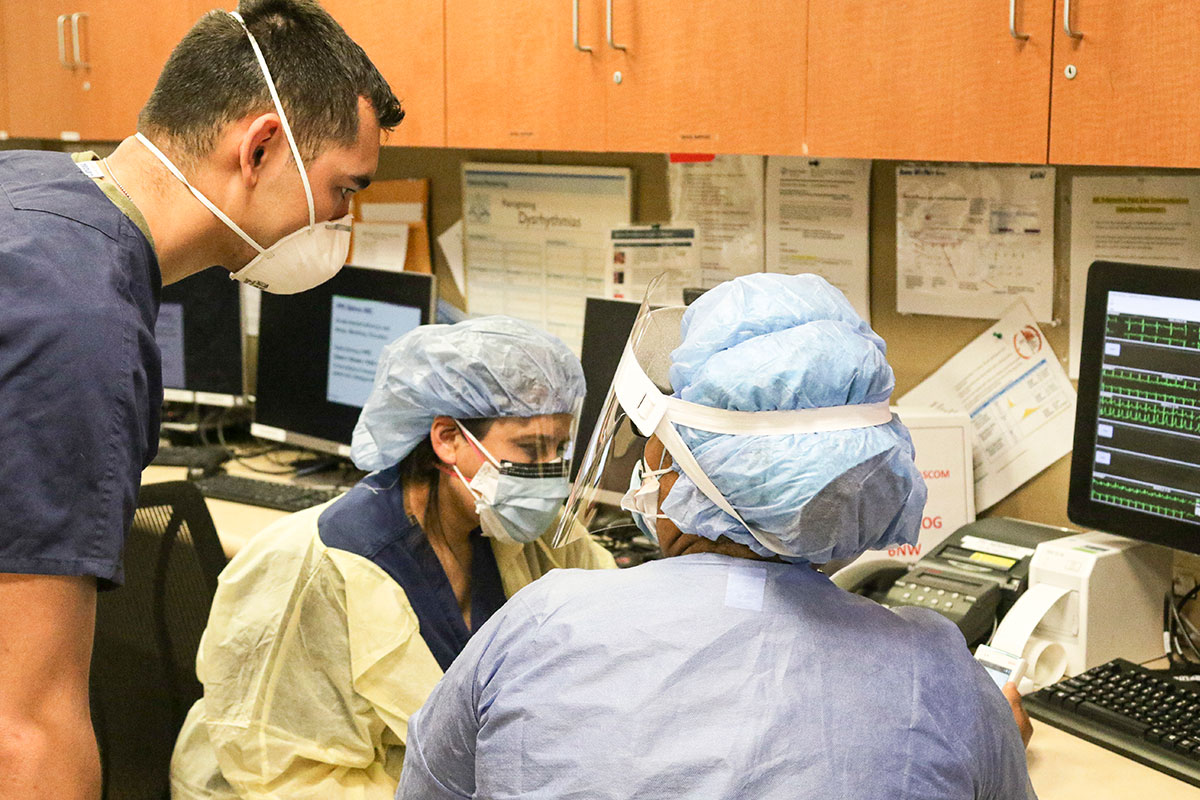
The first days of the COVID-19 pandemic were characterized by rapid multidimensional process changes in all cardiology inpatient and ICU service lines. We radically reorganized rounds across all cardiology units so that large rounding groups, typical of teaching-style rounds, were streamlined to minimum necessary personnel for conducting patient examinations and formulating plans; this change conserved personal protective equipment and minimized potential viral transmissions.
We focused on optimizing collaboration with nurses and respiratory therapists. Recognizing these professionals represent front-line patient care, there was attention to ensuring laboratory and other testing was minimized, and batching care with physicians and trainees bringing materials into rooms, performing assessments or running scheduled blood pressure checks.
Critical care cardiologists (CCC) found themselves in the early pandemic considering COVID-19 on the differential diagnosis or as contributing to otherwise standard CICU diagnoses, including out-of-hospital arrest, acute coronary syndrome, atrial flutter with hypotension, acute cor pulmonale, pericardial effusion and tamponade, and complete heart block.
Triage of critically ill patients across my institution was subject to ongoing revisions, in part to actively cohort similar ICU patients with similar resource and care team needs, cohort care of COVID-19 patients, and maximize use of all available ICU capacity. CICU cardiologists covered patients in various new locations, including patients in the cardiac surgical ICU; CICUs worldwide responded with various staffing paradigms.1,2
Explosive acceleration of the pandemic in Boston and neighboring cities resulted in all 16 beds of the CICU being occupied by critically ill COVID-19 patients by March 31. Partnership with pulmonary/critical care intensivists was essential for expertise and around-the-clock care, along with fellows (both cardiology and pulmonary/critical care).

CICU cardiologists who could not work in direct COVID-19 patient care took on roles in virtual consults for ICU patients, as well as assisting infectious disease colleagues in triage and testing roles.
Introduction of extracorporeal membrane oxygenation (ECMO) patients to the CICU had been discussed prepandemic as a future goal, but during the pandemic ECMO cannulations for refractory hypoxemia and cardiogenic shock were undertaken. Teams for invasive procedures and for prone positioning were implemented to bring expertise to these critical care roles.
My hospital's need for ICU beds for critically ill COVID-19 patients was staggering and quickly outstripped initial plans. By peak demand in April there were 164 such patients, about double our normal hospital ICU bed complement.
During April, neo-ICUs were created from postanesthesia care units and even general floors, and critical care cardiologists, as well as veteran critical care nurses specifically from the CICU, were redeployed to new units.
Because a typical cardiology fellowship embeds four to six months of critical care experience, senior cardiology fellows served as a key locus of expertise and labor pool for neo-ICUs; advanced fellows were recruited as not only responding clinicians, but some as junior attendings depending on seniority and ability to undergo emergency credentialing.
Education, Outreach Supporting Staff

With urgent mobilizations to novel roles, our institution prioritized educational initiatives and outreach to help every type and level of practitioner prepare for critically ill COVID-19 patients. Three cardiology Grand Rounds in March alone were focused on viral biology and epidemiology, pathophysiology and manifestations of acute COVID-19, and ventilator and ICU management of COVID-19.
Led by a multidisciplinary group of critical care doctors – pulmonary, anesthesiology, surgery and cardiology – MGH produced multiple efforts that not only benefitted intramural learners, but extramural education worldwide. These included a daily curated literature review available by email digest (FLARE),3,4 and a library of digital content including didactics, chalk talks and procedural videos (CURVE).5
Additionally, consensus critical care COVID-19 management guidelines were developed6,7 – with input from CICU cardiologists with expertise in cardio-oncology and novel therapeutics, heart failure and cardiomyopathy, genetics, electrophysiology and critical care cardiology – and updated on the internet. MGH CICU physicians participated in reports on critically ill COVID-19 patients published in the New England Journal of Medicine.8,9
On the Vanguard: CCCs
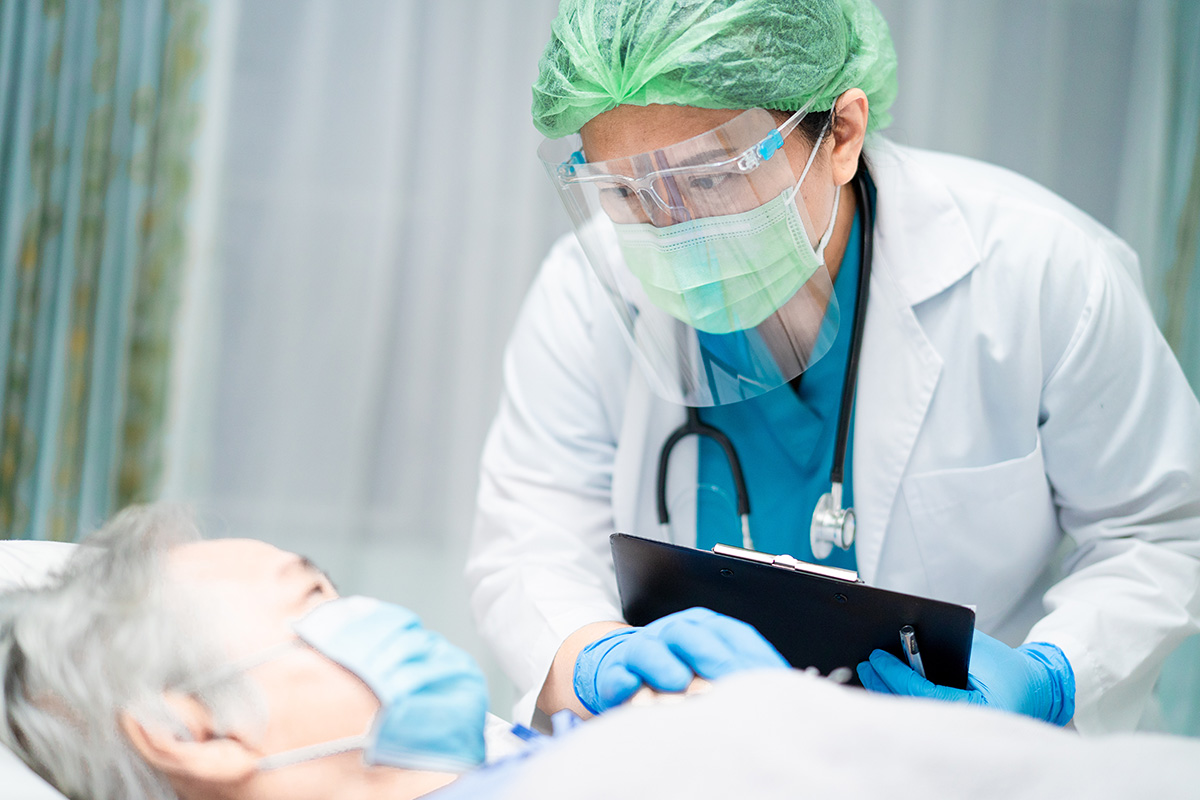
Although the initial critical care surge of COVID-19 in the Boston area subsided by June, the importance of planning for second and subsequent COVID-19 surges, as well as future pandemics and critical care capacity disasters, was imprinted on critical care cardiologists.2
There are nearly 200 such cardiologists in the U.S. – including five on staff at MGH – who also trained in and are formally certified in critical care medicine. Such dual-certified critical care cardiologists are at the vanguard of changes locally, and nationwide, of caring for patients with primary cardiovascular diagnoses complicated by critical noncardiac organ dysfunction, and patients with primary noncardiovascular conditions complicated by acute, critical cardiovascular comorbidities.10
Many such patients require expert bedside care at the interface of traditional cardiology and critical care disciplines, such as 24/7 management of novel mechanical circulatory support devices, and close collaboration with cardiac anesthesiologists and cardiac surgeons.
Proust taught that the "true voyage of discovery" is not in visiting new lands – and certainly 2020 qualifies – but to behold the universe through new eyes. Certainly cardiologists' experience with COVID-19 has afforded new, perhaps 20/20, vision of the capability and potential role of critical care cardiologists,1 and thereby strengthened the motivation for formalizing the subspecialty of critical care cardiology.
The College recently hosted a discussion on this topic, and a formal proposal for a new CCC member section is under evaluation. While the proposal suggests that practice at "level 1" CICUs should be driven by critical care cardiologists (or close collaboration between a CICU cardiologist and another intensivist), CICUs of other tiers may have different resources, patient populations and physician needs.
Overall, the proposed CCC section and philosophy is designed to be inclusive of all cardiologists who practice acute cardiac care, as well as fellows in training, and our colleagues from surgery, anesthesiology, emergency medicine and pharmacy.
References
- Katz JN, Sinha SS, Alviar, et al. J Am Coll Cardiol 2020;76:72-84.
- Anstey DE, Givens R, Clerkin K, et al. Am Heart J 2020;227:74-81.
- Mass General FLARE Fast Literature Updates. Available here.
- Petri CR, Brenner LN, Calhoun TF, et al. ATS Scholar 2020;1:186-93.
- Mass General COVID-19 Urgent Resource Video Education (CURVE). Available here.
- MGH Treatment Guide for Critically Ill Patients With COVID-19. Infographic available here.
- Chivukula RR, Maley JH, Dudzinski DM, Hibbert K, Hardin CC. J Intensive Care Med 2020;Oct 28:[Epub ahead of print].
- Kazi DS, Martin LM, Litmanovich D, et al. N Engl J Med 2020;382:2354-64.
- Newton-Cheh C, Zlotoff DA, Jung J, et al. N Engl J Med 2020;383:475-84.
- Dudzinski DM, Januzzi JL Jr. J Am Coll Cardiol 2017;69:2008-10.
Clinical Topics: Cardiovascular Care Team, COVID-19 Hub, Heart Failure and Cardiomyopathies, Acute Heart Failure
Keywords: ACC Publications, Cardiology Magazine, COVID-19, Critical Illness, Shock, Cardiogenic, Extracorporeal Membrane Oxygenation, Teaching Rounds, Triage, Anesthesiology, Pandemics, Electronic Mail, Pulmonary Heart Disease, Respiratory Distress Syndrome, Fellowships and Scholarships, Motivation
< Back to Listings


